The ward round is an excellent opportunity for medical education. It is an opportunity to learn about taking a history, examining patients, ordering tests, and making decisions about management. If the person leading the round takes some time with the students and trainees, then they should learn a great deal about clinical medicine.
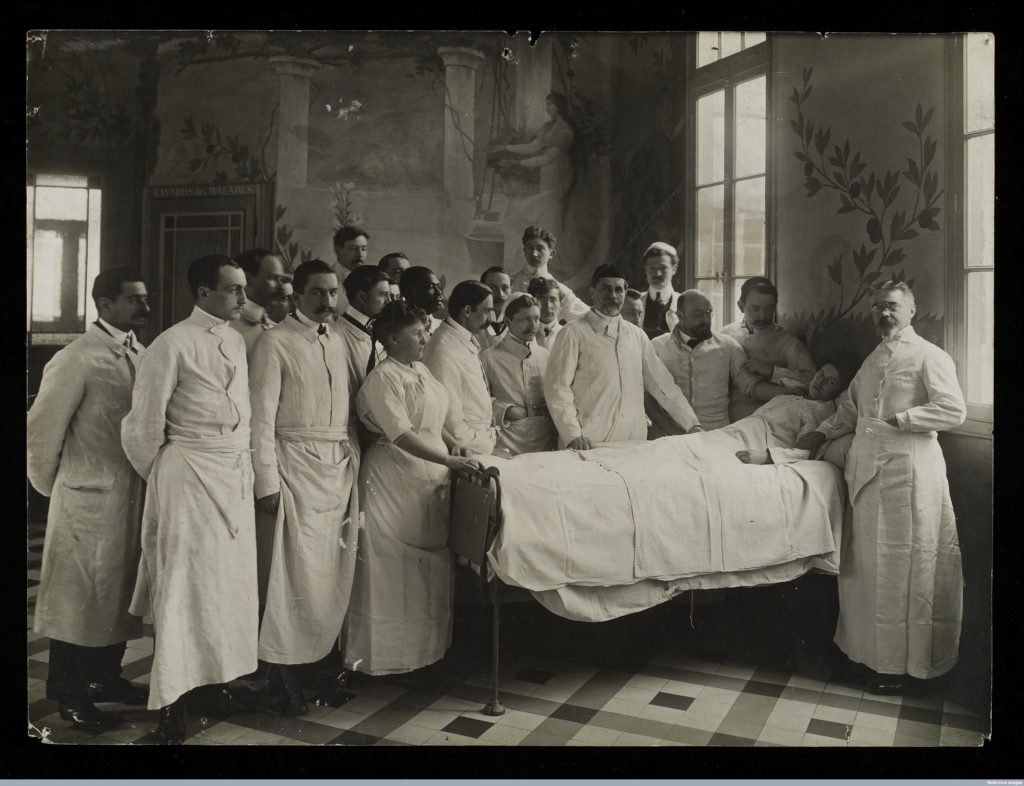
But ward rounds should be primarily patient-centred and it can be hard to fit in both education and clinical care. In the past, ward rounds have sometimes been uncomfortable for patients. It can be intimidating to face a team of clinicians and to answer their questions and sometimes to muster up the courage to ask your own questions. Certainly, the patient in this photograph seems discomfited and worried (1).
The photograph was taken in 1910, but it brings to mind Thomas Bernhard’s comment on the ward round about fifty years later: “every day they appeared in front of my bed a white wall of unconcern”. (2) The number of staff suggests that it might have been a hospital where there was a lot of teaching—but that would be scant comfort to the patient.
Things have improved since 1910—today doctors are more likely to be mindful of the feelings of the patient. However other challenges have arisen in the meantime. Technology in medicine now means that there can be new barriers between the doctors on the ward round and their patient. Doctors have to look at blood results, ECGs, and radiology scans as well as talk to the patient. Sometimes they have to look things up online—if they are unsure of what they should do.
How do patients feel about this? Much depends on the patient and their exact circumstances—but there is some evidence that patients don’t mind their doctors looking things up—a study by Patel et al showed that some of them even feel reassured by this. (3) But it also showed that a great deal depends on context. Patients feel comfortable with junior doctors looking up medications and sometimes think that this is a sign of humility in their doctor as it shows that the doctor knows that they don’t know everything. But they probably wouldn’t feel comfortable with a doctor who had to check more basic things. Patients also wanted the doctor to explain what they were looking up—so they didn’t think that the doctor was being distracted.
This makes me wonder whether we should develop more social rituals around our use of technology in medicine? We use rituals in lots of our other clinical practices. A consultant that I used to work for told me that he always washed his hands slowly and thoroughly in front of his patients. There were lots of sinks in other clinical areas that he could have used, but he wanted to show the patient what he was doing and so ease them into the consultation slowly. The doctor in Steinbeck’s The Pearl made a great play of showing off his medical equipment—as he knew that his patients loved the “the tools of any craft and trust them.”
Should we have other rituals around using our mobile phones to look things up? Healthcare professionals often complain about alerts on their computer screens—that they are a distraction from their patients. But could we turn this on its heads and have different types of alerts.
BMJ Best Practice is our own clinical decision support tool. Should we have an alert on it that says—“If looking things up at point of care, then tell your patient what you are doing”? Or better still—look it up with your patient?
Kieran Walsh is clinical director of BMJ Learning and BMJ Best Practice. He is responsible for the editorial quality of both products. He has worked in the past as a hospital doctor—specialising in care of the elderly medicine and neurology.
Competing interests: Kieran Walsh works for BMJ Learning which provides e-learning resources. He has also written a book on cost and value in medical education.
Photo credit: Wellcome library.
References:
- A crowd of medical staff standing round a woman patient in bed in a hospital ward. Murals of foliage and allegories painted on the walls. Photograph 20th century. By: and Seeberger Freres Published: c.1910. Printed: France Copyrighted work available under Creative Commons Attribution only licence CC BY 2.0, see http://creativecommons.org/licenses/by/2.0/
- Berhard T. (1978) Breath – A Decision. In: Berhard T. (1985) Gathering Evidence. Translated by McLintock, D. Alfred Knopf, New York, pp 240-1.
- Patel R, Green W, Shahzad MW, Larkin C. Use of Mobile Clinical Decision Support Software by Junior Doctors at a UK Teaching Hospital: Identification and Evaluation of Barriers to Engagement. JMIR Mhealth Uhealth.2015 Aug 13;3(3):e80.