In the last few years, the role of neuroinflammation has been established as a relevant pathophysiological mechanism in multiple neurodegenerative diseases. Specifically, in ALS, activated microglia contribute to the non-cell autonomous neurodegeneration of the motor neurons. Moreover, there is no doubt that biomarkers for ALS diagnosis, prognosis and clinical trial stratification are needed.
In the March issue of JNNP, Steinacker and colleague explored the potential use of a marker of microglia activation, chitotriosidase (CHIT1), in the differential diagnosis and prognosis for ALS patients. The authors analyzed the CHIT1 concentration in CSF and serum from patients with ALS. This was compared with bio-fluids obtained from ALS mimics and a wide range of neurodegenerative diseases, including Alzheimer disease (AD), frontotemporal dementia (FTD), Creutzfeldt–Jakob disease (CDJ) and Parkinson´s disease (PD). The authors found that ALS patients displayed significantly higher levels of CHIT1 in the CSF compared with healthy controls, ALS mimics and most of the neurodegenerative diseases, excluding CDJ. Interestingly, the highest CHIT1 levels were found in patients with a rapidly progressive ALS form. In keeping with this finding, CHIT1 level correlated with ALS severity and disease progression, however not with survival. CHT1 blood levels were similar between ALS patients and any other study group. Finally, the brain tissue analysis revealed overexpression of CHIT1 in the spinal cord of ALS patients, specifically in the microglia and macrophages.
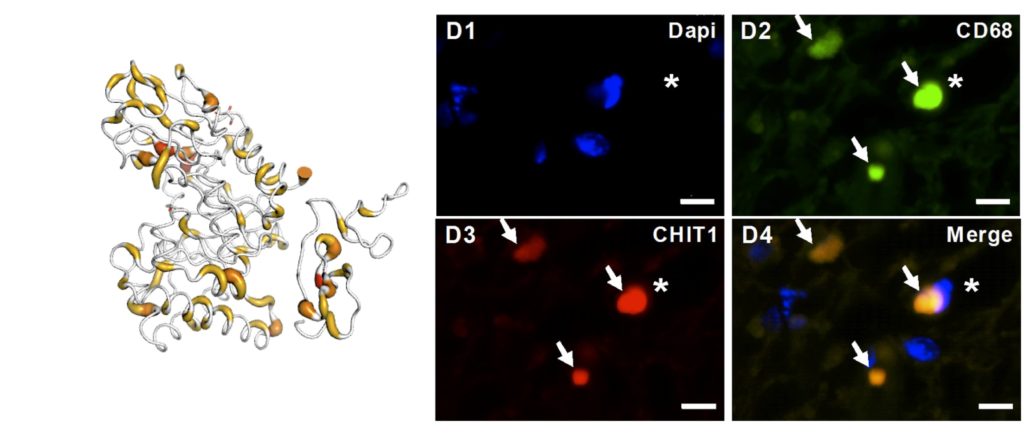
This study confirmed higher levels of CHIT1 in the CSF of ALS patients compared with ALS mimics and other neurodegenerative diseases, potentially originating due to microglial activation in the spinal cord of ALS patients. This interesting finding may suggest that microglial activation is an essential feature of ALS pathogenesis, and a possible therapeutic target. Further cross-sectional and longitudinal studies are now needed to define the potential use of CHIT1 as an ALS biomarker, confirm these findings and define the specific criteria for CHIT1 increase in disease and changes during disease progression. Finally, it would be fundamental to define its utility in patient stratification, especially for clinical trials focused on immunomodulatory strategies.
Read more at http://jnnp.bmj.com/content/89/3/239