India has been transitioning from rural to quasi-urban due to rapid urbanization over the last two decades and is expected to continue in the coming years. It is estimated that 43.2% of India’s population, i.e., 675 million people, will reside in Urban conglomerates by 2035 (UN-Habitat 2022). While urbanization has provided economic growth and socio-economic development opportunities, it has also brought adverse health issues, such as the rising burden of non-communicable diseases, road traffic injuries, emerging and re-emerging infectious diseases, antimicrobial resistance, and substance abuse. These urban health problems are influenced by non-medical factors like socio-cultural, economic, and demographic characteristics (gender, race, ethnicity, caste, religion, education, wealth, behavior, lifestyle), living environment (out-door safety, air, climate), access to safe basic amenities (food, water, shelter), public goods & services (healthcare, sanitation, wage, employment, law & order, electricity, mobility, social-security nets, information) viz., collectively termed as social determinants of health. Against this background, in September 2021, the National Institution for Transforming India technical committee on “Reforms in Urban Planning Capacity” recommended that the Government of India transform 500 cities into “Healthy Cities for All” through 2030 a city-specific master plan supported by concerted multisectoral actions at intersections of spatial planning, public health, and socio-economic development.
Healthy Cities Approach in India
Healthy Cities’ notion is deeply rooted in the principles of promotion of environmental hygiene, public health, healthy lifestyle choices, the role of local bodies, efforts, and their policies in creating the physical and social environment for citizens to mutually support each other in carrying out all life functions and achieving their full potential. Applying the Healthy City approach to a city takes the form of action-oriented projects aiming to reform the deteriorating environmental and public health conditions locally. In the late 1980s, World Health Organization promoted the concept worldwide. The developed healthy city frameworks resulted in context-specific approaches, processes, and innovative solutions generated from health and non-health actors through intersectoral action planning, resource pooling, public-private partnerships, and community participation in integrating health protection and health promotion activities and transforming health determinants for betterment in many European, Latin-American, and South-East Asian countries.
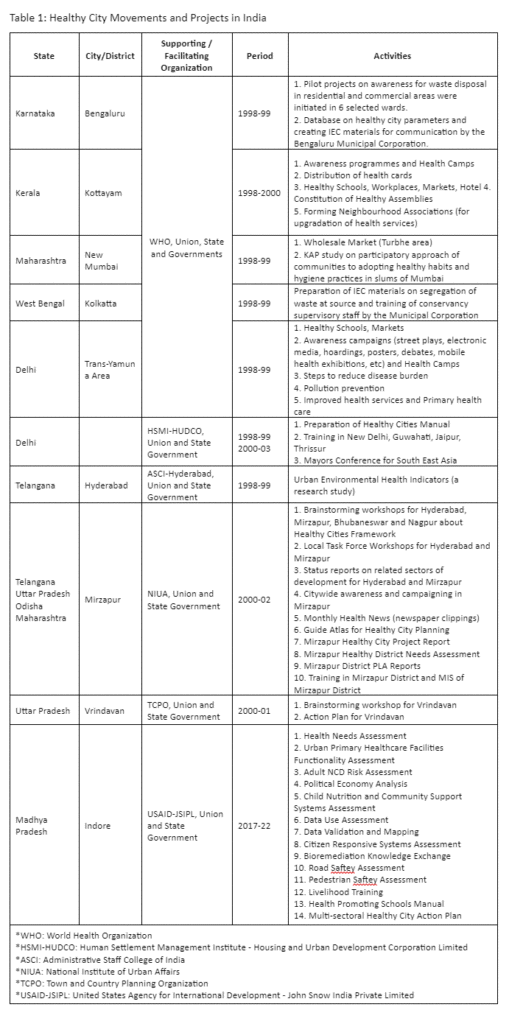
In India, the Healthy Cities Projects were started in the late 1990s initially promoted in the metropolitan cities of Kolkatta, Mumbai, Delhi, and Bangalore. Soon, it was scaled up in tier-II and III towns (Table 1). Unlike high-income countries, in India, the Healthy City Approach was not fully evolved and well received by the governments due to multiple factors and was implemented as short-term demonstration projects with little political attention and sustainability. On review of documents and reports on Healthy Cities, none of the Indian context-specific approaches were quoted nor shared as lessons in the WHO Healthy Cities networks platform for cross-learnings from each other. Recently, a USAID-funded Building Health Cities Project (2017-22) was implemented in Indore, India. It demonstrated that multisectoral systems approach, data-driven decision-making, and active community participation could lead to citizen-centric sustainable urban development with particular emphasis on citizens’ health by addressing their social determinants of health. This, coupled with strengthening urban healthcare systems, can address issues relating to rapid urbanization.
Lessons learned and Way forward
In India, the benefits of the Healthy Cities Movements (HCM) were not fully realized due to the prevailing policies, governance and administrative bodies, processes, inadequate devolution of powers and functions between the Union-State-Local, management strategies, and fiscal capabilities (generation and utilization), along with the political will and culture of the country. The projects require a minimum five-year gestation period for impact. The projects should be planned with an adequate timeframe and sustainable resources, be specific to contextual problems and priorities and adaptable to field realities, and involve sectoral departments, elected representatives, and communities in the planning process for successful completion. There is a need to reduce the rigorous administrative path for project approvals and create enabling environment to ease implementation. The exploratory and dynamic nature of healthy city projects demands timely communications and decision-making; hence institutional processes should be established hassle-free to facilitate these fast-paced environments. The local context-specific demonstrative solutions encourage community participation and behavioral adaptations than the regular planning exercises. The convergence of multisectoral developmental activities and coordination yield better results; Hence, healthy city projects should be nested within the ongoing development programs so that the utility of infrastructures and services complement the government and citizens’ efforts to attain better health outcomes. The elected representatives must foster the publicity of healthy city projects, and the government will have to internalize the healthy city concept in all sectoral departments through development projects.
The COVID-19 crisis has highlighted the shortcomings in India’s healthcare system more prominently in the urban areas, such as poorly equipped urban primary healthcare systems and the role of urban local bodies in public health, including air and water pollution, road traffic injuries, and pandemic-related vulnerabilities. The experiences and learnings from the past healthy cities project, WHO tools, resources, and the “SMART” city mission will guide the institutions and governments to implement future healthy city projects. Healthy city planning is gradually emerging in India, though in its nascent stage; if pursued would evolve into an effective urban planning and policymaking process. In time to come, this phenomenon will develop into a system and practice worth following for building sustainable urban health management strategies to reduce urban health inequities and other challenges and improve the quality of life for urban citizens.
About the author: Kumaravel Ilangovan is a Public Health Professional currently working as a Specialist who leads Urban Health and Primary Health Care portfolio in Health Systems Transformation Platform, New Delhi, India. He can be reached at k.ilangovan@hstp.org.in Twitter ID: @drKumaravel OrcID: 0000-0003-0111-511X
Competing interest: None
Handling Editor: Neha Faruqui