Evidence from Natsal-3 published in BMJ Sexual and Reproductive Health showed that women need contraception from doctors, but men largely get it from the shops. For many of us, this kind of disparity tends to set off our sexism alarms.
In some ways the results are a natural consequence of biological differences. Men tend to use barrier methods which are anatomically convenient. The only major long-term contraceptive for men is the vasectomy, but irreversibility is rightly seen as a huge barrier.
Having said that, the demedicalisation of female contraception – to some degree – certainly seems to be feasible. Research presented at the Annual Scientific Meeting of the Faculty of Sexual and Reproductive Health explored the possibility that pharmacists could provide women with contraceptive services without the input of a doctor. This has the potential to move women’s contraception out of the doctor-patient relationship and onto the high street.
But is medicalisation so bad? People using contraception will make decisions based on intuitions, preferences, and word of mouth, but healthcare professionals have a duty to convey information about the evidence base. The Gynae Geek by Dr Anita Mitra describes itself as “a user’s guide” to the female reproductive tract, and it includes a table of clear information about contraceptive choices. That is crucial medical work. Similar information is presented on the Contraception Choices website.
Tables and diagrams like this allow professionals to share evidence in straightforward ways. As long as evidence is clear, up-to-date and readily available, this is the kind of area where women can make their own decisions.
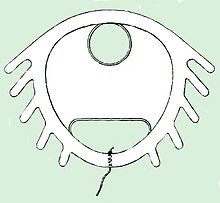
However we cannot always assume that the evidence will be clear and available. That’s why Dr Mitra’s book and the Contraception Choices website are so crucial. In the 1970s many doctors enthused about the Dalkon Shield without adequate scrutiny of the evidence. The Dalkon Shield was an intrauterine device which its inventor, Dr Hugh J Davis of Johns Hopkins University, claimed was remarkably effective compared with the competition. His claims appealed to the American government which was concerned about an impending post-war overpopulation crisis and conveniently allowed him to make large amounts of money from Dalkon Corporation.
But his data was bad. His follow up averaged only four and a half months across 640 women. Over time, reports of high levels of pelvic inflammatory disease began to surface but the company was slow to act. It became clear that both the safety and efficacy of the Dalkon Shield had been overstated beyond the supporting evidence.
The tensions between good science and practical law were highlighted when affected women took the company to court. After years of insisting that the evidence was in their favour, the company’s lawyers began to claim there was an ambiguity about safety. This ambiguity was used to claim that it was uncertain whether women who had become infertile after using the Dalkon Shield would not have become infertile anyway, and thereby dodge tortious liability.
“’They have their experts, we have ours”, claimed one spokesman, exemplifying how power is used to abuse science, create doubt and uncertainty, rather than argue for positions of evidence-based truth.
Dr Hughs can be credited with one great victory for evidence-based contraception, however. His obituary in the New York Times attributed federal laws requiring FDA approval for medical devices to his failure to adequately test his product before going to market.
Ensuring that patients and doctors have up-to-date and relevant evidence is a Sisyphean project where prestige, money and politics always threaten to undermine our best efforts. The topic of this year’s Healthwatch conference, on 17th June, is “Evidence, healthcare and medical devices & implants”. It’s highly relevant to those of us placing implants, IUDs and coils. Tickets are available here: www.healthwatch-uk.org/symposium2019-tickets