The incidence of having a baby in the bottom-down (“breech”) position at the end of pregnancy is about 1 in 25. The “Term Breech Trial” (TBT) is a landmark randomised controlled trial that changed the management of breech birth since its publication in 2000. It concluded that a planned Caesarean birth is safer for the baby, with no increase in morbidity for the mother, compared to a planned vaginal breech birth. Despite the follow-up study not showing any difference in longer-term (two year) outcomes, we have observed a steady decline in vaginal breech birth in high-income countries, and subsequent loss of obstetric skill. In the UK, about 96% of breech presenting babies are born by Caesarean. Vaginal breech birth has become increasingly stigmatised as “out of date” and “dangerous” for babies and mothers.
I became involved in the Optibreech Collaborative after working in Yemen as an obstetrician in a humanitarian response in 2021. In Yemen and many other low-income countries, the risk of Caesarean birth for the mother is too high to justify the small potential benefit to the baby. In contexts where women have a high fertility rate, and where oxytocin boluses are sometimes used in the village setting when labour is slow (or even obstructed), uterine rupture is much more common and is a major cause of maternal death. Other complications from Caesarean birth in a subsequent pregnancy include scar ectopic pregnancy, abnormal placentation and surgical risks of multiple Caesareans – all life threatening complications when high quality obstetric care is limited.
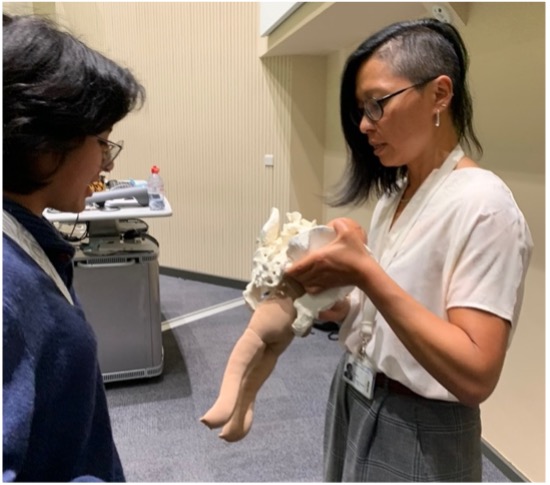
Optibreech Care is an innovation care package based on research:
- Women are encouraged to adopt an upright “all-fours” position as opposed to traditional lithotomy (the evidence shows that upright positions are associated with shorter labours and fewer interventions);
- Birth attendants receive enhanced training in physiological breech birth;
- Manual manoeuvres and time-based indications for interventions are used.
This is a significant departure from traditional obstetric teaching on breech births. Doctors are rarely taught how to assist a birth (breech or otherwise) with women in any other position apart from supine or lithotomy. Whilst midwives and traditional birth attendants may be more skilled in upright birth techniques, their status is lower in the hierarchy of medical practice. The World Health Organisation’s Guideline lists lack of a skilled birth attendant, previous Caesarean, and “clinically inadequate pelvis” as indications for a Caesarean birth in the context of breech presentation, which reflects a lack of skill and confidence in vaginal breech birth even in low-income settings.
It should also be noted that antenatal screening and ultrasound scanning is not universally available. A larger proportion of breech babies in low-income settings will have an underlying fetal anomaly. I performed a Caesarean section for a woman with a breech baby in South Africa and the baby actually had a lethal skeletal dysplasia, dying within a few hours of birth. Caesareans of this nature violate the “first do no harm” principle of non-maleficence as they have no benefit to the baby and only increase the risk of future pregnancy for the mother (in addition to any potential surgical complications in the index pregnancy).
Undoubtedly, a large motivator for the Optibreech Care Trial is its mission to provide choice to women with breech presentation at term. In ethnic-diverse London, I have treated women from Somali, Ethiopian, Pakistan, and other cultural origins where it is considered “better” to have a vaginal birth. “I just think my body can do it”, one Somali woman with breech-breech twins told me. She already had two babies vaginally and was concerned with the recovery from a Caesarean, potential complications, and managing with 4 children under 5. She beamed with joy after the spontaneous, uncomplicated birth of both babies and told me, “You were the only doctor who believed in me.”
The Optibreech algorithm and enhanced training has given my unit in London the confidence to offer safe vaginal breech birth. More women having vaginal breech births in turn challenges myths and resurrects this lost obstetric skill, which has the potential to save mothers’ and babies’ lives globally. Introducing upright vaginal breech methods will take an enormous cultural shift in how we think about maternity care in low-income and humanitarian settings:
- We need investment in training birth attendants in complex vaginal birth (for breech presentation, multiple pregnancy, fetal malposition) in addition to provision of safe Caesarean birth
- Supine-lithotomy position should not be the birth position of choice (cephalic or breech) – it is no wonder many women prefer to birth at home with a traditional birth attendant when faced with this alternative in maternity clinics and hospitals;
- Research findings in high-income settings cannot be universally applied to low-income settings as the risk-benefit ratio for maternal and neonatal health is dependent on cultural and societal contexts.
About the author: Dr Sabrina Das is a Consultant Obstetrician & Gynaecologist in Imperial College Healthcare NHS Trust, with a special interest in high risk pregnancy, global health and quality improvement. She has previously worked in Guatemala, South Africa and Yemen. Views are personal and not reflective of her employer. She tweets at @drsabrinadas.
Competing interest: Dr Sabrina Das is a Principal Investigator for the Optibreech Care Trial.
Handling Editor: Neha Faruqui