By Daniel Friedman @ddfriedman
BJSM would like to thank The Swiss Sports Physiotherapy Association (SSPA, Sportfisio) and the Swiss Sports Medicine Society (SSMS) for joining forces to deliver a world class, sold out conference that took place on 15-16 November 2018 in Bern. For two days, over 800 attendees were treated to a stellar line-up of speakers to hear about the latest in the world of hip- and groin-related pain, load monitoring and recovery.

If you were not able to make it to Bern, don’t worry – we have you covered! And in addition to this blog, you can also check out the highlights from the conference on Twitter #SportSuisse2018.
Day 1
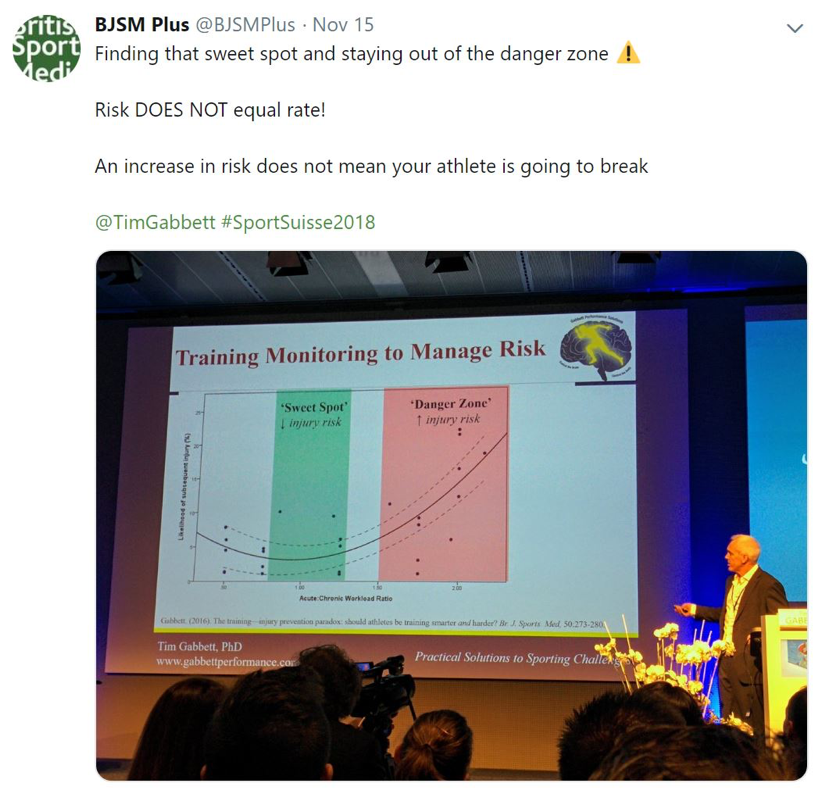
The first session of the day focused on load monitoring, and who better to open proceedings than Dr Tim Gabbett PhD @TimGabbett? Tim introduced the audience to the Acute: Chronic Workload Ratio (ACWR) and questioned whether there is an “optimal load”? Some key messages from his presentation included:
- Risk of injury ≠ rate of injury, but risk of injury increases with spike in acute workload (ACWR of ≥1.5 [on average]), which is influenced by “moderators” such as aerobic fitness, strength, age and high chronic training load.
- Athletes must prepare for the worst-case scenario: “If you train for the average demands, you will only be prepared for 50% of the game”.
- Monitoring alone will not reduce injuries; physically hard and appropriate training reduces injuries.
Dr Franco Impellizzeri PhD @francoimpell followed with a critique of the ACWR and took us on a whirlwind tour of the literature on training load from the past 30 years. Franco ended his presentation with a warning for researchers regarding prediction and an urgent need to prevent misinformation, especially when broadcasting findings via social media.
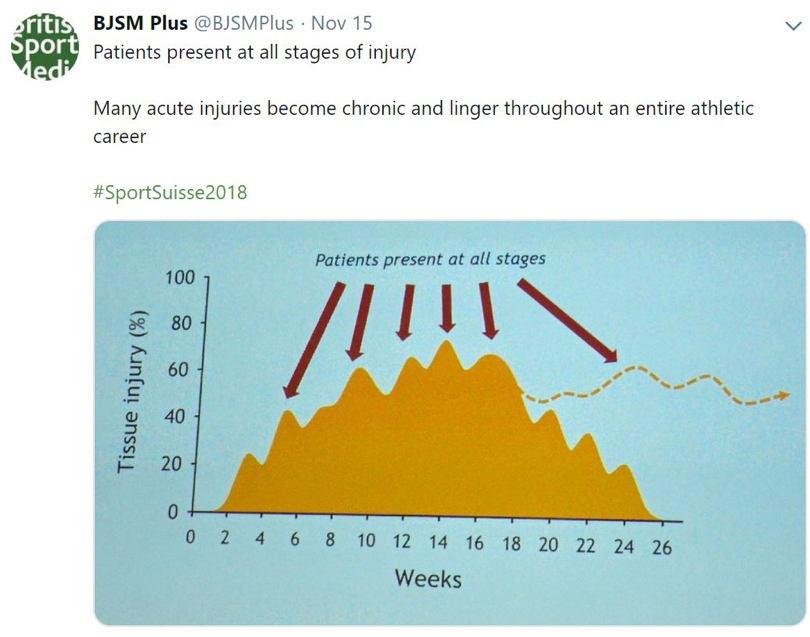
Dr Havard Moksnes PhD @hmoksnes and Dr Mick Drew PhD @_mickdrew examined the burden of overuse injuries and overuse injuries’ relationship with training load.
- Management of overuse injuries:
- Reduce load on tissues
- Increase load tolerance
- Reintroduce sport-specific demands
- Large increases in relative or absolute workloads are necessary but not solely sufficient cause of overuse injuries. Sufficient meaning not a single factor, but a minimum set of factors and circumstances that together produce injury.
For a change of pace, Dr Mike Reiman PhD @MikeReiman provided a brief overview of the workup of FAI syndrome.
- Current hip examination tests for FAI lack diagnostic accuracy and clinical utility.
- FAI surgery (mostly done in US + Switzerland) allows RTP, but what does it take to achieve a return to the same level of performance?
Dr. Joanne Kemp PhD @JoanneLKemp rounded out the morning session by speaking about conservative management for FAI, explaining that physios have the ability to influence the intrinsic and extrinsic factors that contribute to the syndrome.
- There is no level 1 RCT on physio-led treatment of FAI, but treatment should follow an impairment-based model, focusing on hip and trunk strength, function/plyometric/balance training, movement retraining, cardiovascular training, education.
- Impact of FAI on quality of life, activity and sport is enormous, with increased risk of end stage hip osteoarthritis and total hip arthroplasty.

