Fit-for-the-Future, the ten-year plan for the English NHS, envisages a focus on quality and improvement driven by data.1 The plan acknowledges the wealth of data available nationally – including through clinical audits.1 Furthermore, new best practice guidance from NHS England argues for clinical audit contributing to a wider quality management approach.2
Historically, clinical audit is one of the main mechanisms for improvement in healthcare and is closely associated with quality assurance. More recently, approaches to quality improvement have been adopted into healthcare from other industries focussing on small-scale tests of change and learning – typically with measurement as a key element.3 Whilst tensions between clinical audit and other quality improvement approaches have been observed, both can work in synergy and clinical audit can play a key role in moving towards more systematic data driven quality management.2 4
Background: Clinical Audit and Quality Management
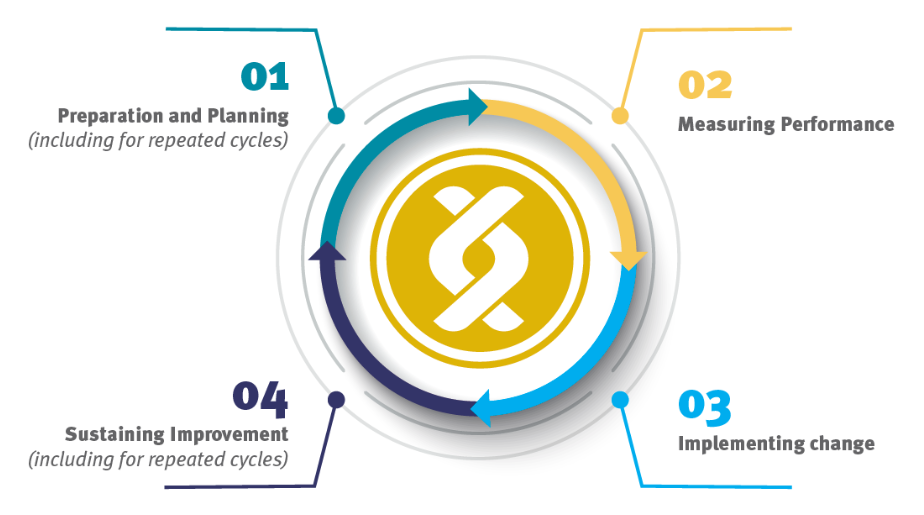
Continuous improvement is a long pursued goal in healthcare.5 A long standing approach to improvement is clinical audit. Clinical audit involves assessing services against evidence-based criteria and is considered the foundation of a well-functioning healthcare system. It is a cyclical approach that provides feedback upon which action can be taking on areas for improvement before re-auditing to assess the impact (see Figure 1 below).2 6 7
Improvement efforts are more impactful when part of a systematic approach.8 9 Quality management systems (QMS) are a means of systematically improving healthcare and embedding continuous improvement. A QMS combines a systematic approach to quality improvement (QI) with quality planning and quality control.9-11 Quality planning refers to how an organisation or system identifies its priorities for improvement and designs interventions to deliver them.10 Quality planning ensures close alignment of improvement activity with the strategic objectives of the organisation or system.10 11 Quality control refers to measurement of processes to monitor performance in real time and taking action to deliver results in line with performance standards.10 11 In addition to these three core components of a QMS, in healthcare a fourth component is included. Quality assurance focuses on checking whether a service is meeting required standards based on external requirements.9 11 Clinical audit can play a key role across such systematic approaches.12
Figure 1 – The Clinical Audit Cycle (HQIP 2020, used with permission)
“Data are critical to both quality improvement and quality assurance. When used effectively, data enable organisations to demonstrate measurable improvement at both the individual project and whole organisation level.”
Samantha Riley, Director of Making Data Count, NHS England
Clinical Audit and Quality Planning: Identifying opportunities for improvement
Clinical audit can support progress on national healthcare priorities by considering findings in planning activities. Clinical audit can contribute insights to service planning and commissioning processes by providing both cross-sectional benchmarking and longitudinal data.1 2 The national clinical audit and outcomes programme (NCAPOP) is one of the largest national audit programmes of its kind and can play a major role in the planning process and identification of improvement priorities.12 If healthcare priorities are to be evidence-based, clinically credible and focused on what matters most to patients, this data should shape how services are designed and inform which improvement priorities are selected. For example, the national mothers and babies audit (MBRRACE-UK) identified persistent inequalities in maternal and perinatal outcomes linked to ethnicity, deprivation, and geography. These findings enabled providers, commissioners and national bodies to prioritise targeted improvement efforts focussing attention on highest risk groups.13 14
Clinical Audit and Quality Improvement: Improving patient care and outcomes
Clinical audit is a quality improvement process that seeks to improve patient care and outcomes. A long-standing approach that has stood the test of time, clinical audit can continue to play a leading role in improving processes and outcomes nationally and locally. Through assessment against evidence-based standards for the structure, processes and outcomes of care, changes can be implemented where indicated and monitored to confirm improvement.7 Clinical audit also works alongside other popular approaches to QI – such as Lean and the Model-for-Improvement. These approaches support experimentation and testing in the ‘implementing change’ stage of the audit cycle.4 Therefore, if we want improvement that is data-driven, evidence-informed and clinically trusted, clinical audit should be central to any systematic QI approach. For example, the fragility fracture and falls audit programme (FFFAP) provides the national audit of inpatient falls (NAIF) which has seen improvements in its key indicators over the past six years. NAIF also provides resources to support local quality improvement projects.15
Clinical Audit and Quality Control: Ongoing measurement of quality
Clinical audit supports quality control processes by providing evidence of impact of changes introduced. In improvement work, to assess tests of change, a family of metrics is used comprising process and outcome measures.3 Audit is ideally placed to contribute to this and help improvement efforts to know whether changes lead to improvement. Whilst audits have been carried out previously at distal points in time, such as annually, there are examples of audits operating more frequently. With increasing focus on digital technologies, further shifts towards real-time audit are anticipated.1 For example, the paediatric intensive care audit network (PICANet) provides continuous, risk-adjusted monitoring of outcomes, allowing providers and national bodies to track trends in mortality, detect variation and identify emerging quality concerns.16
Clinical Audit and Quality Assurance: Evidence based compliance with standards
Quality assurance processes help organisations to understand care quality through periodic checks that particular standards are being achieved and addressing identified shortfalls.2 11 Alongside inspection and accreditation, clinical audit is one of the main quality assurance mechanisms used by healthcare organisations.4 11 Clinical audit is effective for providing assurance of compliance with evidence-based standards – including national standards via national audits.
