 My wife and I arrived in Zambia in August 2012 for a six month placement as surgical registrars in a busy rural hospital in the Eastern Province. This was my first experience of hospital care in the developing world and I was soon working all hours of the day and night, operating on everything from minor wounds, to major trauma, and abdominal catastrophes.
My wife and I arrived in Zambia in August 2012 for a six month placement as surgical registrars in a busy rural hospital in the Eastern Province. This was my first experience of hospital care in the developing world and I was soon working all hours of the day and night, operating on everything from minor wounds, to major trauma, and abdominal catastrophes.
St Francis’ Hospital is unique in the local area because it provides an entirely free service and always has at least one experienced consultant surgeon from Europe. Patients travel for hundreds of kilometres to the hospital expecting, and receiving, a high quality of care.
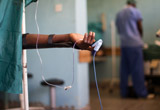
Packed in our hand luggage on the flight were three Lifebox pulse oximeters. They have proved to be incredibly popular with the theatre staff and anaesthetists. Prior to our arrival, the old theatre monitors had burnt out and not been replaced, so anaesthetic monitoring was by manual pulse check and auscultation. This was clearly dangerous, given the high throughput of patients (often more than ten patients per theatre every day) and the complexity of some of the operations, and it had led to some near misses.
To illustrate the benefit of continuous monitoring, I need only describe one case. While amputating a gangrenous hand, the patient suffered a cardiac arrest. We were able to recognise his loss of cardiac output immediately, start CPR, and successfully resuscitate him. He survived and was discharged a couple of weeks later. Without the oximeter we wouldn’t have noticed so quickly, and it is unlikely that he would have recovered.
Perhaps the most motivated people have been the theatre nurses—they will often find the oximeter and make sure it is connected before the anaesthetist asks, or take one to the recovery area following a major case. In fact the hospital is now planning on investing in several more Lifebox oximeters for the recovery area with the aim that all patients are fully monitored from induction of anaesthesia until their return to the ward.
When I first arrived, operating without the reassuring “beep” of a monitor was a novel experience. Now on the other side of the drape, I am operating with the confidence that the patient is stable.
The Lifebox oximeters are proving ideal for this front line environment. They are robust, the charge lasts for hours (we have frequent power cuts), but above all they are easy to use. Indeed, in the minor ops theatre, where we operate under Ketamine sedation, it is sometimes the porter who first notices the dropping saturations and supports the airway.
Every case is now monitored with a Lifebox oximeter. The anaesthetists have a lot more ownership and control over their anaesthetics and we have noticed a big change in how they work.
Geoffrey Roberts is a UK surgeon in training. He and his wife Charlotte are currently spending six months volunteering at St Francis’ Hospital, Katete, a rural mission hospital in Zambia.
