A survey carried out by the Idiopathic Intracranial Hypertension Charity in the UK, which exposed the toll on patients of undergoing repeated lumbar puncture, has spurred a collaborative research project and paved the way for improved clinical management
Idiopathic intracranial hypertension (IIH) is a rare condition that affects as many as one to three in 100 000 people a year. [1,2] It is most common in young women and a rising incidence of the condition is correlated with the increasing incidence of obesity. [3] Most patients with IIH experience chronic disabling headaches, which significantly reduce quality of life. [6] They are also at risk of visual loss varying from mild to total blindness, with up to 25% of patients reported to suffer permanent severe visual loss. [5] The finding of raised intracranial pressure at lumbar puncture is an essential diagnostic criteria. Other diagnostic criteria include the presence of papilledema but no abnormal neurological signs, and a normal brain scan and cerebrospinal fluid content. [7]
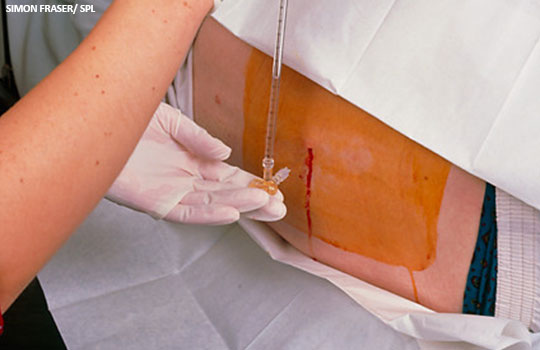 A recent Cochrane review highlighted the limited evidence to guide treatment, and management strategies vary considerably. [9] Patients frequently undergo repeated lumbar punctures (pictured) to evaluate the severity of their disease and in some centres lumbar puncture is carried out as a therapeutic procedure, although there is no good evidence to support this method of management. [2]
A recent Cochrane review highlighted the limited evidence to guide treatment, and management strategies vary considerably. [9] Patients frequently undergo repeated lumbar punctures (pictured) to evaluate the severity of their disease and in some centres lumbar puncture is carried out as a therapeutic procedure, although there is no good evidence to support this method of management. [2]
The patient’s perspective: Sandra Doughty
As a patient with IIH and in my role as the former head of the IIH:UK, a charity set up to support people living with IIH, I know from personal experience and extensive dialogue and feedback from IIH:UK members that undergoing lumbar punctures can be a very distressing experience. Indeed, the experience of undergoing the procedure can be so upsetting for patients that when they later recall it many are brought to tears and express fear about the prospect of undergoing future procedures.
Aware of this distress and the absence of studies assessing the impact on patients of undergoing (what in some cases is repeated) lumbar puncture, IIH:UK undertook a survey of its members. We hoped to illuminate patients’ experiences of lumbar punctures, raise awareness of this among health professionals, and drive developments in clinical practice that would improve patients’ experience of the procedure.
This survey of 358 members of the IIH:UK society reinforced the anecdotal evidence we were aware of in relation to the emotional impact of undergoing lumbar puncture. The IIH:UK trustees realised, however, that a small qualitative survey would be unlikely to sway the views or practice of clinicians so the charity decided to approach the neurology team at the University Hospitals Birmingham (UHB) to suggest a collaborative research project as Alexandra Sinclair is patron of IIH:UK. The neurology team agreed and a joint UHB and IIH:UK team was set up.
Patient led research project
The research collaborative included Alexandra Sinclair, a statistician; Susan Mollan, a clinical neuro-ophthalmologist; William J Scotton, a clinical academic neurology trainee; and Thomas Walters, a medical student. Based on the findings of the initial qualitative survey, we decided to: 1) establish structured questions so that answers to them could be readily analysed, (we had struggled to summarise and analyse the qualitative data from the first survey into a clear message); 2) get help with statistical analysis; 3) involve clinicians. The latter point was a key decision. We are a relatively new charity (established 2011) with little experience in conducting and analysing data. We realised that working with a medical team would add value and that if our research was to sway the mindset of clinicians, the study methodology would need to be robust. Additionally, we hoped that involving an academic university hospital, which already has a dedicated research program for IIH, would not only give credibility to our study but help us disseminate its results widely.
IIH:UK developed the initial questionnaire, which was then shaped by the UHB team to refine questions amenable to objective analysis. This was an iterative process and several rounds of revisions were needed to ensure that the questions remained relevant and understandable to patients. IIH:UK then published the questionnaire on the charity website from 1 April to May 2015. Full responses were received from 502 patients (responses were excluded if they were incomplete, uninterpretable, or from respondents under the age of 16). The number of participants was noteworthy as IIH is a rare disease (Kilgore 2017), and most research studies of IIH have been conducted in smaller cohorts.
The clinician’s perspective
Early on it became evident that the patient perspective of undergoing lumbar punctures bore little relation to the doctor’s perspective and understanding of the procedure. For example, when discussing the number of attempts did this mean a different doctor trying the procedure, or the number of passes through the skin, or the number of passes to re-site the needle within the back?
The patient representatives were keen to establish how many lumbar puncture “attempts” were made. They were aware from patient feedback that this was an important issue for patients since it had a bearing on the overall pain experienced, the duration of the procedure, and their confidence in the doctor conducting the procedure. The clinicians were wary of using the number of attempts at lumbar puncture as a metric due to the variability of interpreting this metric and the possible inaccuracy of the patient’s assessment of this. It is possible, clinicians argued, that given the lumbar puncture site would normally be fully numbed by local anaesthetic, multiple attempts could be performed without the patient’s knowledge.
