Professor El-Omar has chosen Professor Michael Bourke from the Department of Gastroenterology and Hepatology and Westmead Hospital and Clinical School, University of Sydney, Sydney, New South Wales, Australia to do the next #GUTBlog.
The #GUTBlog focusses on the latest paper “Piecemeal cold snare polypectomy versus conventional endoscopic mucosal resection for large sessile serrated lesions: a retrospective comparison across two successive periods” which was published in paper copy in GUT in September 2021. Professor Bourke is the senior author on this paper.

Professor Bourke writes:
“Cold snare polypectomy (CSP) is now scientifically established as the preferred technique for the management of small (<10 mm) colonic polyps. These lesions rarely contain high grade dysplasia and the majority will not progress to cancer, therefore safety is of paramount importance in their management. Effectiveness is also important, as nonetheless, it is well recognised that advanced neoplasia and cancer may develop in colonic segments where small polyps have been resected previously, possibly reflecting prior incomplete resection. The widespread adoption of CSP and it’s clinical practice still remains to be optimised in the broader endoscopic community. Fundamentally, because it is so inherently safe, it should be the safest and generally preferred polypectomy technique undertaken by any endoscopist. The major risks of polypectomy are post procedural bleeding and perforation. When CSP is applied to small polyps these risks are essentially absent. All endoscopists should embrace the catechism: when applying CSP for flat colon polyps, if in doubt, resect more, as much as you comfortably need to ensure complete excision. Such an approach improves efficacy without imposing risk. In my practice, for more than a decade, I aim for the post CSP mucosal defect to be at least double the size of the lesion. These considerations led our group into thinking about utilising the CSP technique for the endoscopic excision of other types of lesions.
Large (>20mm) serrated lesions (LSL) present as ideal candidates for CSP. Their low, soft and flat mucosal profile offers an ideal substrate for smooth transection by a cold snare. They are premalignant and require complete, preferably recurrence free, endoscopic resection to mitigate this risk. Previously this has been achieved by conventional colonic endoscopic mucosal resection (EMR). However, this imposes a risk of delayed post EMR bleeding of 5-7% and a small risk of perforation of <1%. This latter risk is greatly minimised by careful informed inspection of the post EMR defect utilising the Sydney deep mural injury (DMI) classification system, also published in GUT. DMI types 2-5 are closed with clips. Bleeding risk may be minimised by clip closure of the defect. However, much better than suffering these anxieties and risks, would be to avoid them altogether, especially if clinical effectiveness was comparable. Hence the investigation of CSP in the management of LSL.
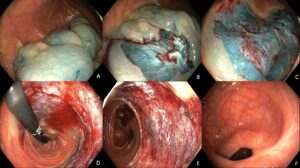
Since mid 2008 all large (>20mm) non pedunculated colonic polyps (LNPCP) referred to our centre for endoscopic management are enrolled in the Australian Colonic Endoscopic Resection (ACE) study. My hospital, Westmead, Sydney is the lead site and recruits approximately 60% of the cases. Multiple clinical and technical variables are included in the data at the first visit and in scheduled follow-up. We have more than 5000 cases to date. Approximately 15% of referrals are LSL. Commencing in 2016, these cases formed the basis for this study.
I was convinced that piecemeal CSP (P-CSP) was the best approach for this unique type of lesion. Based on our earlier experience it was clear to me that there was not equipoise for safety between P-CSP and EMR and thus ,with the support of some of the other ACE centres, it was decided to perform a prospective observational study in comparison to our previous published experience with conventional EMR (also published in GUT). The results were overwhelmingly in support of piecemeal CSP. No adverse events and comparably very low recurrence at 6 and 18 month surveillance, around 4 and 1.5% respectively. This experience precedes the emergence of thermal ablation of the post EMR margin which has driven the risk of adenoma recurrence at surveillance to very low levels, of the order of 1.5%. This study of P-CSP for LSL has cemented the technique as the preferred method for the management of LSL.
Obviously, the next question is what role P-CSP may have in the management of large flat adenomas. Undoubtedly it will certainly mitigate the risk of adverse events, but will recurrence rates be unacceptably high. Albeit, we have shown that recurrence is easily managed endoscopically. It is certainly an exciting time to be working in this field.
Optimal technique is critical to optimise outcomes. A full discussion of that is beyond the scope of this #GUTBlog, but please stay tuned to our further work.”