This blog is part of a series on work by OPTIKNEE Consensus. This is an international consensus group focused on improving knee health and preventing osteoarthritis after a traumatic knee injury.
Keywords: Rehabilitation, Anterior cruciate ligament, OPTIKNEE
Anterior cruciate ligament (ACL) tears are one of the most talked about injuries in sports medicine. Most people who tear their ACL will embark on a rehabilitation program (with or without ACL surgical reconstruction). The international OPTIKNEE consensus project aims to optimize knee health and prevent post-traumatic osteoarthritis (OA) following knee injuries like ACL tears. As part of this consensus, we recently published a systematic review of systematic reviews in BJSM (OPEN ACCESS) examining the effectiveness of different rehabilitation interventions to improve symptomatic, functional, clinical, psychosocial and quality of life outcomes, and prevent re-injury after ACL (and/or meniscal) injury (1). The summary of this study is outlined in this blog.
Why is this study important?
ACL and meniscal injuries can be devastating (2, 3). Although many people successfully regain pre-injury function and return to sport after extensive rehabilitation and surgery, pain, psychological distress and reduced function are equally as common. They cannot return to pre-injury sport – an activity that brings them enjoyment with all the long-term health and wellbeing participation benefits (4). There is little consensus about the optimal components of an ACL tear rehabilitation program to achieve pre-injury function, activity and quality of life, leading to significant variations in approaches. Systematic reviews of systematic reviews pull together the highest level of evidence as a one-stop shop to inform clinical practice.
How did the study go about this?
This study reviewed systematic reviews of randomised clinical trials that evaluated the effectiveness of any rehabilitation intervention following traumatic ACL and/or meniscal injury (a common secondary injury) to improve symptomatic and/or functional outcomes. We assessed outcomes relating to pain, symptoms, function, re-injury, psychosocial factors, quality of life and adverse events.
What did the study find?
We found 22 systematic reviews, including 142 randomised controlled trials of mostly men (56% – 95%), and almost all after ACL reconstruction (none following isolated meniscal injury). In general, there was a disappointingly low level of evidence for the effectiveness of rehabilitation interventions to improve symptomatic and functional outcomes after ACL injury.
The strongest level of evidence (moderate certainty) was found for:
- Neuromuscular electrical stimulation to improve quadriceps strength.
- Open versus closed kinetic chain exercises to be similarly effective for quadriceps strength, self-reported function, and knee laxity.
- Structured home-based rehabilitation to be similarly effective to structured in-person rehabilitation for quadriceps and hamstring strength, self-reported function, and knee laxity.
- Postoperative knee bracing to provide no benefit to physical function and knee laxity.
Low certainty evidence was found for:
-
- Pre-operative rehabilitation consisting of 3–6 weeks of muscle strengthening and neuromuscular (i.e., function and stability) control exercises to improve self-reported and physical function (e.g., hop performance) 3 months post-ACLR.
- Cryotherapy during the first 1-2 days post-ACLR reduces postoperative pain and analgesic use up to approximately 1-week post-surgery compared with no cryotherapy.
- Psychological interventions including guided imagery, relaxation, coping modelling and visual imagery 6-12 weeks after ACLR to improve psychological and knee laxity outcomes.
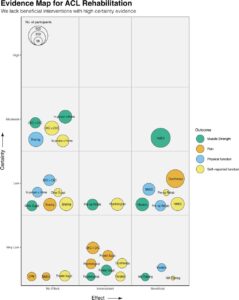
Figure 1: Evidence map for ACL rehabilitation interventions. Only the four most consistent outcomes reported across systematic reviews presented for clarity. CKC, closed kinetic chain; CPM, continuous passive motion; NM, neuromuscular; NMES, neuromuscular electrical stimulation; OKC, open kinetic chain.
Click here for an interactive version of the above figure!
See this infographic for the take-home messages from this study:

References
- Culvenor AG, Girdwood MA, Juhl CB, et al. Rehabilitation after anterior cruciate ligament and meniscal injuries: a best-evidence synthesis of systematic reviews for the OPTIKNEE consensus. British Journal of Sports Medicine. 2022:bjsports-2022-105495. http://dx.doi.org/10.1136/bjsports-2022-105495
- Bruder AM, Crossley KM, Mosler AB, Patterson B, Haberfield M, A. D. Co-creation of a sport-specific anterior cruciate ligament injury risk reduction program for women: A concept mapping approach. Journal of Science and Medicine in Sport. 2020;23(4):353-360. https://doi.org/10.1016/j.jsams.2019.10.019
- Bruder AM, Patterson BE, Donaldson A, et al. Creating Prep to Play PRO for women playing elite Australian football: A how-to guide for developing injury prevention programs. Journal of Sport and Health Science. 2021;doi:https://doi.org/10.1016/j.jshs.2021.09.003
- Bruder AM, Crossley KM, Donaldson A, AB. M. Through the athlete lens: A novel study exploring the perspectives and experiences of injury prevention practices in women playing elite Australian football. Brazilian Journal of Physical Therapy. 2021;doi:https://doi.org/10.1016/j.bjpt.2021.05.003
Author and Affiliations:
Andrea Bruder, Brooke Patterson, Adam Culvenor
Dr Andrea Bruder, La Trobe Sport and Exercise Medicine Research Centre, La Trobe University, Melbourne, Australia
OPTIKNEE Steering Committee Lead Associate Professor Jackie Whittaker