 • The WHO and World Bank have released a report showing as many as 400 million people around the world do not have access to essential health services. The report, published in the year of expiry of the United Nations’ deadline on its millennium development goals, found that while good progress had been made in some areas, such as childhood vaccinations, there had been less success in other areas. For example in 2013, just 37% of people infected with HIV received antiretrovirals. The report looked both at health service coverage as well as financial protection and found that in 37 countries, 6% of the population was in danger of falling into extreme poverty (living on $1.25 (£0.81; €1.11) or less a day) because these people had to pay for health services out of their own pockets.
• The WHO and World Bank have released a report showing as many as 400 million people around the world do not have access to essential health services. The report, published in the year of expiry of the United Nations’ deadline on its millennium development goals, found that while good progress had been made in some areas, such as childhood vaccinations, there had been less success in other areas. For example in 2013, just 37% of people infected with HIV received antiretrovirals. The report looked both at health service coverage as well as financial protection and found that in 37 countries, 6% of the population was in danger of falling into extreme poverty (living on $1.25 (£0.81; €1.11) or less a day) because these people had to pay for health services out of their own pockets.
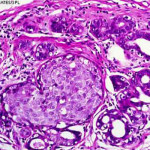 • Research published in JAMA Oncology showing follow-up data from the Women’s Health Initiative trials shows postmenopausal women who are overweight or obese have a raised risk of invasive breast cancer. Women with a BMI greater than 35 had a 58% higher risk of invasive breast cancer than women with a BMI lower than 25.
• Research published in JAMA Oncology showing follow-up data from the Women’s Health Initiative trials shows postmenopausal women who are overweight or obese have a raised risk of invasive breast cancer. Women with a BMI greater than 35 had a 58% higher risk of invasive breast cancer than women with a BMI lower than 25.
• You can read the GMC’s chief executive and registrar, Niall Dickson’s response to Benjamin Dean’s personal view that questioned the role of the GMC in the Shape of Training review.
 • Nearly 14 million units of whole blood or packed red blood cells were transfused in the United States in 2011 and recent research showed that transfusion of four or more units of packed red blood cells was associated with increased odds of perioperative stroke or myocardial infarction. This team from the University of California investigated whether smaller perioperative transfusions, which are more common, also had adverse effects. Their retrospective cohort study of hospital administrative data showed that transfusion of as little as one unit was associated with an odds ratio of 2.33 (95% confidence interval 1.90 to 2.86) for perioperative stroke/myocardial infarction, and the odds of both markedly increased with transfusion of four or more units.
• Nearly 14 million units of whole blood or packed red blood cells were transfused in the United States in 2011 and recent research showed that transfusion of four or more units of packed red blood cells was associated with increased odds of perioperative stroke or myocardial infarction. This team from the University of California investigated whether smaller perioperative transfusions, which are more common, also had adverse effects. Their retrospective cohort study of hospital administrative data showed that transfusion of as little as one unit was associated with an odds ratio of 2.33 (95% confidence interval 1.90 to 2.86) for perioperative stroke/myocardial infarction, and the odds of both markedly increased with transfusion of four or more units.
• In a linked editorial, Stavros Memtsoudis discusses the limitations of using such large national database research to evaluate rare or moderately rare outcomes. He argues for “a third way: specialized data collection constructs such as multi-institutional registries that combine the benefits of large numbers of patients with detailed and relevant clinical information.” However, he concludes that the research to date supports the working hypothesis that a liberal transfusion strategy is associated with worse outcomes than a more restrictive strategy. He advises “prudent clinicians should practice restraint when contemplating blood transfusions and also use strategies to decrease the risk of bleeding and aneamia.”
Kate Adlington is a clinical fellow at The BMJ. Follow Kate on Twitter @kateadlington
