Gill Wilson – Lecturer in nursing, University of Hull

The concept of personalised care and support planning has been championed in health policy as a means of achieving person-centred care for people with long-term conditions (LTCs) (Department of Health (DH), 2006; DH, 2008; Coulter et al., 2015). It is a collaborative approach that seeks to determine what is important to patients and align their preferences with medical care through shared decision-making. The process is cyclical and involves goal setting, developing an action plan and monitoring progress, thus ensuring services are responsive to the needs of patients as individuals (Edwards et al., 2017).
It is important to distinguish between the action of ‘care planning’ described above, and the outcome of a ‘care plan’ (a written or electronic record documenting the plan of care). The care plan should be an active document that is available to the patient and other professionals involved in their care, referred to in each encounter, and evaluated over time (Burt et al., 2014; Edwards et al., 2017).
Most nurses are accustomed to care planning, but the concept in LTCs management is different to the traditional, usually reactionary, nursing care planning. Personalised care and support planning requires skills in shared decision-making, behaviour change, coaching, goal setting and action planning. Nurses and other health professionals involved in this process need training to develop these skills, which can be difficult to accommodate in a busy health care setting. For this reason Health Education England has been urged to work with health professional regulatory bodies to ensure that key components of person-centred care, including personalised care and support planning, are embedded in curricula (Coulter et al., 2013).
Several useful guides are available to aid health and social care practitioners in the care planning process, including NHS England’s Personalised Care and Support Planning Handbook, a Personalised Care and Support Planning Tool by the Coalition for Collaborative Care, and the Royal College of General Practitioners Collaborative Care and Support Planning Toolkit.
Primary care teams are faced with the responsibility of making personalised care and support planning happen. To implement it successfully and meet the needs of people living with LTCs a significant cultural change is needed in the way that health care is delivered. Built on the ideas of the innovative Year of Care project and the influential Chronic Care Model (Wagner et al., 1996), the House of Care model has been adopted by NHS England. Although directed mainly at primary care, it is based on the whole system approach. The defining feature of this model is that the patient is placed firmly in the centre, with care coordinated through personalised care and support planning. Another key feature of the model is the interdependence of the four structural components: the two walls, foundations and roof, as without this infrastructure patient-centred coordinated care will not be realised.
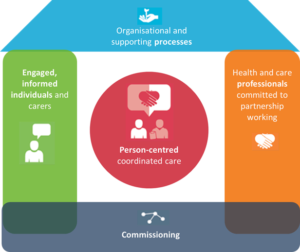
Source: NHS England https://www.england.nhs.uk/ourwork/ltc-op-eolc/ltc-eolc/house-of-care/
Provision of personalised care and support plans for people with LTCs has been slow to implement. In 2008, Lord Darzi pledged that everyone in England with one or more LTC should be offered a personalised care plan. This was further endorsed by the government’s mandate to NHS England that stated by 2015 “everyone with long-term conditions, including people with mental health problems, will be offered a personalised care plan that reflects their preferences and agreed decisions”. Considering that almost 30% of the population in England have at least one LTC, the provision of a care plans for 15 million people by 2015 was an ambitious task.
Almost a decade on from Lord Darzi’s pledge, a 2017 General Practice Patient Survey reported that only 3% of people with LTCs were aware of having a written personalised care and support plan. Similar findings were reported in an earlier study that evaluated the implementation of care planning in England. Many patients did not know what the term ‘care planning’ meant and only 12% of patients were aware of having a written care plan. However, 84% of patients reported having a care planning conversation, although important components of goal setting and action planning were often missing in those discussions (Burt et al., 2012; Newbould et al., 2012).
A trial by Kennedy et al. (2014) offered some insight into why self-management support practices such as personalised care and support planning were slow to be adopted. Staff felt they already provided effective care and that personalised care and support planning did not fit with their existing biomedical priorities. Furthermore, some staff downgraded the importance of offering self-management support to people with LTCs and did not feel it was part of their role.
Until recently, empirical evidence supporting personalised care and support planning has been limited, which may account for the inertia towards implementation by clinicians. However, a recent Cochrane Review found that personalised care and support planning made small but positive improvements in aspects of physical and psychological health, and can support people with LTCs with self-care practices and increase levels of self-efficacy (Coulter et al., 2015).
Implementing personalised care and support planning for adults with LTCs is easier said than done. The process is complex and challenging for both patients and health professionals, and requires a fundamental shift from reactive care to proactive care planning. One size certainly does not fit all when it comes to LTC management; however, evidence suggests that personalised care and support planning has a key part to play in the health professional’s armamentarium for supporting person-centred care.
References
Burt, J., Rick, J., Blakeman, T., Protheroe, J., Roland, M. & Bower, P. (2014) Care plans and care planning in long-term conditions: A conceptual model. Primary Health Care Research and Development, 15(4), 342-354.
Burt, J., Roland, M., Paddison, C., Reeves, D., Campbell, J., Abel, G. & Bower, P. (2012) Prevalence and benefits of care plans and care planning for people with long-term conditions in England. Journal Of Health Services Research & Policy, 17 Suppl 1, 64-71.
Coulter, A., Entwistle, V. A., Eccles, A., Ryan, S., Shepperd, S., Perera, R., Coulter, A., Entwistle, V. A., Eccles, A., Ryan, S., Shepperd, S. & Perera, R. (2015) Personalised care planning for adults with chronic or long-term health conditions. Cochrane Database of Systematic Reviews(3), N.PAG-N.PAG.
Coulter, A., Roberts, S. & Dixon, A. (2013) Delivering better services for people with long-term conditions: building the house of care. London: King’s Fund.
Department of Health (2006) Our health, our care, our say: a new direction for community services. London: Office, T. S.
Department of Health (2008) High quality care for all: NHS next stage review final report. London: The Stationary Office,.
Edwards, S. T., Dorr, D. A. & Landon, B. E. (2017) Can Personalized Care Planning Improve Primary Care? JAMA: Journal of the American Medical Association, 318(1), 25-26.
Kennedy, A., Rogers, A., Chew-Graham, C., Blakeman, T., Bowen, R., Gardner, C., Lee, V., Morris, R. & Protheroe, J. (2014) Implementation of a self-management support approach (WISE) across a health system: a process evaluation explaining what did and did not work for organisations, clinicians and patients. Implementation Science, 9(1), 129.
Newbould, J., Burt, J., Bower, P., Blakeman, T., Kennedy, A., Rogers, A. & Roland, M. (2012) Experiences of care planning in England: interviews with patients with long term conditions. BMC Family Practice, 13(71).
Wagner, E. H., Austin, B. T. & Von Korff, M. (1996) Organizing care for patients with chronic illness. The Milbank Quarterly, 74(4 ), 511-544.