Blog by Swati Satish Joshi
The understanding of the suffering of patients infected with corona virus, especially during the second wave in India, transformed from being subjective to objective, personal to data-centric, and general to individual. While media was engrossed in covering stories of blame (critiquing liberties sanctioned by government, for instance, gatherings of thousands at the cricket stadium, Kumbh Mela, etc.) the health care infrastructure continued to cave in. The exponential rise in the number of corona cases and the dearth of ambulances, hospital beds, oxygen cylinders, remdesivir tablets and injections, meant that patients continued to die in the ambulances, at home, in the parking area of the hospitals etc. The doctors, nurses, and paramedical staff were rendered helpless as they were compelled to witness the dance of death.
In the meantime, the doctors advised the patients diagnosed with COVID-19 to monitor SpO2 using pulse oximeters. A pattern of mortality in the second wave of COVID-19 in India emerged, wherein the patients died owing to the sudden drop in the oxygen level in the bloodstream. Tribune News Service approached Prof. Puri, Head, Department of Anaesthesia and Intensive Care, Post Graduate Institute of Medical Education & Research, who explained the relation between blood oxygen level and Covid-19: if the saturation of oxygen dropped below 94 per cent in the patients infected with COVID-19, it would show a sudden acute drop causing fatalities. My mother’s case was no exception apropos of this pattern of mortality.
My parents tested positive on 16th April, and on April 18th, my mother’s oxygen saturation dropped from 91 to 72 in 75 minutes. We booked the ambulance, but due to the shortage of ambulances, we had to wait for twelve hours to get one. In the meantime, her oxygen level further dropped to 62. A good Samaritan, who himself had recently recovered from COVID-19, donated us his spare oxygen cylinder. That’s how my mother could get supplementary oxygen support until the ambulance arrived. Even after getting the ambulance, the struggle continued. There was only one hospital that had high-tech medical equipment, and even there we had to wait for almost three hours to get her admitted. There were approximately two hundred ambulances waiting outside the hospital to admit the patients. The ground reality at the hospital reflected philosopher Norman Daniels’s reflection on distributive justice. In his article, Daniels discusses the role of health-services that are meant to ameliorate, “quality of life, not to extend or save it. Some of these services restore or compensate for diminished capacities and functions; others improve life quality in other ways” (Daniels, 146). And this holds true with respect to the contemporary convoluted mechanism of availing ambulance services and hospitals with well-equipped Intensive Care Units in Ahmedabad, Gujarat. The guidelines for hiring ambulance services in Ahmedabad would change unexpectedly and the family members of the COVID-19 patients were left to their own devices to arrange for the hospital and ambulance.
I have experienced these hurdles to admit my parents to their respective hospitals. When I had to move my father from one hospital to another, I was informed by the ambulance services that they were instructed by the policy makers to take only those patients to the hospital who were confined at home; inter-hospital transfer of patients by ambulance came to a halt.
In the wake of rising number of patients suffering from COVID-19, first it was difficult to get access to health care facilities. Second, receiving the access was not enough. Some patients are perceived as medical mystery by the doctors because they did not find them suffering from corporeal pain. The traditional understanding of physical pain synonymous with suffering, which is explained by Cassell (32), is one of the major reasons for the delay in medical intervention. Patients who do not experience discomfort such as shortness of breath, despite low oxygen levels, are viewed as special medical cases since their suffering is not corporeal. The tendency to equate suffering with physical pain prolongs the medical intervention for some patients.
My mother was not suffering from shortness of breath, while her oxygen level dropped to 62. And since this was not interpreted as suffering by a certain doctor, he blamed the faulty oximeter, instead of initiating the medical treatment.
The second wave of COVID-19 in India has exposed harsh realities: loopholes in the public health infrastructure, as well as the extreme stress experienced by doctors and nurses owing to the paucity of medical amenities in the face of constant rise in the admission of critically ill patients in the hospital. Moreover, depersonalized understanding of the suffering of the COVID-19 patients has paralyzed the public health infrastructure. The accessibility of the medical intervention is dependent not only on the adequacy of the medical amenities but also on how medical practitioners perceive and classify the patient’s suffering.
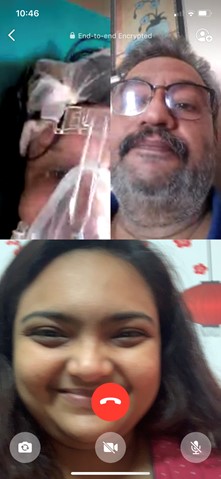
The above photograph is the last and the most precious one I have of my parents. I dedicate this piece to my mother and father, who suffered enormous physical, emotional, and psychological pain in the process of hospitalization. The private hospital where my father was admitted asked us to arrange four remdesivir doses by ourselves, because the government was not able to furnish the hospital with the adequate amount of remdesivir injections . Also, mine is not the only family that had to go through these horrendous struggles. It is very unfortunate that in spite of paying hefty amounts of fees, there are many hospitals that cannot provide beds, medicines, and oxygen cylinders to their patients.
The reception office of the hospital where my mother was admitted wouldn’t update us regularly about her condition. I would text my mother and keep asking her about her SpO2 level. She would keep me posted about the medicines and tests prescribed to her.
Most importantly, the journey of suffering doesn’t end with the patient’s death. We had to wait for almost two hours outside the crematorium to perform the last rites for my mother. I had never imagined I would see my mother burning at the crematorium on the deformed iron stand on a video call. COVID-19 patients are deprived of the personhood and so are their suffering families.
References
Cassell, Eric J. “The Nature of Suffering.” The Nature of Suffering and The Goals of Medicine. New York: Oxford University Press, 1991, pp. 30-47.
Daniels, Norman. “Health-Care Needs and Distributive Justice.” Philosophy & Public Affairs, 10.2 (1981), pp. 146-179.
Mishra, Naina. “Second wave: Covid patients see rapid fall in oxygen level.” Tribune News Service, 21 April 2021, https://www.tribuneindia.com/news/chandigarh/second-wave-covid-patients-see-rapid-fall-in-oxygen-level-242247. Accessed 12 May 2021.
Swati Joshi is a doctoral candidate working on Medical Humanities at the Indian Institute of Technology Gandhinagar. Prior to joining Ph.D., she has worked as a Lecturer of English Literature at St. Xavier’s College, Ahmedabad.