By Drs. Vadim N. Dedov and Irina V. Dedova
ABSTRACT
Background/Aim – Beneficial health effects of regular physical activity and exercise are well established. However, a variety of exercise types and modes complicates quantification of physical activity. Introduction of a single parameter for the objective measurement of exercise amounts might facilitate exercise prescription in primary care practice.
Methods – A novel exercise device with a friction resistance mechanism was equipped with a temperature sensor to measure heat production during the exercise. Heart rates were monitored with a fingertip pulse oximeter. Four healthy volunteers participated in this study.
Results – Heat production in the device during an exercise bout was used as a measure of exercise amount. An individual amount of device usage was determined in the respective fitness test and prescribed according to the current recommendations for daily physical activity. Automatic daily recordings showed significant variations in exercise intensity and duration in unsupervised conditions, but the prescribed amount of exercise has been exceeded on most days and weeks, indicating a full adherence to the exercise prescription. Upon completion of a three-month exercise prescription daily exercise amount was adjusted according to a new fitness test.
Conclusion – This study demonstrated for the first time that amount of physical activity can be calculated as a single parameter of exercise device usage. The results suggest that a personal amount of exercise can be determined and prescribed, and that adherence can be objectively monitored on regular basis.
INTRODUCTION
Medical research has demonstrated that regular physical activity has a significant preventive and therapeutic effect.1 Nevertheless, the implementation of exercise recommendations and guidelines is not effective, especially in general practice.2 It was shown that ‘considerable uncertainty remains as to the effectiveness of exercise referral schemes for increasing physical activity, fitness, or health indicators, or whether they are an efficient use of resources for sedentary people with or without a medical diagnosis’.3 It might be argued that in order to improve efficiency of exercise prescription it should be: (i) personalised and hence based on the assessment of patients’ fitness level,4 (ii) expressed in well-defined doses and (iii) followed by objective monitoring of compliance.
However, current methods for quantification of individual fitness levels and exercise amounts might be too complex for routine application. For example, the maximal oxygen consumption (VO2max) is considered a gold standard for assessing cardiorespiratory fitness, but respective VO2max protocols are not always feasible for many reasons, including limited time and staff, participant burden, possible medical oversight, costly equipment, and difficulty obtaining a maximal effort.5 Quantification of physical activity is also challenging because it takes many forms and varies in type, intensity, duration and frequency.6 It is a common practice to base the assessment of physical activity on self-reporting, which is prone to measurement error and can lead to incorrect inferences about physical activity behaviours.7 It was shown that healthy adults overestimated energy expenditure during exercise by 3-4 folds.8 Exercise-induced energy expenditure can be measured objectively, but it requires sophisticated equipment and complex technologies.9
Here, we report the development of a feasible approach for personalized exercise prescription, which might be suitable for wide implementation in primary care practice and for use in medical research.
METHODS
A novel resistance exercise device MedExercise® ST (MDXD Pty Ltd, Australia) was used in this study (Figure 1A). Changes of temperature in the resistance unit were measured with a temperature sensor connected to the industrial multimeter IP57 (Digitech, Australia). Data was collected using respective software Multimeter V1.0 from Digitech and then converted into Excel databases (Microsoft, U.S.A.) for analysis. The average exercise-induced rise in temperature was calculated after subtraction of ambient temperature values. A fingertip pulse-oximeter CMS-50E (Contec, China) and corresponding SpO2 Review software were used for the continuous measurement of heart rates during the exercise. Overall, four healthy volunteers, aged between 36 and 49 years, participated in this study. Respective informed consents were obtained. Statistical analysis was performed using the Student’s t-test.
