Swiss Junior Doctors and Undergraduate Perspective on Sport and Exercise Medicine Blog Series
By Justin Carrard, @Carrard.Justin
I am very honored to launch the new Swiss Junior Doctors and Undergraduate Perspective blog series. This series will help amplify Sport and Exercise Medicine (SEM) as a medical specialty in our country. It will also encourage dialogue and raise awareness about SEM issues, both unique to Switzerland, and global. Topics of interest will likely include: (i) access to ‘hands-on’ learning opportunities (ii) strategies to raise awareness about and implement physical activity in the daily care of patients, (iii) the integration of research and practice.

The Swiss Society for Sports and Exercise Medicine (SGSM) recently held its first Student’s Day in Interlaken1. A diverse lineup of Swiss SEM experts shared their insights. Presenters included: Dr. André Leumann (sports orthopaedic surgeon), Dr. Boris Gojanovic (sports physician), Dr. Patrik Noack (sports physician) and Prof. Matthias Wilhelm (sports cardiologist).
The goal of the conference was to introduce students to key aspects of SEM. I greatly enjoyed the day, and share my 5 take home messages.
Which postgraduate training is the most appropriate to become a sports doctor in a country that does not have SEM speciality?
As explained in the editorial of the recent Swiss BJSM edition1, Switzerland is one of the European countries in which SEM is not yet a speciality. Thus, it could be a bit tricky for medical students to find their way to become a sports doctor. In our country, about 60% of all sports doctors have a general medicine postgraduate training: about 15-20% are orthopaedic surgeons, 10-15% are physiatrists and 10% have another specialty (e.g., paediatrics, cardiology and respiratory medicine). Medical students should then basically decide whether they prefer to work in a practice, in an operating theatre or in a rehabilitation setting. As Dr. Patrik Noack highlighted through fascinating clinical cases, a broad clinical training base (such as the one of a general practitioner) is suitable for somebody who is keen to become a team doctor and work on the sporting fields. While the Swiss training for general medicine enables a lot of rotations in different specialties (additionally to the core training in internal and general medicine), the following areas are recommended: orthopaedics and traumatology, emergency medicine, cardiology, paediatrics or physical medicine and rehabilitation.
Who is consulting a sports doctor practice and why are they doing it?
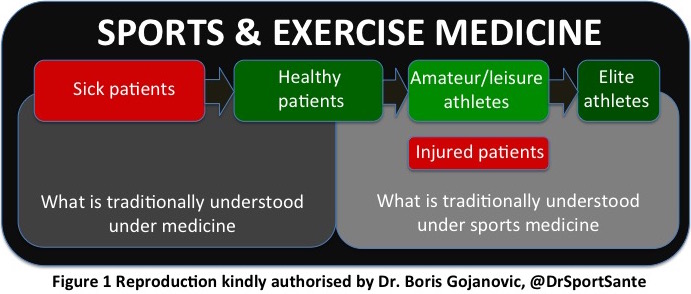
As Dr. Gojanovic explained, most patients currently consulting a sports physician are active ones suffering from musculoskeletal disorders (MSK) or less frequently sedentary people who want to become active and look for counselling. Typically, each sports doctor has some elite athletes among their practice. It is not common in Switzerland that ill patients consult a SEM physician even if mounting scientific evidence points to physical activity’s key role in the treatment of non-communicable diseases (NCDs)2. As pictured in figure 1, SEM is much more than musculoskeletal medicine. SEM offers a great opportunity as a modern way to prevent and treat NCDs.
Is only endurance training useful in reducing the overall mortality?
Health care practitioners often think that endurance training only is the only type of regular physical activity that reduces the overall mortality3. However, as Ruiz et al. showed: “muscular strength is inversely and independently associated with death from all causes and cancer in men”4. Thus, the World Health Organization recommends at least 150 minutes of moderate-intensity aerobic or 75 minutes of vigorous-intensity of aerobic physical activity and muscle-strengthening activities at least twice a week5.
Do elite athletes recover faster from injury than standard patients?
Elite athletes do not heal faster per se compared to standard patients. As young and fit patients, they belong to the left side of a normal (or gaussian) distribution of the needed healing time. Dr. Leumann highlighted that some factors, like nutrition, could be optimized in order to support the healing process. Clinical controls will then be performed more frequently in order to detect as soon as possible a consolidation/healing state compatible with intensive physiotherapy. Thus, although the healing process of elite athletes might not be faster, the injury management is more timely and sophisticated.