Clinical audit is one of the earliest forms of QI in healthcare. Whilst typically associated with quality assurance, clinical audit can play a key role across all quality management domains including planning, control and improvement. To provide confidence that care is consistently safe, effective and improving over time, clinical audit should underpin how we improve and monitor for proactive oversight and quality control.
References
- Department of Health & Social Care and NHS England. Fit for the future: 10 Year Health Plan for England. London: UK Government, 2025.
- NHS England. Clinical audits and registries: A best practice guide. London: NHS England (Available at https://future.nhs.uk ), 2026.
- Shah A. Using data for improvement. BMJ 2019;364:l189. doi: https://doi.org/10.1136/bmj.l189
- Backhouse A, Ogunlayi F. Quality improvement into practice. BMJ 2020;368:m865. doi: https://doi.org/10.1136/bmj.m865
- Berwick D. Continuous Improvement as an Ideal in Healthcare. New Engl J Med 1989;320(1):53-56. doi: https://doi.org/10.1056/nejm198901053200110
- Ivers N, Foy R. Audit, Feedback, and Behaviour Change. Cambridge: Cambridge University Press, 2025.
- HQIP. Best practice in clinical audit. London: Healthcare Quality Improvement Partnership (Available at www.hqip.org.uk ), 2020.
- Dixon-Woods M, Martin GP. Does quality improvement improve quality? Future Hospital Journal 2016;3(3):191-94. doi: https://doi.org/10.7861/futurehosp.3-3-191
- Spela Godec MH, John Illingworth, Carl Macrae. Developing whole-organisation Quality Management Systems in health care: learning from practice and recommendations for progress. London: The Health Foundation, 2025.
- Glassborow R. Moving from Quality Improvement to Quality Management: Supporting better quality health and social care for everyone in Scotland. Edinburgh, UK: Healthcare Improvement Scotland (Available at www.ihub.scot ), 2022.
- Shah A. How to move beyond quality improvement projects. BMJ 2020;370:m2319. doi: https://doi.org/10.1136/bmj.m2319
- Clark CI. Healthcare data: The key to improvement and efficiency [Blog]. London: BMJ Leader; 2025 [updated 03 Dec 2025. Available from: https://blogs.bmj.com/bmjleader/2025/12/03/healthcare-data-the-key-to-improvement-and-efficiency-by-dame-celia-ingham-clark accessed 19 Jan 2026 2026.
- MBRRACE-UK. Maternal mortality 2022-2024 Oxford: National Perinatal Epidemiology Unit; 2026 [updated 15 Jan 202627 Jan 2026]. Available from: https://www.npeu.ox.ac.uk/mbrrace-uk/data-brief/maternal-mortality-2022-2024.
- NHS England. The Maternal Care Bundle: A care bundle for reducing maternal mortality and morbidity London: NHS England; 2026 [updated 16 Jan 2026. Available from: https://www.england.nhs.uk/long-read/the-maternal-care-bundle/ accessed 26 Jan 2026.
- National Audit of Inpatient Falls (NAIF). Stepping towards improvement: an analysis of 2024 inpatient falls audit data and reflection on 6 years as continuous audit. London: Royal College of Physicians (Available at https://www.rcp.ac.uk/86396 ), 2025.
- Universities of Leeds and Leicester. The Paediatric Intensive Care Audit Network (PICANet): PICANet; 2026 [Available from: https://www.picanet.org.uk accessed 27 Jan 2026.
Author

Iain Smith
Iain is an Associate Director for the Association for Clinical Audit and Registries at HQIP the Healthcare Quality Improvement Partnership. With over 25 years of experience in the English NHS in national, regional and local roles, Iain is an experienced senior leader with a nationally established reputation in the field of healthcare quality improvement. Iain is a mathematics graduate and holds postgraduate qualifications in research methods and transformational change as well as a PhD in healthcare quality improvement. Iain also undertakes visiting academic work and is an Associate Editor for the BMJ Leader journal.
Declaration of interests
I have read and understood the BMJ Group policy on declaration of interests and declare the following interests: I am an Associate Director with HQIP and a member of the Editorial Board of BMJ Leader.
HQIP is an independent, not-for-profit long-term partner of the NHS responsible for commissioning and managing the National Clinical Audit and Patient Outcomes Programme (NCAPOP).