RESULTS
We hypothesised that the amount of exercise device usage achieved by the participant at particular intensity and duration would reflect participant’s level of fitness and could be used as the personalised amount of daily physical activity. MedExercise device was chosen for this study because it allowed continuous monitoring the intensity of usage through the measurement of exercise-induced rise of temperature in the friction resistance mechanism. During exercise the user repeatedly extended and flexed legs by moving foot platforms against graded resistance to their movement (Fig. 1A). Friction between the rails and foot platforms caused fast rise of temperature in the resistance mechanism, whereas stopping of exercise results in drop of temperature to pre-exercise level (Fig. 1B). Conversely, a total amount of device usage during the exercise bout correlated with the amount of heat produced in the resistance mechanism. The latter was reflected by an area under the curve and calculated by multiplication of an average exercise-induced rise in temperature and duration of recording in seconds.
For quantification of daily exercise amounts we used the current physical activity guidelines, which stated that: ‘all healthy adults aged 18 to 65 years need moderate-intensity aerobic (endurance) physical activity for a minimum of 30 min on five days each week or vigorous-intensity aerobic physical activity for a minimum of 20 min on three days each week’.10 The definition of exercise intensity in literature varies considerably,11 but a heart rate of 100 beats per minute (bpm) might be assumed as an indicator of moderate physical activity for most healthy adults, whereas 120 bpm usually indicates a vigorous level of exercise. Therefore, usage of exercise device by the participant at 100 bpm for 30 minutes or at 120 bpm for 20 minutes would represent a recommended daily exercise amount according to the physical activity guidelines.10
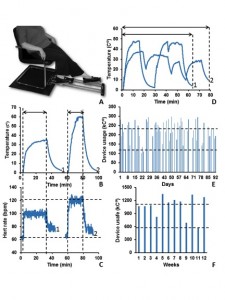
Figures 1B represent a typical recording of temperature in the MedExercise device during moderate (trace 1) and vigorous (trace 2) exercise bouts, as monitored by respective heart rates (Fig. 1C), where a higher intensity of exercise caused temperature rise to the higher level (Fig. 1B). The respective amounts of device usage were calculated and expressed in kilo C⁰ (kC⁰). The amount of exercise at vigorous intensity was higher than during moderate physical activity: 139.5+16.4 kC⁰ and 113.8+7.9 kC⁰ (n=3, P<0.05), respectively. However, since the moderate intensity of exercise was better tolerated, the personal amount of 113.8 kC⁰ daily exercise was selected for the prescription. Therefore, according to the current physical activity guidelines,10 a personalised exercise prescription for this participant was: a minimum of 113.8 kC⁰ x 5 days per week = 569 kC⁰ weekly for three months of MedExercise device use.
Figure 1D exemplifies the patterns of device usage in unsupervised conditions during the exercise prescription. It was shown that the intensity and duration of usage varied to a great extent and included breaks (dents in the curve). Figure 1E and 1F shows daily and weekly amounts of device usage, respectively, for the full period of exercise prescription. The device was used for 4.9+1.2 days a week. An average amount of usage was 217.1+56.1 kC⁰ per day and 1067+251 kC⁰ per week. These results indicated that exercise prescription has been administered in full because the usage of device exceeded the prescribed amount. After completion of the three-month exercise prescription, a fitness level of the participant was retested and resulted at 132.7+15.1 kC⁰ (n=3). Accordingly, the next personalised exercise prescription was adjusted to a minimum of 132.7 kC⁰ x 5 days per week = 663.5 kC⁰ weekly of MedExercise device use for the next 6 months.
DISCUSSION
In contrast to prescription of conventional drugs, which are given in the specific doses and regimes, physical activity takes many forms and varieties, making it difficult to standardise.6 We have hypothesised that the amount of exercise device usage could serve as an objective and practical measure of exercise amounts. MedExercise device allowed direct measurement of heat production during the exercise through detection of temperature rise in its friction resistance mechanism. Conversely, the amount of heat produced in the device corresponded to the amount of exercise that participant performed with the device. A total amount of heat production during an each exercise bout depended on the intensity and duration of device usage, and could be calculated as an average rise in temperature multiplied by the durations of exercise. Therefore, a single parameter of heat production incorporated all variability of device usage such as resistance, frequency, duration and presence of breaks.