Is a left ventricular wall thicker than 12 mm always pathological?
Twelve millimeters thickness is a commonly accepted definition to diagnose left ventricular hypertrophy and consequently suspect hypertrophic cardiomyopathy (HCM) among athletes6,7. However, this criteria was established within white athletes and should be critically reviewed among black athletes, “in whom deaths attributed to HCM are more common”8. Basavarajaiah et al. found that 18% and 3% of black athletes shown left ventricular wall thickness greater than 12mm and 15mm respectively without other cardiac abnormalities9. To conclude, there is potential for false positive HCM diagnosis if physician use the criteria derived from studies among white athletes.
“Together, we reach new heights”1
Forty students participated in this free teaching day around SEM. We heard directly from some of the leading physicians in the country about the many facets and perspectives in the field. The SGSM wishes to engage students and junior doctors to share ideas and motivations to develop the SEM field in a relevant way. In that way, the SGSM invites engagement with its new Swiss Junior Doctors and Undergraduate Sports and Exercise Medicine Society.
*********************
Justin Carrard (@Carrard.Justin) is a first year internal medicine resident based in Biel/Bienne (Switzerland). He is the newly appointed Swiss Correspondent for the brand new BJSM Swiss Junior Doctors and Undergraduate Perspective Blog Series. He is currently implementing the new Swiss Junior Doctors und Undergraduate Sports and Exercice Medicine Society. Justin aims to raise SEM awareness among Swiss medical students and modern solutions it provides to big public health issues like non-communicable diseases. As an ex-competitive swimmer, Justin has a keen interest for endurance sports and regularly practices them with passion.
Email: justin.carrard@gmail.com Twitter: @Carrard.Justin
If you would like to contribute to the “Swiss Junior Doctors and Undergraduate Perspective on Sport and Exercise Medicine” Blog Series please email justin.carrard@gmail.com for further information.
References
- Kriemler, A. Leumann, B. Gojanovic. Together, we reach new heights: Swiss Sports Medicine Society (SGSM/SSMS) joins BJSM Br J Sports Med 2016; 50:1099
- Derman W, Schwellnus M, Hope F, Jordaan E, Padayachee T. Description and implementation of U-Turn Medical, a comprehensive lifestyle intervention programme for chronic disease in the sport and exercise medicine setting: pre-post observations in 210 consecutive patients. Br J Sports Med. 2014 Sep; 48(17): 1316-21.
- Wen CP, Wai JP, Tsai MK, Yang YC, Cheng TY, Lee MC et al. Minimum amount of physical activity for reduced mortality and extended life expectancy: a prospective cohort study. 2011 Oct 1; 378 (9798): 1244-53.
- Ruiz JR, Sui X, Lobelo F, Morrow JR Jr, Jackson AW, Sjöström M et al. Association between muscular strength and mortality in men: prospective cohort study. 2008 Jul 1; 337: a439
- http://www.who.int/dietphysicalactivity/factsheet_adults/en/
- Pelliccia A, Maron BJ, Spataro A, Proschan MA, Spirito P. The upper limit of physiologic cardiac hypertrophy in highly trained elite athletes. N Engl J Med 1991; 324:295–301.
- Sharma S, Maron BJ, Whyte G, Firoozi S, Elliott PM, McKenna WJ. Physiologic limits of left ventricular hypertrophy in elite junior athletes: relevance to differential diagnosis of athlete’s heart and hypertrophic cardiomyopathy. J Am Coll Cardiol 2002; 40:1431–6.
- Maron BJ, Carney KP, Lever HM, Barac I, Casey SA, Sherrid MV. Relationship of race to sudden cardiac death in competitive athletes with hypertrophic cardiomyopathy. J Am Coll Cardiol 2003; 41:974–80.
- Basavarajaiah S, Boraita A, Whyte G, Wilson M, Carby L, Shah A et al. Ethnic differences in left ventricular remodeling in highly-trained athletes relevance to differentiating physiologic left ventricular hypertrophy from hypertrophic cardiomyopathy. J Am Coll Cardiol. 2008 Jun 10; 51(23): 2256-62