After due discussion between patients and clinicians, different opinions on this issue were reconciled and it was agreed that pain would be quantified with a verbal rating score (VRS) with 0 for no pain and 10 for maximal pain. A further question was formulated that asked about the patient’s view of the seniority of the doctor who performed the procedure, as this was felt to reflect the patient’s perceptions of the doctor’s skills.
Main findings, their dissemination, and impact
Together, as a group of patients and clinicians, we have reflected on the main findings of the study. Firstly, we found that two thirds of patients felt poorly informed about what a lumbar puncture involves, particularly when this procedure is undertaken as an emergency, and where this was the case it was associated with higher (recalled) pain scores. As a result of this finding, the research collaborative are currently co-producing pre-procedure patient information leaflets on lumbar puncture. We also agreed that patient experience is likely to be improved when analgesia is adequate and that limiting the number of emergency lumbar punctures is desirable. To address these issues, it was agreed that it would be best to undertake the procedure, where possible, in a prearranged dedicated unit such as an ambulatory care environment. The neurology unit has also set up lumbar puncture simulation training for trainees and introduced ultrasound guided lumbar punctures (Soni 2016).
This joint project took more time than we expected as the IIH:UK and UHB teams gleaned and responded to each other’s perspective and priorities. It has taught the clinical team the value of listening to patients’ concerns and co-creating the research agenda with them, and helped the charity to see the value of joint working with health professionals. A more tangible product of the collaborative has been the move by IIH:UK to independently fund and establish a James Lind Priority Setting Partnership to determine the top 10 research priorities in IIH.
Sandra Doughty is the past chair of IIH:UK.
Alexandra Sinclair is an NIHR clinician scientist fellow at the Institute of Metabolism and Systems Research at the University of Birmingham and a consultant neurologist at University Hospitals Birmingham. Her clinical scientist role combines clinical neurology with translational research into idiopathic intracranial hypertension and the neuroendocrine aspects of headache.
Susan Mollan is a consultant neuro-ophthalmologist at University Hospitals Birmingham NHS Foundation Trust.
William J Scotton is currently an academic clinical fellow in neurology and his research interest is the study of CSF flow.
Thomas Walters is a medical student at the University of Birmingham
Shelly Williamson is the current chair of IIH:UK.
Conflicts of interest: The authors report no conflicts of interest.
Funding: AS is funded by an NIHR clinician scientist fellowship (NIHR-CS-011-028) and by the Medical Research Council, UK (MR/K015184/1).
Related content: Listen to a podcast with Katherine Cowan, a senior adviser at the James Lind Alliance, which has pioneered patient involvement with their research priority setting partnerships.
References:
1.Markey KA, Mollan SP, Jensen RH, Sinclair AJ. Understanding idiopathic intracranial hypertension: mechanisms, management, and future directions. The Lancet Neurology. 2016 Jan;15(1):78-91.
2.Mollan SP, Ali F, Hassan-Smith G, Botfield H, Friedman DI, Sinclair AJ. Evolving evidence in adult idiopathic intracranial hypertension: pathophysiology and management. J Neurol Neurosurg Psychiatry. 2016 Sep;87(9):982-92.
3.Kilgore KP, Lee MS, Leavitt JA, Mokri B, Hodge DO, Frank RD, Chen JJ. Re-evaluating the Incidence of Idiopathic Intracranial Hypertension in an Era of Increasing Obesity. Ophthalmology. 2017;124(5):697-700.
4.Andrews L, Liu GT, Ko M Idiopathic Intracranial Hypertension and Obesity. Horm Res Paediatr. 2014;81:217-225
5.Corbett, J. J., P. J. Savino, H. S. Thompson, T. Kansu, N. J. Schatz, L. S. Orr and D. Hopson (1982). “Visual loss in pseudotumor cerebri. Follow-up of 57 patients from five to 41 years and a profile of 14 patients with permanent severe visual loss.” Arch Neurol. 39(8): 461-474.
6.Mulla Y, Markey KA, Woolley RL, Patel S, Mollan SP, Sinclair AJ. Headache determines quality of life in idiopathic intracranial hypertension. The Journal of Headache and Pain. 2015;16:45. doi:10.1186/s10194-015-0521-9.
7.Friedman DI, Liu GT, Digre KB. Revised diagnostic criteria for the pseudotumor cerebri syndrome in adults and children. Neurology. 2013 Sep 24;81(13):1159-65
8.Batra R, Sinclair A, Mollan S. United Kingdom CSF Disorders Day, 14th October 2016, University Hospitals Birmingham. Neuroophthalmology. 2017 Mar 1;41(3):161-163
9.Piper, R. J., A. V. Kalyvas, A. M. Young, M. A. Hughes, A. A. Jamjoom and I. P. Fouyas (2015). “Interventions for idiopathic intracranial hypertension.” Cochrane Database Syst Rev 8: CD003434.
10.Soni NJ, Franco-Sadud R, Schnobrich D, Dancel R, Tierney DM, Salame G, Restrepo MI, McHArdy P, Ultrasound guidance for lumbar puncture. Neurol Clin Pract. 2016;6 (4):358-368
