Background
The elephant in the room is a metaphorical idiom implying that an obvious issue has been left unaddressed. Our elephant is a challenging one. As Smith (2019) explained, 30 years ago the concept of interdisciplinary teams in professional sports care did not exist – and most likely, the appointed physiotherapist would provide the majority of required multi-faceted care. Smith (2016) previously presented that “Prior to 1990 there was no such thing as a sports therapist. This does not mean that anyone who participated in sport did not sustain injuries or receive primarily basic treatment from trainers, first aiders, physios and doctors. It does mean that, until that point, there was not a specific profession in the UK with its own clearly defined professional title, training, education and scope of practice, dedicated to sports and exercise therapy.” As both the professional care of elite sports performers and SEM itself have evolved, National Governing Bodies (NGBs) in sport have developed their medical provision frameworks (and medical handbooks) to clarify current regulations regarding which practitioners are required and accepted to work in their sport. In a most recent Society of Sports Therapists (SST) guested editorial issue of the BJSM Sports Therapists: An integral part of multidisciplinary teams Smith (2022) expands the reasoning for equitable recognition of GSTs.

Other recent contributions to the wider discussion include Ehiogu (2021) and Carolan et al. (2021) who offered (debatable) analysis of the seemingly insufficient attention paid to exercise rehabilitation within physiotherapy undergraduate and masters’ educational programmes. Carolan et al. (2021) proposed a consideration for sport rehabilitators in this discussion. We propose a greater and unbiased consideration to the appropriate inclusion and recognition of both GSTs and GSRs in elite sports settings. The complexity of our elephant is that there is a small and established set of comparable professions seeking to work with both athletic and non-athletic populations across a delivery continuum which incorporates everything from a diversity of roles in the NHS, to working in grass roots and elite level sport.
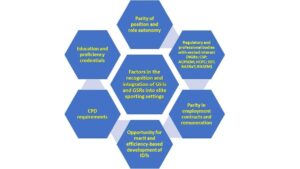
NGBs (National Governing Bodies in Sport); CSP (Chartered Society of Physiotherapy); ACPSEM (Association of Chartered Physiotherapists in Sports and Exercise Medicine); HCP (Health and Care Professions Council); SST (Society of Sports Therapists); BASRaT (British Association of Sport Rehabilitators); BASEM (British Association of Sport and Exercise Medicine); IDT (Inter-disciplinary Team); GST (Graduate Sports Therapist); GSR (Graduate Sport Rehabilitator); CPD (Continued Professional Development)
Analysis, Evidence and Experience
To date, a disparity still exists within current NGB medical regulations. We can go back to 1988 when the Football Association (FA) set up a group who recommended that therapists working in professional football had to be Chartered Physiotherapists. This was pragmatic and justifiable at the time due to physiotherapists seemingly having the skills, scope of practice, educational standards, and professional accreditation to fulfil the role. If we then fast forward to 2014, the updated FA medical regulations required clubs to employ at least one full-time physiotherapist as “senior physiotherapist”. Within the same medical regulations, it was stated, that “In exceptional circumstances, with prior permission from the head of FA medical services, football clubs may employ a Graduate Sports Therapist”. Such a statement offers some level of disregard to sports therapists, and with “prior permission” would require rigorous checks prior to gaining clearance. The current FA 2022 medical regulations state “the home club should have a registered member of the HCPC in attendance throughout matches”.
Current Rugby Football League (RFL) medical guidelines are similar to those of the FA. To work at the highest level of the super league “a sports therapist must be supervised by a physiotherapist, unless they can demonstrate one year’s full time or two-year part time supervised experience in a professional environment and any evidence should be submitted to the chief medical officer”. This highlights that those sports therapists must work under physiotherapists and are required to gain clearance from hierarchical members before gaining employability. In the lower levels of rugby and at part time clubs “home or away matches can be managed by a physiotherapist or equivalent.”
