A quality improvement programme for psychiatry trainees
Dr Clare Trevelyan and Dr Liz Ewins
Quality improvement (QI) is increasingly at the forefront of postgraduate professional skills development. The 2013 Francis report highlighted a need for a culture of collective leadership, and trainees as important agents of change1. However, QI has not yet been fully embedded in psychiatry training. In 2014, the Medical Education Department at Avon and Wiltshire Mental Health Partnership NHS Trust (AWP) created a team to develop a QI programme as they were keen to use the energy, enthusiasm, and talent of trainee doctors to address areas for improvement in the clinical and educational environment. This team was spearheaded by advanced trainees working as clinical teaching fellows.
The programme we developed offers trainees resources, training, project supervision, and coaching, collaborating with the Trust’s Quality Academy to create coordinated project governance procedures. Prior to this programme, no trainees in AWP were involved in QI projects. Seventy-six percent of core trainees and 60% of advanced trainees were involved in QI between 2014 to 2016, and it has become embedded as a necessary part of the Severn School of Psychiatry ARCP.
Our trainee QI projects have focused on improving safety, efficiency, and patient experiences. They have developed from a grassroots level, driven by areas for improvement identified by trainees. This has included improving multidisciplinary team communication processes and documentation, physical health training, improving liaison referrals, and patient feedback processes. Projects have also addressed Trust and Deanery level quality priorities, including improving medical handover across the Deanery, and developing professional guidance for the Place of Safety (136 suite).
Trainee projects have achieved national publication and poster prizes, and feedback indicates trainees are engaged and enjoying QI work. Through the involvement of trainee doctors and the Quality Academy’s drive to QI, there has been a shift in culture with increasing numbers of senior doctors and the wider multidisciplinary team becoming involved. We hope that this programme will help develop medical leadership with a sound understanding of effective improvement methodologies.
How we set it up
This project got started when the AWP Director of Medical Education (DME), Dr Steve Arnott, approached Dr Liz Ewins at the start of her year working as a teaching fellow for the Trust and asked her if she would set up a QI programme for trainees. Liz was able to access local academic expertise at the University of Bristol and Severn Deanery, including the Head of School Dr Rob McPherson, to help her develop ideas for the programme by using it as the subject of an Educational Fellowship awarded by Severn Deanery. Along with her supervisor Dr Geoff Van Der Linden and AWP Medical Education Project Manager Bridget Kelly, Liz adapted training strategies employed by the local Foundation School2 and the Royal College of Physician’s ‘Learning to Make a Difference’ programme3 to develop training and support to enable psychiatry trainees to undertake their own QI projects within the Trust.
A half day training session was developed to teach trainees about QI and project methodology, including using PDSA cycles in practical examples so that they could undertake their own projects. This was delivered by Liz alongside the Quality Academy local lead. Trainees were encouraged to come up with their own ideas for projects and to work with other trainees to implement changes, under the supervision of a higher trainee, specialty doctor, or consultant. They were asked to include the wider multidisciplinary team in developing and implementing projects, to support successful and sustainable changes.
Training was initially targeted at trainees, but a growing number of specialist doctors and consultants requested to attend and they were invited to a second training session. A resource handbook was developed and a series of short follow-up sessions were put in place to provide further advice about QI methodology and to help support trainees’ projects. Trainees were asked to register their projects by completing a short online form on the Trust Quality Academy website so the Trust could monitor participation.
During the pilot we found that forming close links with the Trust Quality Academy provided invaluable assistance in setting up the scheme and supporting training. They have been particularly helpful when offering guidance regarding governance and what permissions might need to be sought. Key to this process has been the support from Trust medical management leads (including the Medical Director and DME) and work by the Deanery to embed QI alongside audit into ARCP requirements.
After this successful launch, the next teaching fellow in post, Dr Clare Trevelyan, took on the role of trainee QI lead for 2015-16. The team worked with the Quality Academy to develop the governance structure and online registration process for projects. We have continued to develop training sessions on QI methodology as part of the Core Training Course for psychiatry trainees, as well as offering sessions at Local Academic Programmes, developing, and delivering workshops for the AWP Excellence in Education and Excellence in Quality Improvement conferences. During this second phase we have built up strong links with the West of England Academic Health Science Network (WEAHSN), who have helped us deliver training to senior medical staff and clinical leads. In June 2016 we helped develop and deliver a regional QI conference for all staff in the South West, “QI in Action”, in collaboration with Health Education South West, WEAHSN, and the South West Academic Health Science Network.
Challenges
One of the key challenges has been how to sustain successful changes and embed them within teams as trainees rotate through posts. Is this the responsibility of the central QI team or should it be handed to the localities? Our approach needed to be flexible for different projects. We also noticed that the same sorts of projects were getting registered all over the Trust, but getting these projects linked up to share learning was easier said than done. There needs to be development of how we link trainee grassroots projects with Trust priorities, and we also need to increase service user involvement as co-production is a key concept in QI. We are considering achieving this through the introduction of suggested projects in training sessions.
The ability of medical education to offer effective coaching to all trainee projects as the scheme developed was limited by available expertise and time. The project team were keen to keep trainee project governance within Medical Education rather than the Quality Academy so we could tailor support and training for the particular needs and ambitions of the trainee doctor. However, approving, supervising, and chasing up projects and their reports is time consuming. This has until this year been carried out by one teaching fellow with support from Bridget Kelly, but this may no longer be feasible as the project expands. Indeed it may no longer be desirable to keep trainee projects separate as projects involve more and more of the multidisciplinary team.
