
 By traditional measures, the recent World Health Assembly (WHA) was a success. The assembly, which governs the World Health Organization (WHO), passed resolutions on important topics such as reducing traffic accidents; improving nutrition; and promoting integrated, patient centered care. All good things. But the west African Ebola outbreak and WHO’s failure to respond effectively cast a long shadow.
By traditional measures, the recent World Health Assembly (WHA) was a success. The assembly, which governs the World Health Organization (WHO), passed resolutions on important topics such as reducing traffic accidents; improving nutrition; and promoting integrated, patient centered care. All good things. But the west African Ebola outbreak and WHO’s failure to respond effectively cast a long shadow.
Margaret Chan, the director general of the WHO, started the assembly with a warning on infectious disease readiness: “The world is not prepared to cope.” By the end of the assembly, there had been progress: agreement on a new program for health emergencies with operational capabilities to respond to disease outbreaks, an agreement that we needed to “strengthen” the implementation of International Health Regulations (IHR), and consensus that we need better funding for research and development. But there were lingering doubts about whether any of this will make the world safer next time around.
Resolutions to do a better job are an important first step, but they only go so far. For WHO to be able to execute the goals set at the WHA—from having an effective operational response center to strengthening nations’ abilities to meet IHR requirements—it will require resources. Herein lies the rub: each of these initiatives is woefully underfunded. Laurie Garrett expertly delineates the issue: there is a yawning gap between what the world claims it wants from WHO and what the world will pay for.
This is not a new problem—just look at WHO’s funding over the past couple of decades. In 1998-99, about half of WHO’s funding came from assessed contributions and the other half was voluntary. As we see in the figure below, assessed contributions have been more or less frozen (and declining in inflation adjusted dollars), as WHO’s overall funding increased over the past 15 years. Voluntary (usually earmarked) contributions now make up over 75% of the budget.
Figure 1: Trends in assessed and voluntary contributions, 1998–2013 (US$ millions)*
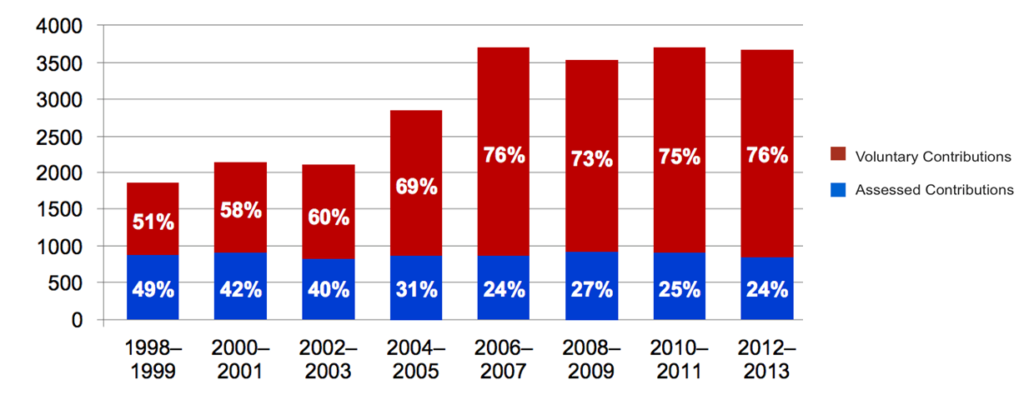
*Data exclude in-kind contributions. For 2010–11 and 2012–13, assessed contributions and voluntary contributions were projected.
Source: World Health Organization, Executive Board Special Session on WHO Reform. Provisional Agenda Item 3 (EBSS/2/INF.DOC./2)
When such a large proportion of funding comes with strings attached, it’s clear that WHO has lost control of its own agenda. It serves as a contracting agency, doing the work of funders. In this light, when WHO set the goal to become more effective in pandemic response, it shouldn’t be a surprise that funders do not line up to support the agency.
While side discussions at the WHA did focus on the lack of funding for proposed initiatives, there was little discussion about why this is the case. Why is it that assessed contributions are flat? Why is it that while there is broad agreement that WHO needs resources for more effective emergency response, donors don’t step up? The answer is simple: it’s an issue of trust. Donors do not trust WHO to spend their money wisely.
There is serious doubt about the ability of WHO to prevent or to manage the next pandemic. And thus, we find ourselves in a classic vicious cycle: because donors don’t trust WHO to be effective, they choose not to fund it adequately, further weakening WHO’s effectiveness. It is time to break this cycle and restore faith in the agency.
Restoring trust has to begin with WHO reform. WHO is seen as secretive and closed, with poor human resources management and accountability. In a report on improving the global response to Ebola we laid out a series of reforms that WHO can undertake to restore trust. Some recommendations require little to no additional resources. This includes “good governance” practices for WHO. It’s pretty simple: Establish a freedom of information policy to create greater transparency and an inspector general’s office to ensure the organization is accountable. Reform human resource management to attract top talent and let go of chronic underperformers.
These reforms require little resources and can be instituted quickly. They just need political leadership and will. If WHO begins with a few key reforms that succeed in improving openness and transparency it will be more effective even with existing resources. And effectiveness begets effectiveness: as WHO gets more transparent and more effective, it will attract top talent and new resources.
The 69th World Health Assembly focused on key issues plaguing the world’s populations. However, lingering doubts from Ebola, made only stronger by the Zika outbreak, reminded participants of one simple fact that Dr Chan iterated: the world is not able to cope with pandemic diseases. If WHO is not up to the task, and in turn unable to convince the world of its competence, the 70th World Health Assembly will be faced with far more fundamental issues than which resolutions to pass.
Ashish K Jha is the director of the Harvard Global Health Institute, the K. T. Li. professor at the Harvard T.H. Chan School of Public Health, and a practicing internal medicine physician at the VA Boston Healthcare System.
Competing interests: None declared.
Liana Woskie is the assistant director of the Harvard Global Health Institute’s Initiative on Global Health Quality and manages the institute’s pandemic response work.
Competing interests: None declared.