Thoughts and Proposals
It does now appear less likely that statutory regulation of sports therapists will be achieved as the Society of Sports Therapists (SST) applications have historically been supported by the Health and Care Professions Council (HCPC) but declined by the Government on several occasions. Smith (2019) suggested that formal recognition by sporting NGBs should be awarded to those Health Care Professionals (HCP) who have the definitive skills, knowledge and abilities required, along with appropriate qualifications and professional membership(s) for accountability. Such practitioners will most recognisably belong to either the Chartered Society of Physiotherapy (CSP) and Association of Chartered Physiotherapists in Sport and Exercise Medicine (ACPSEM), the Society of Sports Therapists (SST1) or the British Association of Sport Rehabilitators (BASRaT1). At qualification from an accredited programme, GSTs are deemed competent in a set of 5 core areas (prevention; recognition and evaluation; management, treatment and referral; rehabilitation; education and professional practice issues) (SST, 2012). In short, GSTs have a breadth of knowledge and skills that cover the athlete’s needs, and this also includes performance preparation, immediate injury care and return to sport-specific fitness. For professional practice, sports therapists or rehabilitators who are full and insured members of their respective professional body are required to uphold formal Standards of Proficiency and Standards of Conduct, Performance and Ethics which are wholly comparative to those required for HCPC membership, as well as maintain a specified profile of CPD.
It is pertinent to again highlight and agree that it should not be about the occupational title but rather be about the person who has the skills, knowledge and credentials to fulfil the job specifications. GSTs and GSRs emerge from an evolved and robust academic pathway which is built on a strong sports and exercise science foundation (Smith, 2022). There can be little doubt that each of the 3 central professional roles in discussion (GST, GSR and physiotherapist) can offer not only the required provision, but great value to the IDT sports employment setting, at any level. One only has to look at these organisations (SST1; SST2; BASRaT1; BASRaT2) and their members to appreciate the level of work and contribution they are able to offer. We recognise that there is a legitimate hierarchy to the organisational structure in any SEM environment, which absolutely should be lead by those with the highest credentials. However, we do propose that a fresher approach would be where opportunities are open to those with the appropriate qualifications, skills, experience and personal characteristics. In continuing the theme, we therefore politely call upon the relevant bodies (professional associations, societies and sporting NGBs) to factor this into the next rounds of formal planning for what could be a more innovative and flexible medical infrastructure in sports. It is essential that all those with vested interest keep up with the ever-evolving nature and requirements of elite sport alongside the educational pathways designed to prepare the practitioners for operating within this – and ensure that evidence-based athlete-centred care is at the forefront. As a side note, such developments may also deter some GSTs and GSRs from any unnecessary side-stepping of gaining post-graduate licence to practice physiotherapy qualifications. So, whilst we may remember that an elephant never forgets, we must also not forget the elephant.
References
Carolan, M., Prescott, E., Peil, C. and Aspinal, S. (2021) What about Sport Rehabilitators? https://blogs.bmj.com/bjsm/2021/06/04/sc-or-physio-who-are-the-real-exercise-professionals-what-about-sport-rehabilitators/?int_source=trendmd&int_medium=cpc&int_campaign=usage-042019
Ehiogu, U. (2021) S&C or Physio – who are the real exercise professionals? https://blogs.bmj.com/bjsm/2021/05/02/who-are-the-real-exercise-professionals-strength-and-conditioning-professionals-or-physiotherapists/
Smith, G.N. (2016) Foreword. In Ward, K. (Ed) Handbook of sports therapy, injury assessment and rehabilitation. Routledge, London.
Smith, G.N. (2019) Same label—different product: time to review the hiring criteria for therapists in sport. Br J Sports Med, 53:1514-1515.
Smith, G.N. (2022) Progress over 30 years should not mean principles have to change: a Society of Sports Therapists’ perspective. Br J Sports Med. 56:775
SST (Society of Sports Therapists) (2012) Standards of education and training. https://society-of-sports-therapists.org/
Authors and Affiliations:
- Ryan Conville BSc (Hons) Sports Therapy
LinkedIn: ryan-conville
- Keith Ward BSc MA MSST CIMSPA PCRMM FHEA
School of Health, Sport and Food, University College Birmingham
Twitter: @keithward01
Competing interests
None declared.