Top tips
Build key relationships with potential QI champions. This has been really important in building momentum and senior buy-in for the programme. The project has been well supported by key figures in the Medical Education department (where it is housed) but also at the Deanery and the Trust Quality Academy. There is no substitute for face to face meetings.
Make use of the wealth of resources out there. We have worked with the West of England Academic Health Science Network (WEAHSN) and inviting their experts to contribute to our training sessions; this has been incredibly valuable and important to ensure the quality of the training we can offer. We have attended QI training events around the country and discovered ideas for our own training, as well as using free resources for healthcare professionals available through the Health Foundation and Institute for Healthcare Improvement website (www.ihi.org).
Make a big deal out of project successes. Everyone wants to hear about this! Take any opportunity to support trainees in presenting their work internally and externally, and spread good news about prizes and publications. Get project updates onto the agenda for Trust management meetings such as Trust Medical Advisory Groups. Not only does this increase morale but also increases interest and awareness in QI and its potential.
Enjoy QI! To combat the change fatigue that NHS staff can experience you need a good dose of enthusiasm; this starts with the QI team. It’s all about communicating why QI is such an important and empowering tool for healthcare professionals, enabling front line staff to make a difference in improving patient care and experience.
References
- Francis, R. (2013) Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry. London.
- Bethune R, Soo E, Woodhead P, Van Hamel C, Watson C. Engaging all doctors in continuous quality improvement: a structured, supported programme for first-year doctors across a training deanery in England. BMJ Qual Saf 2013; 22(8):613-7.
- Vaux E, Went S, Norris M, Ingham J. Learning to make a difference: introducing quality improvement methods to core medical trainees. Clin Med 2012; 12(6): 520-5.



 Morven Millar 3rd year Medical Student University of Dundee
Morven Millar 3rd year Medical Student University of Dundee
 Biography
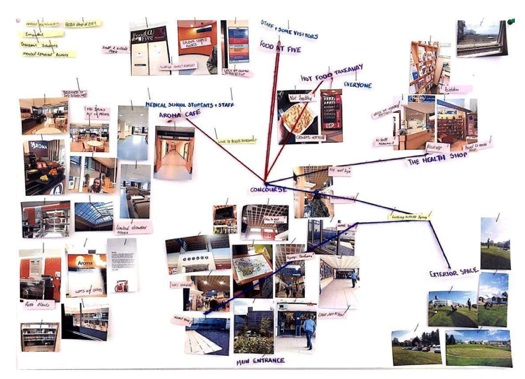
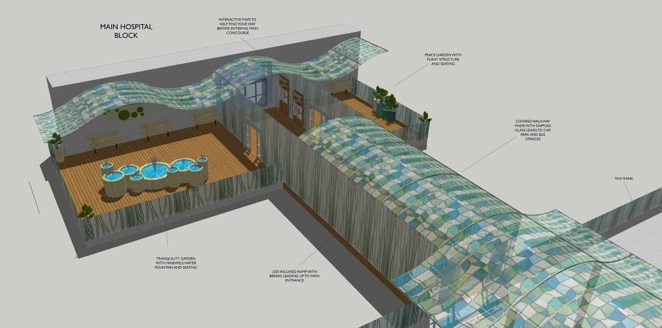
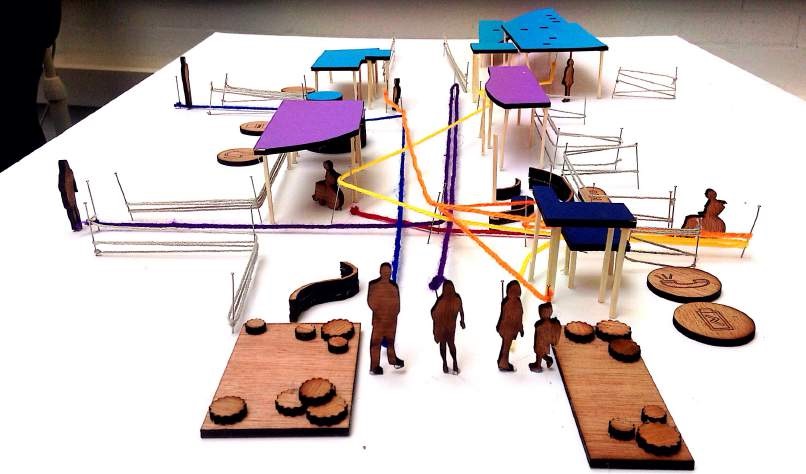
Biography what really matters to users, and employ the narratives to inform patient focused service
what really matters to users, and employ the narratives to inform patient focused service 
 Dr Howard Ryland is a Registrar in Forensic Psychiatry at South West London and St George’s Mental Health NHS Trust. He was previously National Medical Director’s Clinical Fellow at the Academy of Medical Royal Colleges and the Vice-Chair of the Academy’s Trainee Doctors’ Group. He is a member of the Academy’s Quality Improvement Task and Finish Group.
Dr Howard Ryland is a Registrar in Forensic Psychiatry at South West London and St George’s Mental Health NHS Trust. He was previously National Medical Director’s Clinical Fellow at the Academy of Medical Royal Colleges and the Vice-Chair of the Academy’s Trainee Doctors’ Group. He is a member of the Academy’s Quality Improvement Task and Finish Group.