Nicki Credland, Chair of the British Association of Critical Care Nurses; @credland_nicki

Critical care is an extremely stressful working environment. The specialty is often misunderstood, with a lack of appreciation for the complexity of critical care nursing. We know that it is a highly technical and constantly evolving environment and the continued professional development required to work in such an environment is significant. However, these factors have been shown to impact on the health and well-being of staff. Pre-COVID research suggested that one-third of critical care nurses experienced severe burnout, with 86 percent experiencing one of its three classic symptoms of exhaustion, depersonalisation and reduced personal accomplishment (Moss et al. 2016).
The COVID-19 pandemic has exacerbated the situation exponentially. Nurses were scared about contracting COVID themselves and taking it home to their families. Difficulties arising from access to and the uncomfortable nature of PPE, working long shifts, uncertainty about the management of COVID patients on the Intensive Care Unit (ICU), patient and relative distress and rising death rates all increased the intense emotional stress and trauma experienced.
Increased nurse-to-patient ratios have raised fears over nurses’ safety and that of their patients. In the United Kingdom, ICU capacity expanded by 2250 beds between January 2020 and January 2021. However, there has not been a matching increase in nurse staffing levels with ICU nurse-to-patient ratios increasing from 1:1 to up to 1:4 in some areas. The physical effect of this increased workload cannot be underestimated and as a consequence we see ICU nurses exhausted.
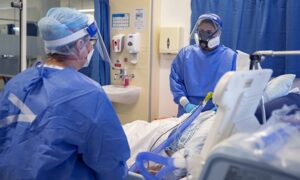
There is significant concern over patient safety when working at these extended ratios. Nurses are scared of making mistakes and of causing harm to patients through omission of nursing care due to volume of workload. Nurses report that that care becomes depersonalised, with a focus shifting to the completion of tasks rather than meeting individual patient needs. Nurses often talk about going home not feeling that they had done a good job. Others discuss feeling guilty or reporting that they “have nothing left to give”.
One solution to this increased workforce demand was to redeploy staff from other areas to support ICU nurses. These staff were deployed from theatres, wards, outpatients and diagnostic settings, often with little notice or preparation, and sometimes with little choice. Critical Care Nurse Educators worked hard to ensure as much support as possible was given to these staff under huge time constraints, and considerable national work focused on providing resources to staff suddenly “thrown in the deep end”. Their support has been outstanding and without them, the current situation would be even more grim, Again though, this solution came with consequences. Firstly, the redeployed staff were suddenly working in an alien environment. Whilst some flourished and have chosen to subsequently pursue an ICU career, many were terrified and have since vowed never to return. Secondly, these staff understandably needed close supervision, adding a layer of stress for ICU nurses. Now, not only did they have to care for increasing numbers of complex COVID patients with a high mortality rate, but had to do so whilst supporting healthcare professionals who had never worked in an ICU environment before.
Due to visiting restrictions, family members were unable to visit loved ones in ICU. This had a significant impact on staff who, especially at the end of life, played an increasingly extended role. I remember talking to one charge nurse who had looked after six patients, all of whom had died during a single shift. He sat with them all and spoke to each of their families via video link. He said he felt broken. He also knew that he had to go back to work the following day and “do it all again”. This cumulative effect has impacted on thousands of critical care staff. The feelings of guilt associated with patients dying, when added to the intense emotional stress faced daily, is manifesting as post-traumatic stress disorder at an unprecedented level throughout the specialty.
In response to these concerns, the World Health Organisation, in its Co-ordinated Global Research Roadmap 2020, calls for more research to support healthcare workers’ health and psychosocial needs. It is imperative that we shape proposals about how best to support nurses’ mental health and well-being reducing emotional burnout and pain at times of crisis such as pandemics. This absolutely must be a government priority as we move out of this pandemic. Simply put, we will fail to deliver effective care to patients if we fail to care for our staff.
Whilst the effect of the pandemic has taken its toll on the mental health and welfare of nurses, there have been some more positive impacts on the profession. Nursing, and critical care nursing in particular, has received a huge amount of media attention and increased its profile in a positive way. The public are much more aware of the critical role that nurses play in managing seriously ill patients. The ability to adapt and rise to the challenges faced has been inspiring. Nurses have led research, implemented evidence-based practice and delivered world class care under significant pressures to ensure that the patients come first. There is so much to be proud of and in turn so much to protect.
References:
Moss M, Good V, Gozal D, Kleinpell R, Sessler C (2016) An Official Critical Care Societies Collaborative Statement: Burnout Syndrome in Critical Care Health Care Professionals: A Call for Action Am J Crit Care 25 (4): 368–376.
World Health Organisation (2020) A Coordinated Global Research Roadmap WHO https://www.who.int/publications/m/item/a-coordinated-global-research-roadmap