COVID-19 is spreading rapidly across Europe. Many people are currently suffering from it and thousands in Europe are dying. We know that these numbers will inevitably rise much further. The European Council recently stressed the importance of European solidarity and cooperation in response to the COVID-19 outbreak.
Most European countries have ensured that there are no major financial barriers in access to health care, to tests, and to (eventual) subsequent treatment. Ensuring adequate capacity in a crisis such as this, especially for ventilators and intensive care for the most severe cases, is more difficult to solve at short notice and, in some places facing the most severe pressures, there are reports of rationing care. In a situation such as this, international cooperation to enable access to acute-bed capacity is one way to reduce this pressure.
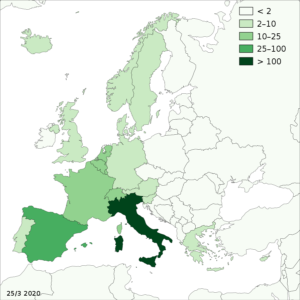
The increased need for intensive care capacity is not affecting all countries with equal intensity. In some countries, hospitals are overcrowded already, while in other countries there are, for the moment, empty beds waiting for patients. Some examples of European cooperation are now emerging (with German hospitals taking patients with COVID-19 from eastern France and northern Italy). Public and private clinical laboratories are also coordinating efforts in several European countries to increase the testing and screening capacities for COVID-19. Such measures can be extended within the legislative framework provided by the Directive on cross-border care, which creates mechanisms for issues such as payment for care received in another member state.
Re-distributing the impact of peak pressure of the epidemic in one geographical area (region or country) by use of existing capacity in other area will reduce congestion and stress in health systems.
International sharing of intensive care beds is only one of the existing opportunities for a truly European effort addressing the COVID-19 challenges, building on the mechanisms established for public health threats that cross borders, laid out in Decision No. 1082/2013/EU.
The COVID-19 pandemic has demonstrated the importance of cooperation in health care between Members States, such as the Joint Procurement Initiative for medical countermeasures and the Innovative Medicines Initiative 2, but there is a need to go further, both now, using mechanisms such as those in Article 196 of the Treaty of Lisbon, on co-operation in the event of natural or manmade disasters, and in the future, through enhanced co-operation mechanisms, building on those established within the European Semester.
This pandemic also shows the urgent need for innovations in prevention and care, exploiting the opportunities offered by digitalization, such as tele-medical services in situations where face-to-face provision needs to be minimized. Cooperation and innovation is necessary if we are to increase the resilience of our health systems through strong person- and people-centred care that will benefit all European citizens.
The economic disruption associated with COVID-19, with containment measures forcing a large number of people to stay home will exceed what happened at the peak of the last international financial crisis. Moreover, it hits all countries within a short time period.
Family and social networks are threatened by this crisis. The psychosocial impact of isolation and social distancing to contain the virus generates additional population needs, which can only be addressed through investment in comprehensive primary care and strengthened social cohesion in affected countries. What this crisis makes clear is the need for more integration of primary care and public health services, further establishing their role in both disease prevention and health promotion.
In future, Member States must commit to ensuring the collection, retention and, with appropriate safeguards, sharing of meaningful data that can inform identification of proven and efficient practices . These will be essential in preventing and responding to new crises.
These are truly exceptional times. A united response underpinned by the solidarity and human values that are at the heart of the European project will build a stronger European identity, one that could inspire and help other regions across the world. Local initiatives by citizens, the heroic efforts of health care staff, and the commitment of volunteers illustrate the centrality of solidarity in the European project.
By demonstrating solidarity in the ways that Member States cope with infectious disease outbreaks, Europe will provide an enduring example and a precedent for addressing future pandemics. However, solidarity must extend to vulnerable regions outside the European Union – particularly, but not necessarily limited to, low and middle income countries, and especially the most vulnerable within them.
Pathogens do not respect national borders. COVID-19 will not be the last pandemic. The Member States of the European Union (EU) must act to protect populations and to save the democratic and humanitarian values the Union stands for.
The authors are all experts in health care, health systems, health policy, and health economics at European level. They are or have been Members of the Expert Panel on Effective Ways of Investing in Health . They are writing this letter in a personal capacity.
- Jan De Maeseneer, Department of Public Health and Primary Care, Ghent University, Belgium
- Pedro Barros, Nova School of Business and Economics, Universidade Nova de Lisboa, Portugal.
- Martin McKee, London School of Hygiene and Tropical Medicine, United Kingdom
- Christian Anastasy, consultant, France
- Natasha Azzopardi-Muscat, Department of Health Services, University of Malta, Malta
- Margaret Barry, World Health Organisation Collaborating Centre for Health Promotion Research, National University of Ireland Galway, Ireland
- Aleš Bourek, Center for Healthcare Quality, Masaryk University, Czech Republic
- Werner Brouwer, Erasmus School of Health Policy & Management, Erasmus University Rotterdam, The Netherlands
- Anna García-Altés, Catalan Health System Observatory, Agency for Health Quality and Assessment of Catalonia, Spain
- Damien Gruson, Department of Clinical Biochemistry, Cliniques Universitaires St-Luc and Université Catholique de Louvain, Brussels, Belgium.
- Dionne Sofia Kringos, Amsterdam UMC, University of Amsterdam, Department of Public Health, Amsterdam Public Health research institute, The Netherlands
- Fernando Lamata, Advisory Council of the Ministry of Health, Spain
- Lasse Lehtonen, Helsinki University Hospital, Helsinki, Finland
- Christos Lionis, Clinic of Social and Family Medicine, School of Medicine, University of Crete, GreeceLiubove Murauskiene, Department of Public Health, Institute of Health Sciences, Faculty of Medicine, Vilnius University, Lithuania
- Sabina Nuti, Department of Health Management, Sant’Anna School of Advanced Studies, Pisa, Italy
- Walter Ricciardi, Department of Public Health, Università Cattolica di Roma, Italy
- Heather L. Rogers, Biocruces Bizkaia Health Research Institute and Ikerbasque Basque Foundation for Science, Spain
- Luigi Siciliani, Department of Economics and Related Studies, University of York, United Kingdom
- Dorothea Stahl, Klinikum Bremen-Mitte, Gesundheit Nord gGmbH – Klinikverbund Bremen, Bremen, Germany
- Sarah Thomson, WHO Barcelona Office for Health Systems Strengthening, Spain
- Katarzyna Wieczorowska-Tobis, Department of Palliative Medicine, Karol Marcinkowski University of Medical Sciences, Poland
- Claudia Wild, Austrian Institute for Health Technology Assessment (AIHTA), Austria
- Jelka Zaletel, National Institute of Public Health, Slovenia
European Union, 25 March 2020