Roberta Heale, Deputy Editor for Social Media for EBN, @robertaheale, @EBNuringBMJ
The first blogs written for EBN in 2012 were about the use of evidence in practice. In fact, the inaugural blog described that although evidence-based nursing is the standard of our care, there are many barriers, some of which include difficulty finding, or lack of time searching for research evidence; evaluation of the quality of evidence; and struggles implementing the evidence. The blog also identified that there were many clinical circumstances where there is a lack of evidence. COVID-19 has challenged us, especially when it comes to evidence-based nursing which is focused not only includes provision of the best possible care to patients, but also in protecting ourselves from the virus.
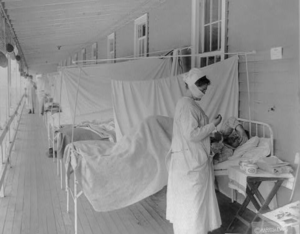
photo credit https://www.loc.gov/item/2016648028/
If you look for information about evidence based practice, you’ll find articles outlining anywhere from 3 to 7 possible principles arising from many different disciplines. However, some key principles help us to understand evidence based practice. Formal use of evidence in practice was originally conceptualized in medicine and was defined as “… integrating individual clinical expertise with the best available external evidence from systematic research.”(1) Principles arising from EBM are: to clearly define the problem, search the literature for relevant research evidence, evaluate the quality of the research and choose interventions that reflect the most relevant, best quality of evidence. Evidence based nursing takes this further by adding more consideration of patient values and availability of adequate evidence. (1)
Although there is a massive amount of information about COVID 19, there aren’t a large number of quality research studies. Many observational studies have been released, which help to guide us. However, science is still trying to determine even basic things like the possibility of spread through aerosol as well as droplets. Organizations release guidelines and protocols based on the best that we know at this time. However, concerns arise when policies aren’t congruent with evidence.
EBN blog July 19, 2020 by Dr. Evelyn McElhinney @evmcelhinney COVID19 Infodemic – A Tsunami of Health Literacy Issues outlined the difficulty in sorting through information about COVID 19 to find the best evidence for practice. She described the huge amount of information ranging from research articles and trusted, organizational sources to ‘fake news’, rumors and conspiracy theories. She cautions us to be wary of what we read to determine the veracity of it and then to consider the quality of the evidence. The issue, of course, is the enormous amount of evidence available that one has to sort through.
We can’t forget patient’s role in the equation. Our patients have the internet, but may not seek out reputable sources and their values and beliefs are not always congruent with best evidence. How do you manage this, especially if their values conflict with the best evidence to date and may put you, and others, in harm’s way?
There are lessons for us from nursing in the past. The flu pandemic of 1918-1920 came at a time when health care was just starting to embrace germ theory and when there were no treatments or medications to alleviate symptoms or secondary bacterial infections. Nurses practiced with the evidence that was known…hand washing, especially betweenpatients, isolation of infected individuals, use of protective equipment, such as masks, to reduce their own infections. In fact, nursing knowledge about aseptic techniques and implementation were more advanced than physicians at the time (3) Nursing practice worked. “After all, during the pre-‘miracle drug’ years, hospital wards were not ravaged by cross-infections, nor were surgical patients afflicted with postoperative infections”(4)
Until we know more, nurses should cling to historical evidence to guide their practices. Evidence that reflects an understanding of the spread of infection and how this is prevented is the current gold standard. We’re also put in a position to advocate for those who are expected to put themselves at risk, through organizational policies and employer expectations. We should look to the past to guide our current practice.
1. Mays, T. (2020). Evidence Based Practice (NUR 4169): What is EBP? https://fgcu.libguides.com/EBP
2. McElhinney, E. (2020). A Tsunami of Health Literacy Issues. https://blogs.bmj.com/ebn/2020/07/19/covid19-infodemic-a-tsunami-of-health-literacy-issues/
3. Barry, J. (2005). The Great Influenza. The Story of the Greatest Pandemic in History. Penguin Publishing Group
4. McPherson, K. (2012). Beside Matters. The Transformation of Canadian Nursing, 1900-1990. University of Toronto Press.