Dr Rintje Agricola PhD @RintjeAgricola commenced the afternoon session by speaking about the influence of athletic activities during growth on hip development.
- Cam morphology develops around the age of 13 (period in which bones are most responsive to exercise – remember that bones are adaptive!)
- Type and frequency of athletic activities during adolescence influence cam morphology.
Dr. Per Hölmich @PerHolmich spoke about the evolution of groin pain diagnosis and treatment.
- The most common complaint with hip-related problems is groin pain. Anatomy is key to diagnosis and treatment of groin pain.
- The Copenhagen adductor exercise is a great addition to the exercise program for FAI.

Dr Kristian Thorborg PhD @KThorborg presented on managing hip and groin problems in team sports.
- Identify groin issues as early as possible. Screen not to predict but to detect already existing problems.
- The Copenhagen five-second squeeze test is a valid indicator of sports-related hip and groin function.
Dr Andrea Mosler PhD @AndreaBMosler explored the risk factors for and prevention of groin pain in athletes.
- Consider primary, secondary and tertiary prevention when approaching injuries. Upstream prevention for all is time and money well spent!
- Criterion-based rehab for groin pain should include: determining impairments, determining exercise progressions based on outcome measures, sensitive pain provocation tests to determine load progression.
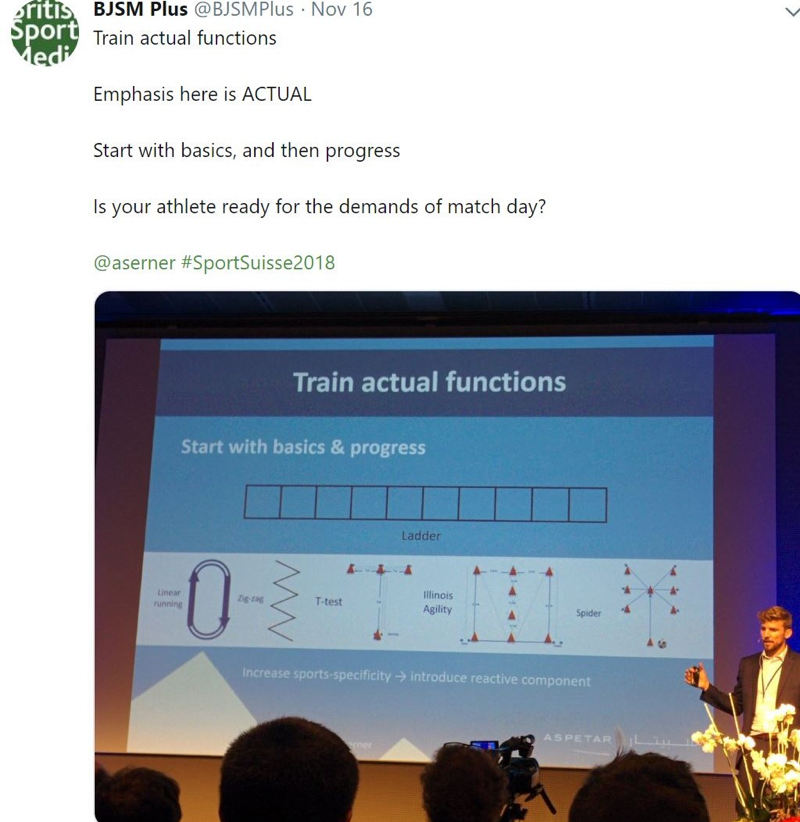
Dr. Andreas Serner PhD @aserner was the lucky last for Day 1, and left the audience with some guiding principles for rehabilitation of groin injuries.
- Focus on the athlete’s sport requirements and what elements are likely to cause pain for that athlete.
- Isolate weakness to then improve strength. Train through pain up to 2/10, rest, and repeat. Graduated return to play is key.
Videos of the presentations from the conference can be viewed at:
Sportfisio Swiss Youtube
Sportfisio Swiss 2018 Conference website
Sportfisio Swiss Facebook
Sportfisio Swiss Twitter
To read about Day 2, check out Part 2 of this blog here.
***
Daniel Friedman @ddfriedman is a final year medical student at Monash University in Melbourne, Australia. He is currently based in Vancouver, working for the BJSM as an associate editor, and has previous experience working for the WHO, focusing on the prevention of noncommunicable diseases and the promotion of active healthy lifestyles. Daniel’s interests span physical activity and public health, injury prevention, and nutrition. Email: ddfriedman@gmail.com.
Competing interests
None