Authors: Rhys Jeffries; Simon Barry; Laura Wallis; Chris Davies and Mark Taubert
on behalf of the Respiratory Health Implementation Group Wales, the Institute of Clinical Science and Technology, Velindre University NHS Trust and the NHS Wales Health Collaborative, Cardiff, UK.
Guideline website: https://covid-19hospitalguideline.wales.nhs.uk/
Introduction: It became evident in early March 2020 that clinical practice in managing COVID-19 varied markedly across the UK and even at local level. The evidence-base on how to manage the pandemic in all areas, including intensive care medicine but also palliative care, was scant. It was therefore important to bring clinicians across Wales together to create a national approach to the management of COVID-19 that was adaptable and responsive, reflecting the likely changes in management as the pandemic unfolded and new evidence emerged. This ranged from initial assessment at the front door, to management in ITU and acute palliative care approaches in order to minimise symptoms and distress. This guideline needed to be compact and simple, built on core principles, accessible to all healthcare staff via smart phones, tablet devices or computers, and inclusive of the clinical leads across the country to reduce the barriers to adoption, thus facilitating the implementation process.

Implementation: Our team designed, developed, disseminated, and implemented an electronic National COVID-19 Hospital Guideline to support healthcare professionals to respond to admission demands during the COVID-19 pandemic.
The guideline features a universal, evidence-based and regularly updated pathway for assessment, triage and management of patients presenting to hospital with COVID-19. Additionally, it is supported by a digital platform hosting video-education delivered by experts across all parts of NHS Wales, ranging from intensive care to palliative care doctors. Whilst the guideline framework does not change (fixed ‘flow through the system’ component), the clinical processes are dynamic, with updates delivered in a video format accessed through QR readers on colour-printed guideline posters and via email updates, as the disease burden and trajectory changes.

Bespoke implementation software developed by the Institute of Clinical Science and Technology (ICST) enables local level invitations encouraging engagement with the guideline platform. We believe that this is the first time ever that such a national guideline has been created, following the principles of implementation science.
Our analysis shows that this national guideline has influenced the clinical behaviour of healthcare professionals across all hospitals managing admissions of COVID-19 across Wales. User feedback has been collated throughout and acted upon. Ratings have been favourable, with an overall rating of 4.1/5, with over 80% of respondents from across Wales wishing for email updates to continue. Guideline platform activity has been commensurate with the trend in hospital admission rates across Wales and with the number of COVID-19 cases and deaths. We have recently (November/December 2020) seen increased activity as the admissions gradually rise again.
What does it look like?
There was no existing exemplar way of working in what has become a sustained, global pandemic. Much of this is pioneering work was based on evidence from previous viral outbreaks including SARS and MERS, but also management of acute respiratory distress syndrome. The dynamic elements of the guideline have had 18 updates as the clinical information has changed, and are evidence-based and consistent with UK guidance such as NICE. Palliative Care guidelines have taken into account an All Wales bereavement survey and a large project is underway to examine the impact of Covid-19 related bereavement, which will impact on some of the areas of our guideline that deal with death and dying, and the appropriate aftercare.
