This week’s blog is written by Dr Judith Benbow, Senior Lecturer, Cardiff University, Professor Danny Kelly, Royal College of Nursing Chair of Nursing Research, Cardiff University and Professor Aled Jones, University of Plymouth.
Nurses seek help from other nurses as their primary coping strategy. Notwithstanding patients’ needs for more nurses, crucially nurses need more nurses for their resilience and wellbeing, now more than ever during this intractable workforce crisis.
Radical workforce reform is required to keep and support current nurses1. Despite the growth in nursing numbers, The Nursing and Midwifery Council (NMC) report that nurses are continuing to leave the profession early in droves2. Burnout, ill health, lack of support from colleagues, concerns about patient care, workload, staffing and work-life balance continue to be the main reasons for leaving cited. These data reflect the extant evidence on the exposure of nurses to pressurised workplaces with sub optimal staffing and the dire consequences on staff morale which can negatively affect patient care.
Resilience?
The American Psychological Association3describes resilience as the process and outcome of successfully adapting to difficult or challenging life experiences, especially through mental, emotional, and behavioural flexibility and adjustment to external and internal demands. A buffer of stress, resilience may positively influence the wellbeing of nurses. Supportive relationships and social networks are core to resilience, to gain support, learn strategies and engender a sense of belonging. A core human need, belonging is needed for nurses and midwives to flourish and thrive in work4.
Resilience is a contested topic in nursing. This is partly due to the spotlight has predominantly been upon the individual nurse and their ability to cope with stress, in so doing viewing it separately from the workplace and how the environment can provide support to sustain it. Resilience is a capacity that can help nurses manage occupational stressors, built from exposure to occupational adversity 5. Understanding the role of positive workplace factors are key to its enablement, underpinned by strong supportive relationships. Resources being one of the core workplace factors, in particular the people we work with, for nurses this means other nurses.
“Nurses” as a resource for other nurses’ resilience
In contrast to other workforce research, Benbow’s study5 was interested in “nurses” as a resource for other nurses’ resilience consistent with a social-ecological stance that views resilience as both an individual and an environmental asset. The pre-pandemic study explored the perceptions of resilience and workplace environments in a substantial sample of nurses (n=1459) across Wales. The nursing workforce shortfall dominated the findings, appeared to be the root of the problem and showed how the shortfall can hinder resilience in three multilevel ways.
First, increases in workload can drain personal and team reserves, leading to vicious circles of fatigue and stress which can affect professional functioning and is unsustainable.
Second, the interactions between nurses to build resilience can suffer. More time is needed to not only care for patients, but colleagues and themselves. The most helpful workplace resource was a conversation with a trusted colleague. Furthermore, the most frequent coping strategy that these nurses reported was receiving team support. Some teams were able to be offer more support than others.
Finally, the collective resilience of the environment as a shared asset for all to benefit can be reduced by sub-optimal staffing. This means that a progressive process of increased risk and vulnerability can be potentiated for the nurse, organisation, and workforce more broadly. It was found that these nurses did not necessarily want to change their work per se but more nurses could help their resilience. Despite the most adverse situations it was found that nurses can respond in a resilient way.
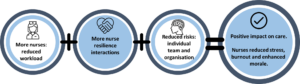
This evidence adds weight to the imperative for keeping and supporting current nurses and the links between adequate numbers and nurse wellbeing6. Furthermore, nurses new to any environment require support, which can impact on the resilience of existing nurses. The figure below simply depicts how situating nurse resilience in a wider workplace context, highlights how the combined potential of nurses shared resilience can influence the health and wellbeing of nurses for the benefit of all.
Call to arms
Radical workforce reform is required to address the shortfall and support nurse resilience so that nurse wellbeing is not sacrificed for patient care. Supportive relationships cannot be left to chance prioritisation of protected space and time is required in workforce projections not solely workload demands. This is a call to the new government, and all those who influence the nursing workforce and workplace to make nurse resilience and wellbeing a top priority. Nurses need nurses.
The author of this blog is a member of the International Network for Health Workforce Homepage | International Network for Health Workforce Education (inhwe.org)
References
- Twycross A. 2023. Our Nurses, Our Future: No more rhetoric, its time for action Evidence Based Nursing Blogs BMJ Our Nurses, Our Future: No more rhetoric, it’s time for action – Evidence-Based Nursing blog (bmj.com) [ Accessed 19th July 2024]
- Nursing and Midwifery Council. 2023. Registration Data Reports. Available at Registration data reports – The Nursing and Midwifery Council (nmc.org.uk) [Accessed 19th July 2024].
- American Psychological Association (APA) 2023. Building your resilience Available at: APA Dictionary of Psychology [Accessed 19th July 2024]
- West M, Bailey S, & Williams E. 2020. The Courage of Compassion: supporting nurses and midwives to deliver high quality care. UK The Kings Fund https://www.kingsfund.org.uk/publications/courage-compassion-supporting-nurses-midwives [Accessed 19th July 2024] Google Scholar
- Benbow J. 2022. Exploring Contemporary Nurse Roles in Wales a Mixed methods study Available at -ORCA (cardiff.ac.uk) [Accessed 19th July 2024].
- Maben J, Ball J, & Edmonson AC. 2023. Workplace Conditions (elements of improving quality and safety in Healthcare). In: The great Big Book of Quality Improvement This Institute doi:10.1017/9781009363839 Google Scholar