This is the seventh blog by Dr Ammara Hughes on Primary Care Leadership and COVID vaccination. Read the first, second, third, fourth, fifth and sixth blogs in the series.
Three years ago, I ran my first marathon. As runners will know, this generally comprises of a four-to-five-month training programme, which becomes all consuming. You fit the runs around your daily schedule of work and domestic commitments. Whatever the weather, no matter how tired you are, you have to stick to and trust the plan. Above all else, you do not skip that Sunday long run, or the “SLR”.
The COVID vaccination programme is a bit like marathon training. Slow and steady but must fit around other commitments.
At the beginning, everyone was raising their hand to run a COVID vaccination hub. FOMO (fear of missing out) was evident. This vaccination programme was the talk of the land, not just the town. The set up was at sprint pace, but at some point, it had to be about endurance.
The deal was to set up the sites using existing workforce. A tall order in a profession with shortages, struggling to recruit GPs and nurses. The standard operating procedure (SOP) stipulated GPs as the vaccinators. (A word of advice. If you need a vaccine, the last person you should go and see is a GP. We just don’t do enough of them. But maybe the powers that be think we’re masters of everything).
In a war-like call to arms, GPs were encouraged out of retirement to help their country in its time of need. They were rewarded for doing so with a suite of online training modules, which reminded them all why they had retired in the first place. But the brave soldiers battled their way through the thick fog and made it out the other side intact.
This still wasn’t enough. We needed more hands on deck. Medical students! St John’s Ambulance volunteers! Fast track vaccination training programmes were set up around the country, and before long, proud volunteers were ready to go at mass vaccination centres. Beaming smiles on TV when their journeys were filmed and broadcast.
Raj Gill, our lead physician associate and workforce lead for the Primary Care Network, had an alternative plan.
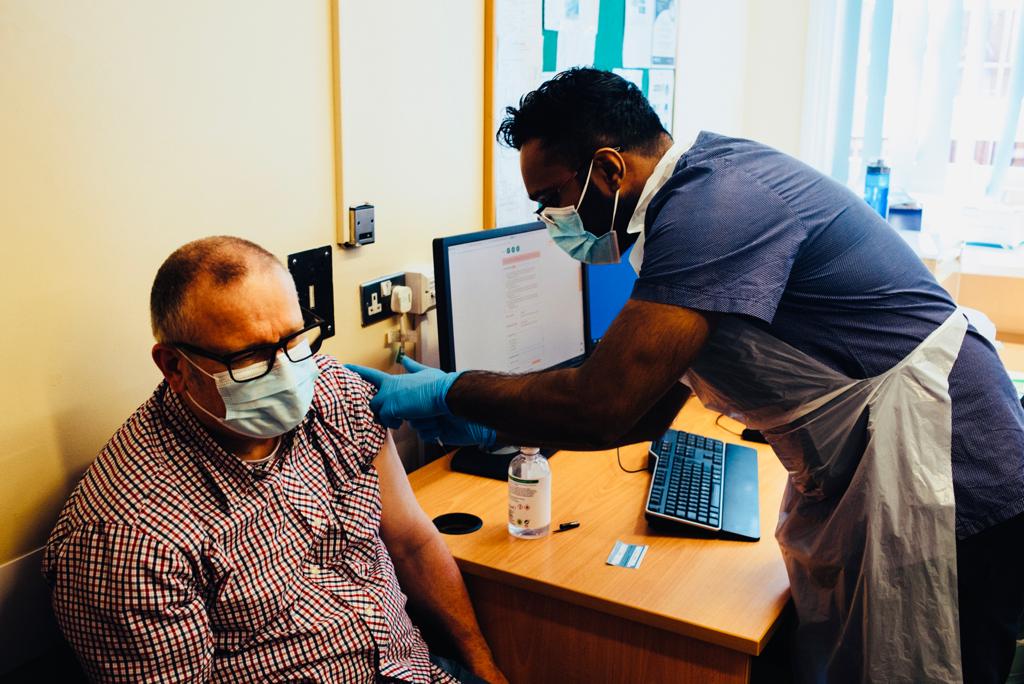
Physician associates (PAs) have been part of the medical profession in the UK for the best part of a decade. In the USA, their equivalent, the physician assistants, have been around for nearly 50 years. The recognition of PAs and their role in General Practice was really cemented with the introduction of the Primary Care Network (PCN) model in 2019. Significant investment was put forward to support groups of GPs to appoint such health professionals. Some of us were ahead of the curve though and had been appointing PAs for some time. Raj has been with us for eight years and is also now a partner, thanks to some forward-thinking GP colleagues. With his experience comes a network of PAs wanting to join our PCN, as many practices are still preferring a more traditional model of General Practice. PA students are desperate for GP placements, because practices aren’t quite sure how to accommodate them, or remain sceptical about the value they bring. We have no such hesitation and welcome our PA students with open arms.
This reputation helped us launch our vaccine hub. We were bold enough to offer an alternative to the model laid out in the SOP. It was a bit of a headache for commissioners to sell this one to NHS England. The proformas didn’t really allow for this scenario, which resulted in many phone calls and emails to see why deviation from the command was necessary.
It was really simple. Rather than GPs, we would use physician associates to staff the hub and be the vaccinators. As a PCN we had appointed PAs who were working in our practices daily. They were routinely giving vaccines, so we couldn’t see any reason why they couldn’t give COVID vaccines. They were “existing workforce” and were more experienced than the newly qualified fast tracked vaccine volunteers.

GPs would supervise and sign off each PA as a vaccinator and each vaccine would be given under a “patient specific direction” or PSD. A PSD is needed if the vaccinator is not a prescriber and is effectively a prescription authorised by another prescriber. (For some reason, PAs do not yet have the go ahead to prescribe, despite formulating management plans every day).
After some in depth quality assurance visits and questionnaires, we were allowed to proceed on the basis that a GP was present at all times to supervise. I observed each PA draw up and administer five vaccines. (I have no qualms in telling you that only a PA was allowed to give me my COVID vaccine! I politely declined the kind offer of my fellow GPs).
Four months in, our own army of PAs allows us a sustainable model for the vaccine hub, as we are not pulling our GPs or nurses out of practices. Or indeed any other health professional. Our PCN practices can get on with the day job, while the PCN clinical directors, workforce lead and PAs continue the marathon that is the COVID vaccination programme.
Acknowledgements
Thanks to Raj Gill and his army of physician associates, Stanley Bell, Tripti Chakraborty, Chanceeth Chandraknathan, Shameem Dukandar, Zein Hussain, Rebekah Ohene, Vidhi Patel, Amy Perrott, Lydia Warner, Natasha Warner and Nasra Yusuf, for being the frontline of our vaccination hub.
*Photographs posted with permission, courtesy of Oli Sones

Dr Ammara Hughes
Dr Ammara Hughes MBBS MRCGP (2004) is a GP partner at Bloomsbury Surgery, Central London, and co-Clinical Director, Central Camden PCN and a member of the NHS Confederation PCN network. She qualified as a doctor from Charing Cross and Westminster Medical School in 1996. She spent 8 years in hospital medicine in London, before becoming a GP in 2004. She has been in leadership in the NHS since 2007. She was an elected Governing Body GP member of Camden Clinical Commissioning Group from 2011-2017, serving two terms. Since then, she has undertaken provider lead roles. She was Vice Chair of Camden Health Evolution from 2017-2019, stepping down to take on the role of Clinical Director of Central Camden Primary Care Network.
Declaration of interests
I have read and understood the BMJ Group policy on declaration of interests and declare the following interests: none.