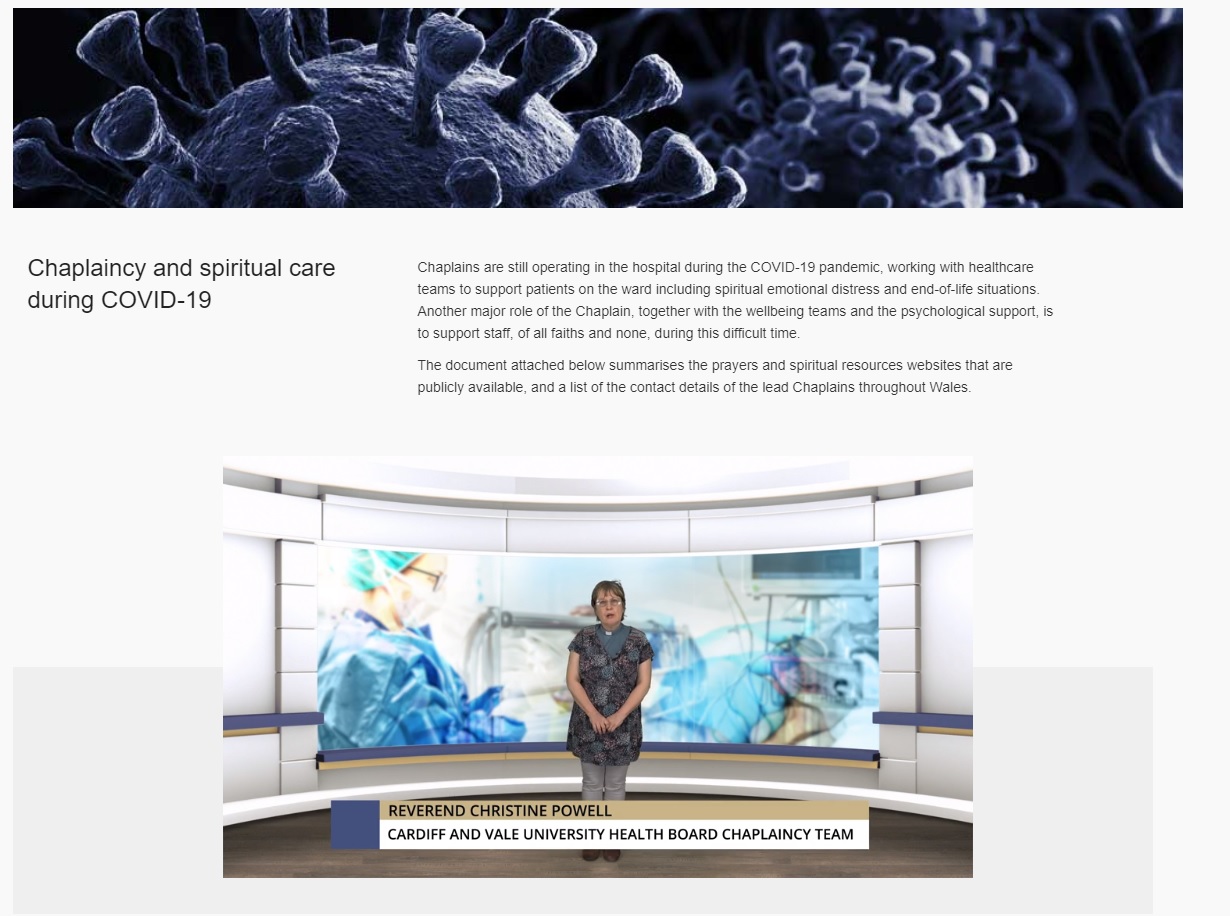
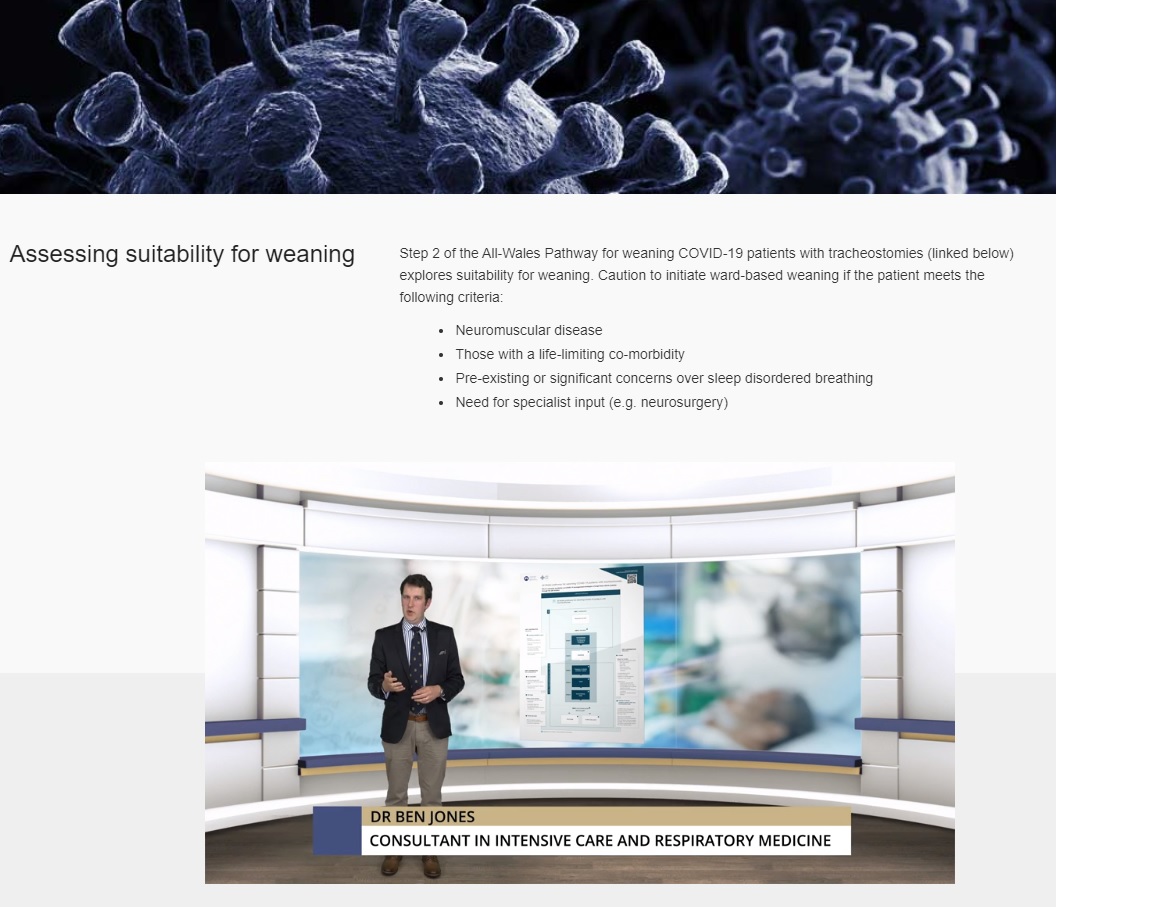
The platform now hosts over 150 instructional videos delivered by clinical specialists and allied health professionals across Wales. They act as a ‘tutor in need’ with quick, snappy updates on topics such as, managing severe breathlessness or agitation due to Covid-19.
Guideline adherence continues to be analysed through implementation data and user surveys. A large multi-centre clinical audit has been undertaken, the findings of which will update the guideline. The guidelines, videos and website were set up in a matter of weeks and were delivered free of charge. Professionals from all walks of life came together to give their time, work on guidelines, review of the literature and appear in videos. Crucially, this serves as a model to approach similar programmes of work for the future, such as a recently proposed community and primary care guideline for the management of COVID-19.
Within four weeks, 4,500 hospital clinicians nationally were registered and receiving updates. Amongst these, there were mainly senior clinical decision makers (medical directors, consultants and registrars).