As a test for validity of our approach, we have determined a daily amount of exercise according to the most commonly used physical activity guidelines10 and selected the amount of device usage at a tolerable moderate intensity for three-month prescription. This exercise prescription was personalised because it was based on individual exercise capacity of the participant. Daily monitoring of device usage provided an objective insight into patterns and amounts of physical activity during exercise prescription. It is an important advantage because commonly used self-reporting is biased and prone to errors.7, 8 It was observed that the patterns of unsupervised exercise varied to a great extent due to fluctuations of intensity, different durations and presence of breaks. However, the amount of device usage consistently exceeded the prescribed daily and/or weekly amounts for the whole period of prescription that indicated a full adherence to exercise prescription and regular physical activity. After completion of previous exercise prescription the fitness test was repeated in order to adjust the dose for the next period of exercise prescription.
The limitation of this study is a small number of healthy participants that necessitates further clinical studies. The strength of our approach includes the measurement of exercise amounts as a single parameter, simplified assessment of fitness levels, personalised exercise prescription and objective monitoring of adherence. It is important that exercise prescription sets only a minimum amount of exercise so that other types of physical activity should be encouraged for better health effects.
References
1. Lucini D, Pagani M. Exercise: Should it matter to internal medicine? Eur. J. Intern. Med. 2011;22:363-70.
2. Weiler R, Feldschreiber P, Stamatakis E. Medicolegal neglect? The case for physical activity promotion and exercise medicine. Br J Sports Med 2012;46:228-32.
3. Pavey TG, Taylor AH, Fox KR, et al. Effect of exercise referral schemes in primary care on physical activity and improving health outcomes: systematic review and meta-analysis. BMJ 2011;343:d6462.
4. Buford TW, Pahor M. Making preventive medicine more personalized: Implications for exercise-related research. Prev Med 2012.
5. Mitros M, Gabriel KP, Ainsworth B, et al. Comprehensive evaluation of a single-stage submaximal treadmill walking protocol in healthy, middle-aged women. Eur J Appl Physiol 2011;111:47-56.
6. Slade SC, Keating JL. Exercise prescription: a case for standardised reporting. Br J Sports Med 2011.
7. Ainsworth BE, Caspersen CJ, Matthews CE, et al. Recommendations to improve the accuracy of estimates of physical activity derived from self report. J Phys Act Health 2012;9 Suppl 1:S76-84.
8. Willbond SM, Laviolette MA, Duval K, et al. Normal weight men and women overestimate exercise energy expenditure. J Sports Med Phys Fitness 2010;50:377-84.
9. Levine JA. Measurement of energy expenditure. Public Health Nutr 2005;8:1123-32.
10. Haskell WL, Lee IM, Pate RR, et al. Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Med. Sci. Sports. Exerc. 2007;39:1423-34.
11. Norton K, Norton L, Sadgrove D. Position statement on physical activity and exercise intensity terminology. J Sci Med Sport 2010;13:496-502.
Figure legend
Figure 1. (A) Position of the participant in the chair, while using MedExercise® device. (B, C) Typical changes of temperature in resistance mechanism of the device (B) and participant’s heart rate (C) recorded simultaneously during the moderate intensity (trace 1) and vigorous (trace 2) exercise bouts. Double headed arrows indicate duration of actual exercise. (D) Patterns of temperature traces during of unsupervised device use. Dents in the curves represent breaks in device usage. Double headed arrows indicate duration of recording. Background room temperatures were subtracted (all temperature curves). (E) Daily amounts of device usage during the three-month exercise prescription. (F) Weekly amounts of device usage during the three-month exercise prescription. Horizontal dotted lines indicate a single and double prescribed amount of device usage.
Competing interests
Dr Vadim Dedov has a stake in MDXD Pty Ltd, which designed and produced the equipment used in this study.
**********************************************
Vadim N. Dedov, M.D., Ph.D., MDXD Pty Ltd, NSW, Australia
Irina V. Dedova, M.D., Ph.D., School of Medical Sciences, University of New South Wales, NSW, Australia