Part of the BJSM’s Young Clinician Blog Series
Shoulder injuries. A dread for many physiotherapists and a delight for a few of us less sane. A person with a shoulder injury often presents with a lot of complexity – this is a challenge I tend to relish. What follows is a story of my battle managing a personal experience of recurrent shoulder instability and the lessons it has taught me as a physiotherapist.
My journey began in 2020, aged 25.
I returned home after six months of living my dream of surfing around Indonesia with my partner. I got back into skateboarding, and I can assure you concrete is much harder than water when you fall. I fractured my right radial head after landing on my outstretched arm. Shortly after my arm healed, I started playing touch rugby. Now, unfortunately, my injuries didn’t stop there. Over the coming weeks, I experienced three separate incidences of traumatic shoulder instability that prevented me from continuing activities I enjoyed. 
I understand that shoulder instability has high recurrence rates within a season, and various research reports a 37-90% re-injury rate [1]. I had stubborn high hopes to make my goal of returning to playing rugby union. The season was only three months away, and my options were:
- Surgery – six months off work, no rugby and no surfing.
OR
- Conservative – No time off work, continue surfing and start non-contact preseason training and potential safe return to play.
Aside from surgery, there is a lack of consensus for best management for return to play post-shoulder dislocation, but for the next 12 weeks, I modified activities to be pain-free. I worked hard to gain equal shoulder strength and to be confident with rugby-specific actions [2]. Despite a hint of worry playing on my mind, I felt great. I was prepared for the season’s first game, starting at half-back. I was making tackles, had no concern running the ball into contact, and even scored a try! In the match’s final minutes, I dived to make a direct tackle, and I made contact with my right arm outstretched into abduction. Bang!
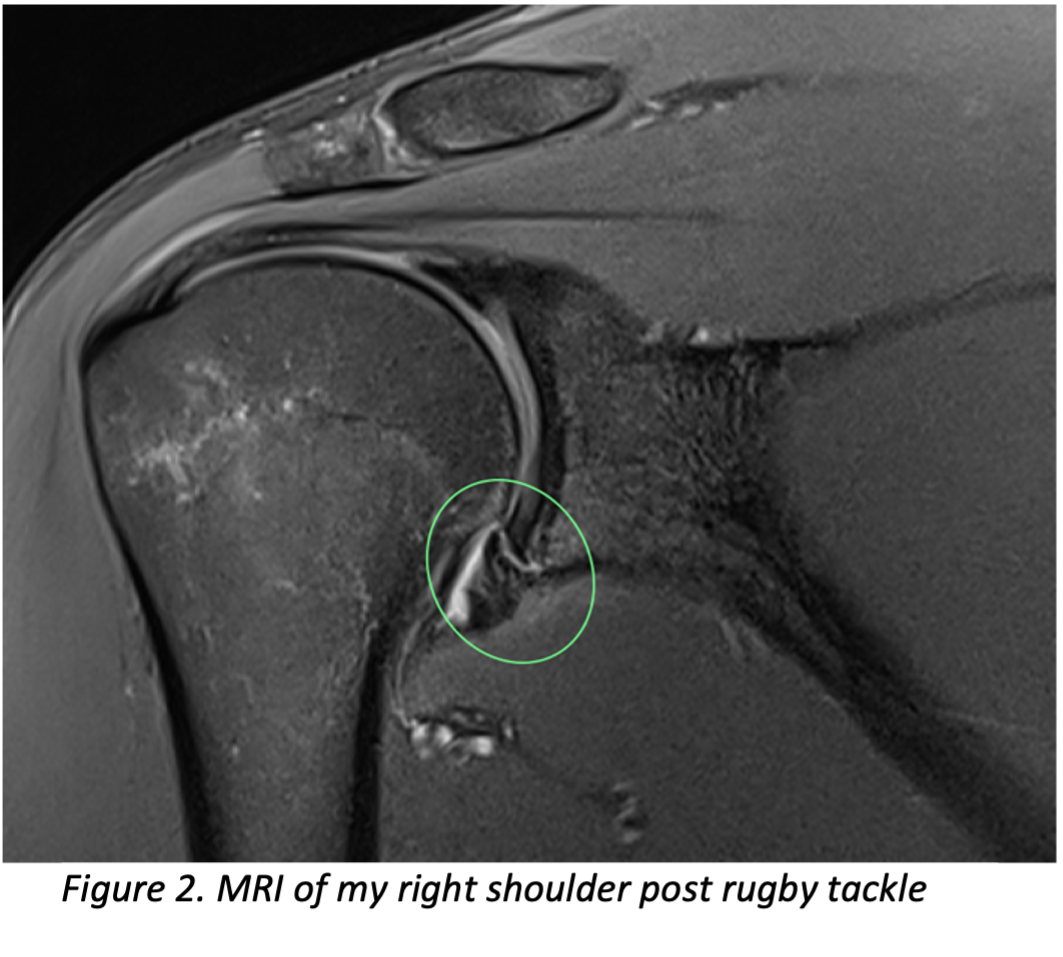
Back to square one, I stopped playing rugby but continued with gym and non-contact training. I had a consultation with a surgeon and opted for surgery, but due to work commitments, that had to wait. Non-surgical treatment can be effective for around 60% of people [3], but unfortunately, I began experiencing instability more frequently and felt more fearful each time. I lived through the experience of the impact of this injury, both physically and psychologically. Emotions and behaviours change drastically as we progress through an injury. Our negative thoughts relate to how severe we suspect the injury to be and its impact on our lives. For shoulder instability, this is also a predictor of recurrence [3]. Our progression through the rehabilitation leads to frustration, and finally, as we begin the return to play process, the fear of re-injury may become more apparent as we reflect on our past events [4].
Reflection
So here I am, nearly two years post-injury, now ten weeks post-op with newfound confidence to return to play. It has been a valuable lesson that will continue to develop with my career. Here is a quick summary of what it has taught me:
- Education is essential
- Injuries are scary. Even scarier for our patients with little knowledge
- Life continues around you when you are injured, while part of your life may feel as though it is on halt. A person with this injury may not be able to undergo a specific intervention (e.g. surgery) at a preferred time, even if it is the best option
The best we can do as therapists is to understand our patients’ goals and perspectives to guide them to regain strength and function to survive and encourage and educate them to thrive.
Author and Affiliations:
Mitchel Versey
Physiotherapist at Motion Health Group, Auckland, and currently undertaking a Post-graduate Diploma in Sports Physiotherapy at the School of Physiotherapy, University of Otago, New Zealand.
No competing interests
References:
1 Watson S, Allen B, Grant JA. A clinical review of return-to-play considerations after anterior shoulder dislocation. Sports Health 2016;8:336–41. doi:10.1177/1941738116651956
2 Griffith R, Fretes N, Bolia IK, et al. Return-to-sport criteria after upper extremity surgery in athletes—A Scoping Review, Part 1: Rotator cuff and shoulder stabilization procedures. Orthopaedic Journal of Sports Medicine 2021;9:23259671211021828. doi:10.1177/23259671211021827
3 Olds MK, Ellis R, et al. Who will redislocate his/her shoulder? Predicting recurrent instability following a first traumatic anterior shoulder dislocation. BMJ Open Sport & Exercise Medicine 2019;5. doi:http://dx.doi.org.ezproxy.otago.ac.nz/10.1136/bmjsem-2018-000447
4 Clement D, Arvinen-Barrow M, Fetty T. Psychosocial responses during different phases of sport-injury rehabilitation: A Qualitative Study. Journal of Athletic Training 2015;50:95–104.