Amelia Swift (@nurseswift) is a senior lecturer in nursing at the University of Birmingham and an associate editor of Evidence Based Nursing.
The world has experienced many devastating epidemics and pandemics in recent history. There have been three previous influenza pandemics in the 20th Century in 1918, 1957 and 1968. The 1918 pandemic caused the death of approximately five percent of the world’s population (1), with bacterial superinfection contributing to the high mortality rate (2). The 1957 H2N2-type virus proved fatal even without bacterial coinvaders (3). Between these two pandemics much progress was made in terms of recognising the responsible virus and developing vaccines. By 1957 there was a global network of laboratories linked to the World Influenza Research Centre in London, which acted as a hub for research and virus tracking (4). However, this cooperation did not help to stop that pandemic. It took five months for an epidemic first recognised in Hong Kong to spread across the globe. It was characterised by late and contradictory information and advice resulting from poor information and cooperation between government, physicians, scientists, and the media.
The current pandemic (Sars-Cov-2) is thought to have originated in Wuhan, China around the end of 2019. It was first reported to the World Health Organisation (WHO) is December 2019 and by mid-February cases were being reported across the world with Europe as the epicentre (5). There have been an estimated 13 million cases and more than half a million deaths (6) and accusations of the same failures in advice and decision-making that were made in the past have been levelled at governments and their advisors.
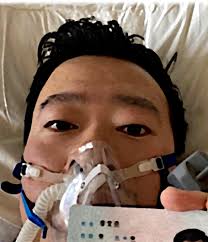
The lessons we should have learned relate to science, communication, co-operation, and ethics. One of the major differences between pandemics of the past and the present is that we have better vigilance and communication systems. It has been said that one of the things that allowed Sars-CoV-2 to spread so quickly across East Asia was a lack of transparency. The physician, Dr Li Wenliang, who first noted the novel disease in his patients was detained and charged with spreading false rumours. These charges were later dropped and he was exonerated but died of coronavirus disease in early February 2020 (7). Limiting spread and protecting the vulnerable can only happen if governments allow scientists to speak freely and promote effective communication and sharing of knowledge.
Governments too must communicate. It was not until March 2020 that global governments began to meet, and even then, a unified approach was not decided (8). Even closely neighbouring countries giving their populations very different advice. Approaches to reduction of transmission, and the seriousness with which the virus was regarded, led to lock-down in some places and open borders and movement in others. The most devastating early pandemics of cholera and bubonic plague coincided with imperialization and the advent of ocean travel (9). Since January 2020 WHO have advised that travel restrictions are only to be used as a short-term measure to allow countries time to prepare other measures such as quarantine and track and trace processes (10).
The different responses of countries to the pandemic is explored in a series of blogs collated by Dr Adam Oliver of the London School of Economics.. The blogs show that despite very different outcomes, the countries share some common ground in their rationale. There is a balance to be made between health and mortality on the one hand and economic consequences on the other. Countries differ quite markedly in terms of how willing the government is to be led by public opinion, and public willingness to comply with strict measures over the medium to long term. The example of Sweden is used to demonstrate a ‘soft’ approach based on trusting the public to cooperate. Authoritarian governments are more likely to institute strong interventions such as lockdowns. South Korea has been noted to have one of the most successful track and test regimes, able to test up to 20,000 people per day and providing results to them within 24-hours (11). This country is generally held up to be a success story. They were able to isolate those who were infected, providing support to them to increase compliance. They built temporary hospitals and drafted in large number of health care workers and used central government purchasing to address shortages of personal protective equipment (PPE). It is said that their rapid and effective response was directly due to lessons learned through their poor management of an outbreak of Middle-Eastern respiratory syndrome in 2015.
