Angela Teece (A.M.Teece@leeds.ac.uk). Trainee Lecturer in Adult Nursing, University of Leeds
I recently left clinical practice, where I had worked as a critical care sister in a large district general hospital, to undertake a university role. Stepping back from practice and reading recent legislation on the deprivation of liberty (DoLS), enabled me to reflect on how the care I provided to patients could be viewed as restrictive.
Deprivation of liberty could relate to:
- Is the patient under close supervision?
- Is the patient free to leave the clinical area?
Clearly, on this level, all critical care patients, and many patients on general wards, are being deprived of their liberty. DoLS guidance is supported by the 2005 Mental Capacity Act (MCA) in its definition of restraint. This can be physical, chemical or verbal, for example, the use of bed rails restricts patient mobility, and regulated visiting times and controlled entry to the unit reduce opportunities for the patient to interact with their family.
Critical care is a specialised area of practice. Patients are commonly sedated to enable tolerance an endotracheal tube, ventilator and multiple vascular access devices. Each of these things, although used in the patient’s best interest, could be considered a form of restraint under the MCA and DoLS. Physical restraints in the form of ‘boxing gloves’ may be used to prevent agitated patients interfering with life-saving treatment (Happ, 2000) and chemical restraint may also be used to control agitation (Hofso and Coyer, 2007).
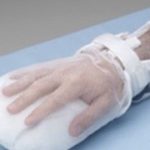 On reflection, I believe nurse are generally tasked with applying restraints, either by putting ‘boxing mitts’ on an agitated patient, or by administering at their discretion as required medication. Nurses must be able to justify their actions. Any restrictive intervention must be in the patient’s best interests and decisions can only be made for a patient if they lack capacity (MCA, 2005). Nurses should fully assess the need to restrain their patient using a validated tool, and conduct reassessment regularly whilst maintain their patient’s dignity whilst restraints are being used. Links have been made to patient experience of critical care and long-term psychological problems such as post-traumatic stress disorder (Jones et al., 2001). Rigorous nursing documentation, completion of DoLS referrals and regular patient observation and evaluation are vital to prevent prolonged restrain and promote patient dignity.
On reflection, I believe nurse are generally tasked with applying restraints, either by putting ‘boxing mitts’ on an agitated patient, or by administering at their discretion as required medication. Nurses must be able to justify their actions. Any restrictive intervention must be in the patient’s best interests and decisions can only be made for a patient if they lack capacity (MCA, 2005). Nurses should fully assess the need to restrain their patient using a validated tool, and conduct reassessment regularly whilst maintain their patient’s dignity whilst restraints are being used. Links have been made to patient experience of critical care and long-term psychological problems such as post-traumatic stress disorder (Jones et al., 2001). Rigorous nursing documentation, completion of DoLS referrals and regular patient observation and evaluation are vital to prevent prolonged restrain and promote patient dignity.
Happ, M.B. 2000. Preventing treatment interference: The nurse’s role in maintaining technologic devices. Heart & Lung: The Journal of Acute and Critical Care. 29(1), pp.60-69.
Hofso, K. and Coyer, F.M. 2007. Part 1. Chemical and physical restraints in the management of mechanically ventilated patients in the ICU: contributing factors. Intensive Crit Care Nurs. 23(5), pp.249-255.
Jones, C., Griffiths, R.D., Humphris, G. and Skirrow, P.M. 2001. Memory, delusions, and the development of acute posttraumatic stress disorder-related symptoms after intensive care. Critical Care Medicine. 29(3), pp.573-580 578p.
