Keywords: COVID-19, head injury, athletes
In this blog we will detail how we found that high school athletes that contracted COVID-19 were over three times more likely to have a concussion following return to sport, compared to their fellow high school athletes. Our study (recently published in BJSM) was a grassroots initiative, spurred by sports physicians covering high school sport, throughout the ATI Physical Therapy network (1). Sports physicians anecdotally were noticing that athletes returning to sport from COVID-19 were more likely to suffer a concussion. Due to these ongoing community conversations, a research initiative was enacted to evaluate this particular important sports medicine question. A consortium between ATI Physical Therapy sports medicine team, consisting of physicians, athletic trainers, physical therapists, and leadership, in partnership with clinical epidemiologists from the Department of Orthopaedic Surgery & Rehabilitation at Wake Forest University School of Medicine, Sport Injury Prevention Research Centre at the University of Calgary, and the Pharmaco- and Device Epidemiology Unit at the University of Oxford was created to perform this study.
Why is this study Important?
Concussions in high school athletes are a serious problem. Almost 20% of all adolescents in the United States report experiencing a concussion during high school . High school athletes may be at higher risk for sustaining a concussion compared to adult athletes.
Coronavirus (COVID-19) infections have impacted adolescent health, long after acute COVID-19 has resolved. Adolescent athletes report a high rate of symptoms resultant from COVID-19, including multisystem inflammatory syndrome. Further, COVID-19 may affect the neurological system, potentially impairing cognitive processes (2).
Concussions have important repercussions in adolescent and high school athletes, due to their growing brains. While COVID-19 infection rates have been quantified, we do not know the potential consequences of long-term COVID-19 symptoms in adolescents, as they return to high school sport. Understanding the interplay between COVID-19 and concussion rates as high school athletes return to sport could potentially improve clinical examination, decision making, and athlete and parent education.
How did the study go about this?
A prospective study over one academic year was performed to evaluate concussions rates in high school athletes that contracted COVID-19 and those that did not. All illnesses and concussions were recorded by athletic trainers over the six state ATI network.
What did this study find?
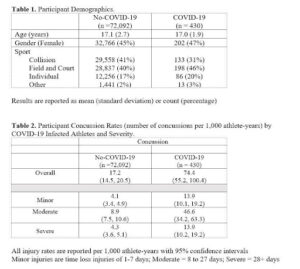
A total of 72,522 athletes participated in high school sports during the 2020-2021 academic school year. A total of 1,273 concussions (No-COVID-19: 1,241; COVID-19: 32) were documented during the school year. High school athletes who sustained a COVID-19 infection demonstrated over a three times [3.1 (95% CI: 2.0, 4.7), p < 0.001] greater rate of concussion compared to high school athletes that did not contract COVID-19. See Table 1 for more details.
What are the key take home points?
- Athletes with COVID-19 infection had greater than 3-fold rates of concussion within sixty days following recovery from infection compared to athletes without COVID-19 infection.
- Further research is warranted to explore why athletes with a recent COVID-19 infection are at higher risk of concussion.
- Clinical judgement or concern may guide further evaluation or a more cautious return to sport in athletes recovering from COVID-19.

References:
(2) De Sousa RAL, Improta-Caria AC, Aras-Júnior R, de Oliveira EM, Soci ÚPR, Cassilhas RC. Physical exercise effects on the brain during COVID-19 pandemic: links between mental and cardiovascular health. Neurological Sciences. 2021;42(4):1325-1334.
Authors and Affiliations:
Garrett S Bullock, PT, DPT, DPhil1,2,3 Carolyn A. Emery, BSPT, PhD,4,5 Vicki Nelson MD,6 Albert Prats-Uribe, MD, MPH, FFPH,7 R. Gil Gilliand, ATC,8 Charles A Thigpen ATC, PT, PhD,8,9 Ellen Shanley PT, PhD, OCS8,9
1 Department of Orthopaedic Surgery & Rehabilitation, Wake Forest University School of Medicine
- Department of Biostatistics & Data Science, Wake Forest University School of Medicine
- Centre for Sport, Exercise and Osteoarthritis Research Versus Arthritis, University of Oxford
- Chair Sport Injury Prevention Research Centre, Faculty of Kinesiology and Pediatrics and Community Health Sciences, Cumming School of Medicine, University of Calgary, 2500 University Dr. NW, Calgary, Alberta, T2N1N4, Canada
- Sport Injury Prevention Research Centre, Faculty of Kinesiology, University of Calgary, 2500 University Dr. NW, Calgary, Alberta, T2N1N4, Canada
- PRISMA Health, Greenville, South Carolina.
- Pharmaco- and Device Epidemiology, Centre for Statistics in Medicine, Nuffield Department of Orthopaedics, Rheumatology, and Musculoskeletal Sciences, University of Oxford
- ATI Physical Therapy
- University of South Carolina Center for Effectiveness Research in Orthopedics
Email contact: gbullock@wakehealth.edu