Pauline Brown is Lead Research Nurse for the Multi-Specialty Research Delivery Team at Gloucestershire Hospitals NHS Foundation Trust. Pauline has worked in research delivery for 13 years, she is passionate about professional learning, development, and quality improvement and recently qualified as a Professional Nurse Advocate.
The roll out of the Professional Nurse Advocate (PNA), following the success of the Professional Midwifery Advocate (PMA), refreshed my understanding of clinical supervision and the importance of midwives and nurses taking time out to think, enabling them to make the best decisions. The A-EQUIP model (Advocating for Education and Quality Improvement) represents the areas of responsibility of the PNA, and follows Proctor’s model of clinical supervision with its normative, formative, and restorative elements with the addition of personal action for quality improvement (NHS England and NHS Improvement, 2021).
Perhaps we as nurses need to accept that spending time with our colleagues to share practice, concerns or needs is not an extravagance but a necessity. The PNA role can facilitate that, supporting staff to gain confidence and competence through learning and development both individually and as groups though clinical supervision (Carter, 2022). This in turn supports our wider teams and excellence in patient care.
How can the PNA support clinical research delivery teams?
We know that staff new to research delivery experience a steep learning curve. Junior research nurses or coordinators are still developing their professional skills and confidence, they need to quickly adapt to a new way of working unlike any previous role in a clinical setting, whilst tackling the world of research. Working in a multi-specialty research team in particular demands rapid learning of patient pathways and building relationships with new clinical teams. In a previous BMJ blog Research Delivery was described as a speciality in its own right (Aldridge, 2020).
The real challenge for many research delivery colleagues is the autonomy of coordinating research projects. Staff can be part of a supportive team of colleagues but also work independently with individual responsibility for coordinating allocated studies, and it can be difficult to fully appreciate each other’s work demands. We need to encourage our staff to slow down, reflect and process thoughts to help see different perspectives.
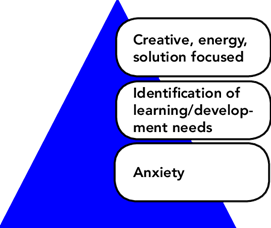
Figure 1 The restorative clinical supervision model (Wallbank 2007)
The Restorative Clinical Supervision model by Wallbank (2007) (figure 1) demonstrates our need to firstly address any anxiety within our work to allow us to identify learning and development needs, which then creates space for creative thinking. Restorative clinical supervision is not a new concept but if not fully understood it might not be accessed as well as it could be. I introduced the idea of clinical supervision to my own delivery team through our journal club and an article by Butterworth (2022). Butterworth suggests that while there might be some confusion over how to apply clinical supervision there is no one way to deliver it, and there is certainly evidence to support its effectiveness.
As a team leader I strive for learning and improvement to be part of our team culture. This means creating the time and space for staff to learn and develop rather than adding it to their to-do list. Restorative Clinical Supervision through the support of a PNA can provide the opportunity for staff to think about personal development as well as supporting service change.
It’s not only new research delivery staff or research nurses who might benefit from restorative supervision. While the nursing profession may dominate clinical research delivery teams in many organisations, there are an increasing number of health professionals taking up dedicated roles in research delivery as well Clinical Research Practitioners (CRP’s), all of whom will have a different set of learning and development needs while carrying out the same or similar roles (NIHR, 2023). Research delivery leaders also carry out unique roles, particularly if employed in smaller organisations or research departments. Linking with others in similar roles for supervision could offer reassurance, support, and reduce feelings of isolation. This could all be doable within our regional NIHR Clinical Research Networks through remote meetings.
Research delivery staff are a growing workforce. Staff retention is one of the key outcomes of the PMA and PNA programme along with improved staff wellbeing and improved patient outcomes (NHS England and NHS Improvement, 2021). If we want to support, develop, progress and retain our research delivery staff at all levels we need to offer more than research skills training.
Find out who the PNA or PMA’s are in your own organisation to access support for you or your team, or ask your professional development team how to access PNA or PMA training.
References
Aldridge N (2020) Clinical Research Delivery Teams and the Covid response: defining a new specialty. https://blogs.bmj.com/ebn/2020/08/17/clinical-research-delivery-teams-and-the-covid-response-defining-a-new-specialty/ (Accessed 2 May 2023)
Butterworth T (2022) ‘What is clinical supervision and how can it be delivered in practice?’ Nursing Times [online]; 118: 2, 20-22 Available at: https://www.nursingtimes.net/roles/nurse-managers/what-is-clinical-supervision-and-how-can-it-be-delivered-in-practice-17-01-2022/ (Accessed: 25 April 2023)
Carter, V. (2022) ‘Can restorative clinical supervision positively impact the psychological safety of midwives and nurses?’, British Journal of Nursing [online] 31(15), pp. 818-820. Available at: https://www.magonlinelibrary.com/doi/abs/10.12968/bjon.2022.31.15.818 (Accessed: 2 May 2023)
NHS England and NHS Improvement (2021) Professional Nurse Advocate A-EQUIP Model. A Model of Clinical Supervision for Nurses https://www.england.nhs.uk/publication/professional-nurse-advocate-a-equip-model-a-model-of-clinical-supervision-for-nurses/ (Accessed: 25 April 2023)
NIHR (2023) Clinical Research Practitioners
https://www.nihr.ac.uk/health-and-care-professionals/career-development/clinical-research-practitioners.htm (Accessed: 2 May 2023)
Wallbank S (2007) Restorative Supervision Manual. Restorative Clinical Supervision Programme http://www.restorativesupervision.org.uk (Accessed: 25 April 2023)