By James Ross Bailey
During the first two years of medical school, students are taught physical exam maneuvers by either practicing on each other or by using Standardized Patients (SPs). These SPs are paid actors that act out a variety of medical conditions. They play an important role in medical education. But, what SPs cannot do is accurately reproduce physical exam findings. For instance, it would be impossible for even the Denzel Washington of SPs to accurately produce the laxity of a knee with an ACL tear.
As third- and fourth-year medical students, we are expected to use the physical exam skills learned during the first two years to accurately diagnose patients in the clinical setting. The question that frequently plagued me throughout these years, however, was: how am I supposed to know if that test is positive if I’ve never felt a true positive to compare it to? It was this question that led me to my last three years of research evaluating the effectiveness of soft-embalmed cadavers for identifying positive physical exam findings.
The Thiel Method: a soft-embalming technique
The cadavers used in this research underwent an innovative soft-embalming technique known as the Thiel method, which allows for better preservation of muscle tissue and joint range-of-motion. Preserving the cadaver’s range-of-motion allows us to perform diagnostic physical exam maneuvers that would be impossible on traditional cadavers.
The diagnostic test first used to evaluate the effectiveness of these Thiel-embalmed cadavers for physical exam instruction was the Lachman exam. The Lachman exam is the most sensitive test for the diagnosis of ACL rupture.
My research: how effective are soft-embalmed cadavers?
Four cadavers were used for this project. Using an incision in the posterior popliteal fossa, two of the cadavers were given ACL tears, one was given a PCL tear, and one was subjected to a sham incision. Fifty-four first year students from East Tennessee State University’s (ETSU’s) Quillen College of Medicine and ETSU’s Department of Physical Therapy were given a brief lecture on proper technique for the Lachman exam prior to testing and completed a seven-question pre-survey regarding their self-perceived ability to diagnose an ACL tear using the Lachman exam.