Lockdowns and social distancing in more liberal countries have often been resisted or ignored. The rationale is sometimes economic in the case of the factory boss who’s business is going under (12), sometimes it is moral and political in the case of mass protests in support of Black Lives Matter (13), and sometimes it seems to defy reason in the case of large numbers visiting coastal areas during a recent heatwave (14). There are myriad reasons for this resistance, not least among them conflicting reports about whether lockdown slows the spread of the virus (15,16). Science should be able to shine a light that guides decision-making, but public trust in science is fragile and has been easily rocked by relatively small challenges. One of the most dangerous to my mind is government interference in what is supposed to be an independent endeavour.
The lessons to be learned from this and other pandemics are extremely complex. Individuals and societies, government and laws, economics and resources are all in play. Public response suggests a desire for clear and irrefutable rules backed by hard and incontrovertible evidence. What we have learned from all of this is that evidence is never incontrovertible, and rules have so many exceptions that they are next to impossible to apply. Whatever we choose to do hurts someone. Our behaviour suggests we do not like rules and do not believe the evidence unless it suits us. How then will we learn our lessons?
1. Taubenberger JK, Morens DM. 1918 Influenza: the mother of all pandemics. Emerging Infectious Diseases 2006;12(1):15-22. doi: https://dx.doi.org/10.3201/eid1201.050979.
2. Kilbourne ED. Influenza pandemics of the 20th Century. Emerging Infectious Diseases 2006;12(1):9-14. doi: https://dx.doi.org/10.3201/eid1201.051254.
3. Rogers DE, Louria DB, Kilbourne ED. The syndrome of fatal influenza virus pneumonia. Transactions of the Association of American Physicians 1958;71:260-73.
4. Jackson C. History Lessons: the Asian flu pandemic. British Journal of General Practice 2009;59(565):622-23.
5. Forman R, Atun R, McKee M, et al. 12 lessons learned from the management of the coronavirus pandemic. Health Policy 2020;124(6):577-80.
6. Ritchie H, Ortiz-Ospina E, Beltekian D, et al. Coronavirus (Covid-19) deaths 2020 [Available from: https://ourworldindata.org/covid-deaths#what-is-the-total-number-of-confirmed-deaths.
7. Davidson H. Chinese inquiry exonerates coronavirus whistleblower doctor. The Guardian 2020 20 March 2020.
8. Blavatnik School of Government. Coronavirus government response tracker Oxford: University of Oxford; 2020 [Available from: https://www.bsg.ox.ac.uk/research/research-projects/coronavirus-government-response-tracker accessed 13/07/2020 2020.
9. Markel H. Contemplating pandemics: the role of historical inquiry in developing pandemic-mitigation strategies for the 21st century. In: Threats. IoMUFoM, ed. Washington (DC), USA: National Academies Press (US), 2007.
10. World Health Organisation. Updated WHO recommendations for international traffic in relation to COVID-19 outbreak: WHO; 2020 [Available from: https://www.who.int/news-room/articles-detail/updated-who-recommendations-for-international-traffic-in-relation-to-covid-19-outbreak.
11. Beaumont P, Connolly K. Covid-19 track and trace: what can the UK learn from countries that got it right. The Guardian 2020 21/5/2020.
12. Chaudhary V. Clothes factory bosses in Leicester vow to defy city lockdown because they cannot afford to lose any more money – even if it puts lives at risk. MailOnline 2020 1/7/2020.
13. Buchanan L, Bui Q, Patel JK. Black Lives Matter may be the largest movement in US history. NY Times (Print) 2020 3.7.2020.
14. Yeginsu S. Lockdown? What lockdown? Heat wave brings Britons out in droves. NY Times (Print) 2020 26.6.2020.
15. Meunier TAJ. Full lockdown policies in Western Europe countries have no evident impact on the COVID-19 epidemic. medRxiv 2020
16. Ghosal S, Bhattacharyya R, Majumder M. Impact of complete lockdown on total infection and death rates: a hierarchical cluster analysis. Diabetes and Metabolic Syndrome 2020;14(4):707-11.

