Applies to: The FA ATMMiF, The RFL IMMOFP, The FA ITMMiF, Sports Promote, WRU ICIR and The RFU PHICIS
Authors: Lisa Hodgson, Gemma Phillips, Jonathan Gordon, Jonathan Hanson, John MacLean, Prabhat Mathema, Andrew Smith, Mark Woolcock, Charlotte Cowie, Simon Kemp, Michael Patterson, Jo Larkin, Jerry Hill, Mike Rossiter, Niall Elliott, Pippa Bennett, Jonathan Power, Ari Pillai, Harjinder Singh, Craig Sheridan, Matthew Hurwood, Peter Riou, Tony Bennison, Susan Chakraverty, Richard Tingay, Richard Higgins, Richard Weiler, Rod Jaques, Simon Spencer, Jon S Patricos.
Background
COVID-19 is the infection caused by the Novel Coronavirus SARS-CoV-2, first identified in humans in December 2019 and declared a global pandemic by the World Health Organisation in March 2020.
Here we guide pitch side emergency care during the current time of heightened awareness of contracting and transmitting COVID-19. This guidance uses Public Health England (PHE) policy and the staged framework as issued by the UK Government on Return To Training (RTT)[1],[2]. Please refer to any regional or devolved nation-specific guidance as applicable to your area of practice. We attempt to address the potential for adverse clinical outcomes due to the consequences of COVID-19 infection, whilst balancing the risk of exposure to both the casualty and medical response team.
Please ensure you remain up to date with Public Health and government authority guidance on COVID-19 case management, Personal Protective Equipment (PPE) recommendations and RTT. Any update of Resuscitation Council UK (RCUK) or Public Health England (PHE) guidance supercedes the content of this document, this will also be dependent on your region of practice.
Requirements of Elite Sport Organisations in the context of Emergency Care provision
- EnsureCOVID-19 Officer/Managers are appointed and have clearly defined roles in respect of emergency care risk assessment, and updating Emergency Action Plans (EAPs) to reflect this.
- All Health Care Professionals (HCPs) who have opted in to return to work in the sporting environment (training and match venues) must have sight of all EAPs before entering the environment for the first time. It would be advised to consider vulnerable individuals at risk of poorer COVID-19 outcomes[3] and their involvement in potentially high-risk situations.
- Optimal personal and environmental hygienemust be practised at all times by all individuals within the sporting environment, with regular education.
- Adherence to government social distancingrestrictions must be maintained at all times aside from technical training, or with appropriately certified PPE, following thorough situation specific risk assessments.
- Individual sport specific biosecurity measures must be upheldfor all staff involved in the elite sporting environment. At the present time this may include symptom questionnaires, temperature testing, antigen testing and zoning.
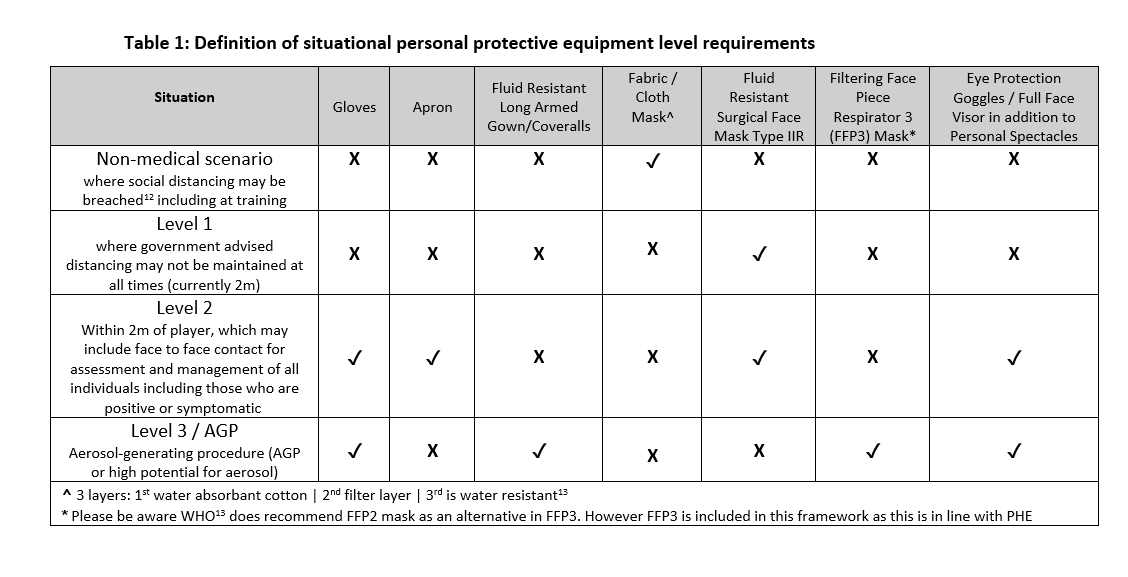
- Appropriate type and quantities ofPPE must be available at all times, including as part of the mandatory emergency medical equipment, to reflect COVID-19 specific safety amendments (see Table 1) that may arise in sport.