After testing, all students completed a brief post-survey to evaluate the effectiveness of this instructional method.
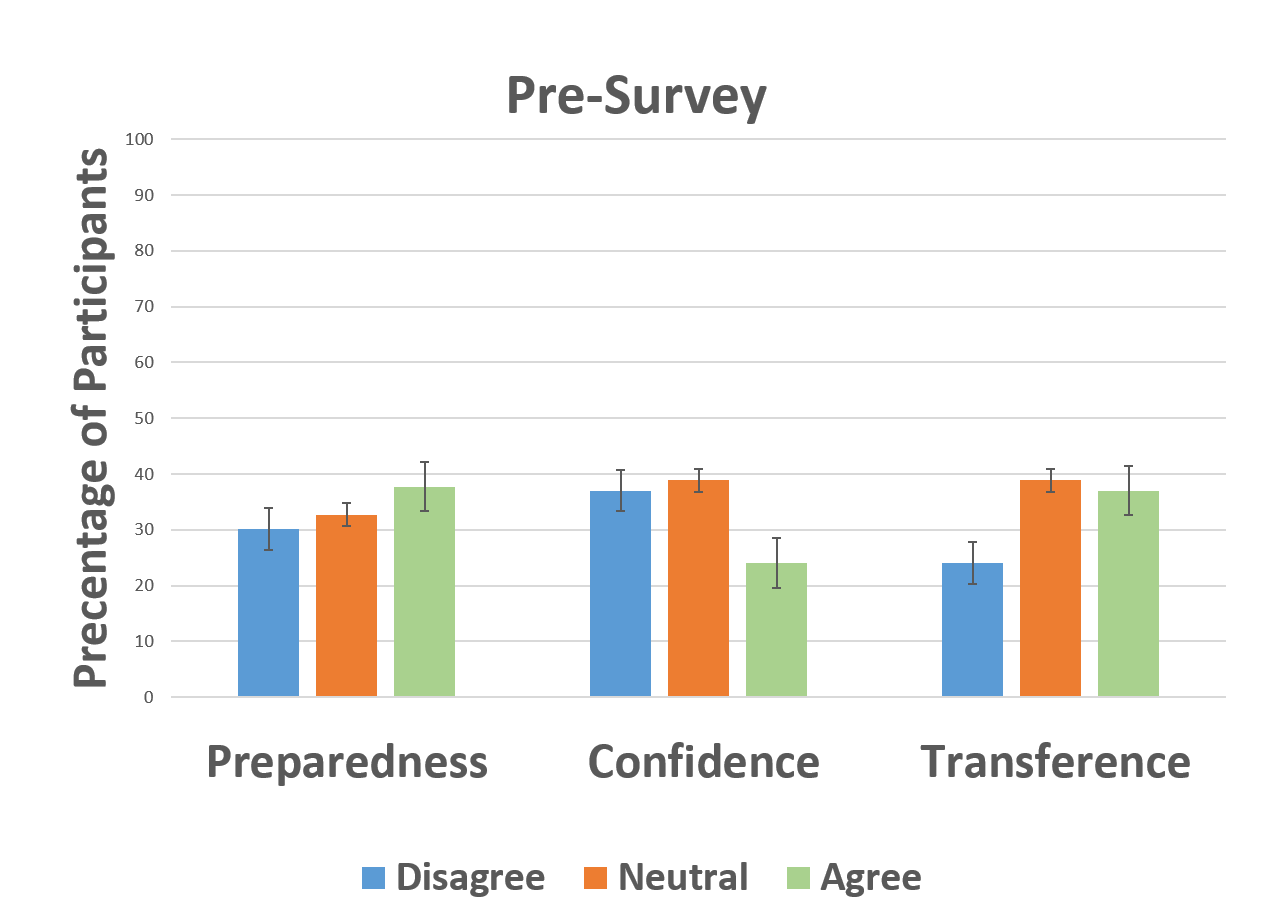
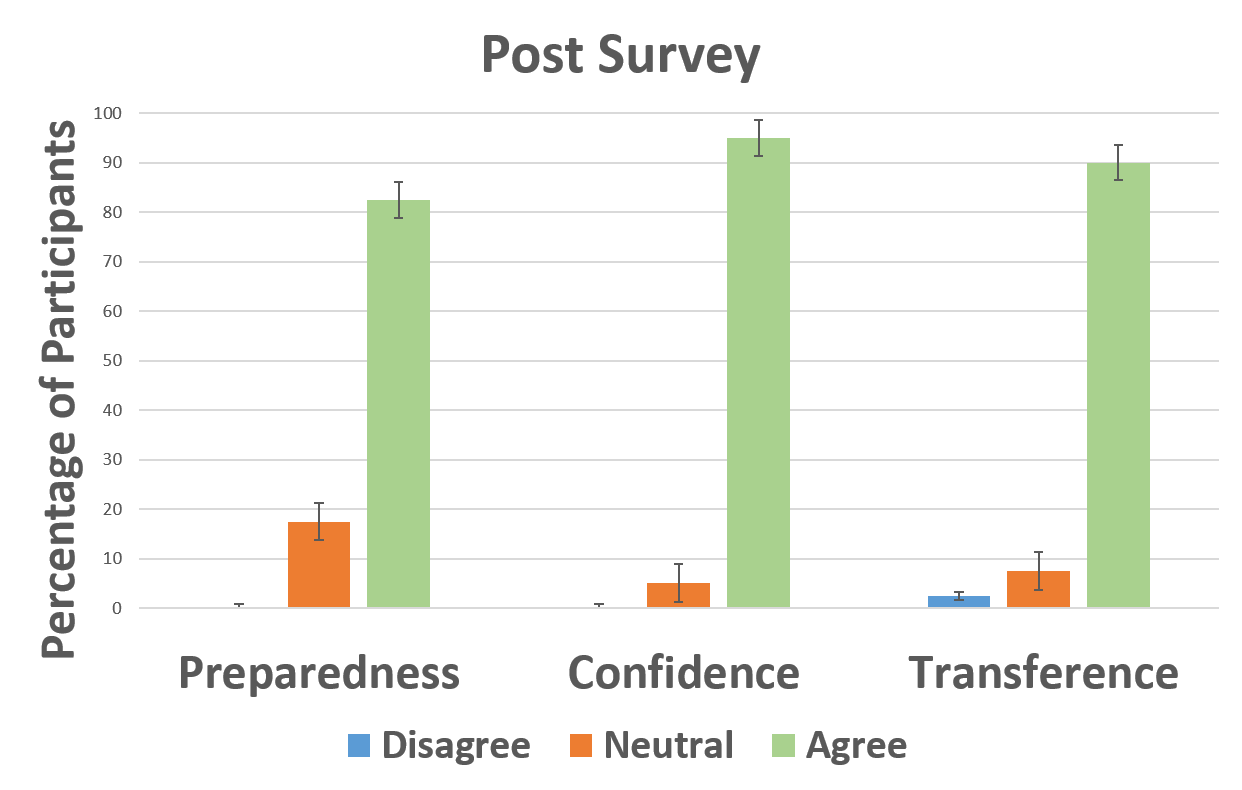
Results were overwhelmingly positive. 1) 90% of participants preferred using Thiel-embalmed cadavers in addition to SPs. 2) 95% of participants indicated on the post-survey compared to 24% on the pre-survey that they now feel confident performing the Lachman exam on a real patient. 3) 82.5% of participants indicated on the post-survey compared to 37.7% on the pre-survey that they now feel prepared to perform a Lachman test during a clinical evaluation. 4) 90% of participants indicated on the post-survey compared to 37% on the pre-survey that they believed the skills learned during the session are easily transferrable to patient care. 5) 100% of experimental group participants indicated that the Thiel cadavers enhanced their Lachman examination technique.
My conclusion
The Thiel-embalmed cadavers are a valuable training resource for both medical and physical therapy students. These cadavers enhance student confidence, increase student preparedness to perform the exam during a clinical evaluation, improve Lachman exam technique and consequently future diagnostic capabilities.
This study has already led to curriculum changes at my medical school. It identifies the need to incorporate training aids that allow students to identify positive versus negative exam findings. Medical and physical therapy students should be able to distinguish between a positive versus negative test result upon starting formal clinical rotations. The research supports the hypothesis that Thiel-embalmed cadavers serve as one of the few training aids available to address this apparent gap in pre-clinical medical education curriculums.
Special thanks to Rob Becker, Dr. Kyle Boden, Dr. Brian Johnston, and Dr. Tom Kwasigroch for their work on this project.
***
James Ross Bailey is a fourth-year medical student at East Tennessee State University’s Quillen College of Medicine. He is pursuing a career in orthopaedic surgery. Email: baileyjr1@etsu.edu