Recognition:
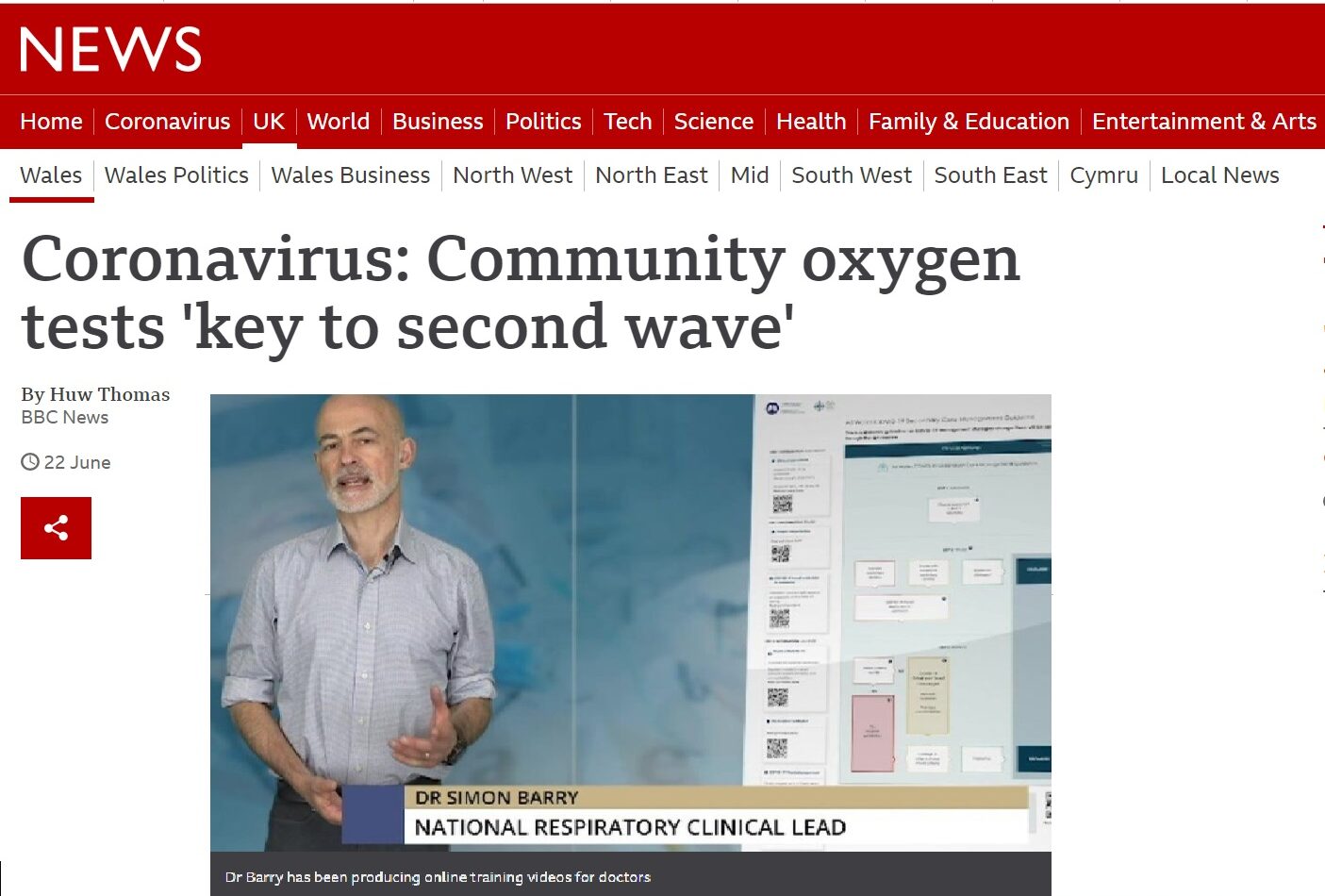
The British Lung Foundation and Asthma UK, the British Thoracic Society, and various multi-professional clinical groups have endorsed and promoted this guideline. It has received acknowledgment in the form of a national award, MediWales Winner 2020 for Best Scaling up of Innovation and Transformation (video link). It has featured on the BBC Wales News as an innovative approach to COVID management and our user-data shows that is being accessed from not just the UK, but the rest of the world as well.
The second wave of the pandemic will present a further scaling up of this innovative resource; the guideline will increase notifications and instructions to support clinical and managerial staff on the wards and at the coalface in hospitals, hospices and community settings across Wales.
The Intensive Care National Audit & Research Centre (ICNARC) report shows that ICU mortality in Wales is lower than the UK average. Coinciding with these outcomes, Wales has one of the lowest mortality rates in the UK for COVID-19 during the pandemic thus far, according to the Office for National Statistics. The potential we have in Wales to deliver in a collaborative manner has been used to full effect in this huge project. There is now also a primary care version which can be accessed here. For further information please click here.