- All staff need to be appropriately trained in the correct use and application of PPE[4]. The safe and efficient donning and doffing of PPE should be addressed as part of normal emergency medical protocol breifings and training episodes, including fit testing where appropriate[5]
- Appropriate cleaning products and systematic cleaning protocols implemented after each use of equipment in line with PHE standards[6], or where this is not practical duplicate medical equipment available to prevent delay in case of subsequent need[7]
- Correct disposal of all PPE andcontaminated equipment, as per national clinical waste policy[8]
Personal Protective Equipment precautions
Definition of PPE:
Single Use Items: Equipment that must be changed after each contact. Includes gloves and aprons.
Sessional Use Items: Clothing and equipment worn for a period of time when undertaking duties in a specific clinical care setting or exposure environment; a session ends when the health and social care worker leaves this defined remit; however, it should be disposed of if it becomes moist, damaged or visibly soiled.
Sessional items include: fabric/cloth masks, fluid resistant surgical face masks, filtering face piece respirator (FFP2+3) Masks, eye protection (shield, goggles, visor) and fluid repellent long armed gowns/coveralls. In cases of severe global PPE shortages PHE have made exceptions to facilitate sessional use of equipment, please refer to PHE guidance[9].
Reusable Item: Equipment appropriately decontaminated to PHE standards that can be reused[10]. Includes certain coveralls and eye protection.
Fit-tested Item: FFP masks filter airborne particles and depend on the user creating an air tight seal between their skin and the face seal of the mask[11]. The face fit of each FFP mask will vary according to individual manufacturing. Therefore, each individual requiring use of an FFP mask must ensure they have a mask that is compatible to their face shape. Each mask requires a ‘fit-testing’ process to be conducted to ensure no aerosol leakage occurs through the seal. Facial hair does impact the efficacy of the masks and alternative arrangements may need to be considered in these circumstances.
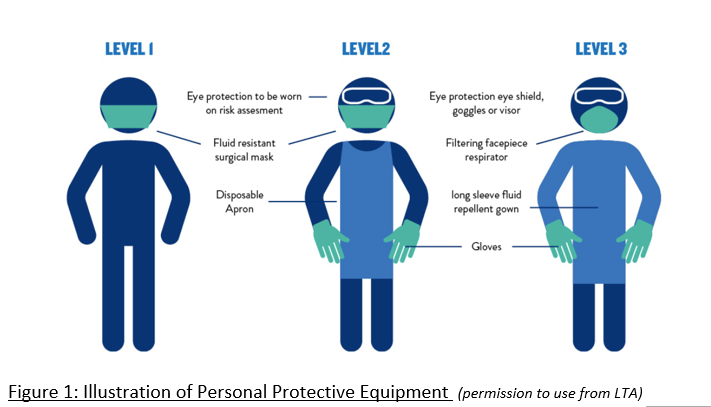
[1] https://www.gov.uk/government/publications/coronavirus-covid-19-guidance-on-phased-return-of-sport-and-recreation
[2] https://blogs.bmj.com/bjsm/2020/05/26/working-with-government-to-plan-a-return-to-sport-during-the-covid-19-pandemic-the-united-kingdoms-collaborative-5-stage-model/
[3] https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/groups-at-higher-risk.html
[4] https://www.gov.uk/government/publications/wuhan-novel-coronavirus-infection-prevention-and-control/covid-19-personal-protective-equipment-ppe
[5]https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/879103/PHE_COVID-19_Donning_quick_guide_gown_version.pdf;
https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/879105/PHE_COVID-19_Doffing_gown_version.pdf; https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/877658/Quick_guide_to_donning_doffing_standard_PPE_health_and_social_care_poster__.pdf
[6] https://www.gov.uk/government/publications/covid-19-decontamination-in-non-healthcare-settings/covid-19-decontamination-in-non-healthcare-settings
[7]https://www.gov.uk/government/publications/wuhan-novel-coronavirus-infection-prevention-and-control
[8] https://www.hse.gov.uk/healthservices/healthcare-waste.htm
[9] https://www.gov.uk/government/publications/wuhan-novel-coronavirus-infection-prevention-and-control/managing-shortages-in-personal-protective-equipment-ppe
[10]https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/877533/Routine_decontamination_of_reusable_noninvasive_equipment.pdf
[11] https://www.hse.gov.uk/news/face-mask-ppe-rpe-coronavirus.htm