On Wednesday 18th November (8pm-9pm GMT) we are delighted to host our final #ebnjc tweet-chat of the year on person-centred care in nursing and healthcare with Professor Brendan McCormack.
Participating in the Twitter chat requires a Twitter account. If you do not already have one you can create an account at Twitter. Once you have an account contributing is straightforward – follow the discussion by searching links to #ebnjc or @EBNursingBMJ, or better still, create a tweet (tweets are text messages limited to 140 characters) to @EBNursingBMJ and add #ebnjc (the EBN chat hash tag) at the end of your tweet – this allows everyone taking part to view your tweets.
For further details on how participate in this twitter-chat please click here.
The concept of ‘person-centredness’ has become established in approaches to the delivery of healthcare and particularly within nursing. In the United Kingdom, person-centredness is embedded in many policy initiatives. Recent research into person-centredness has attempted to clarify the meaning of the concept, explore the implications of the term in practice and determine the cultural and contextual challenges to implementing a person-centred approach. Evidence from research suggests that adopting this approach to nursing provides more holistic care. In addition, it may increase patient satisfaction with the level of care, reduce anxiety levels among nurses in the long term, and promote team working among staff. Existing evidence is consistent in the view that being person-centred requires the formation of healthful relationships between professionals, service users, families and others significant to them in their lives and that these relationships are built on mutual trust, understanding and a sharing of collective knowledge. This evidence is also consistent with previous nursing literature on therapeutic caring where the concept of ‘person’ is central. The relationship between person-centredness and caring is strong and focuses on the centrality of concepts that are common to both, such as, relationships, values, caring processes and the environment of care (context). In a three year quasi-experimental research and development project to implement person-centred nursing across eight different clinical settings in an acute hospital setting, McCormack and McCance developed the ‘person-centred nursing theoretical framework’ (McCormack & McCance,2006 and 2010) and this has been further developed through a range of research studies into the Person-centred Practice Framework (McCormack & McCance, in press). The framework has been tested through a range of research projects internationally and the findings confirm its content validity, replicability, transferability and usability in practice.
The figure below is the new version of the Person-centred Practice Framework (McCormack & McCance) which is soon to be published in the 2nd edition of the book – Person-centred Practice in Nursing and Healthcare.
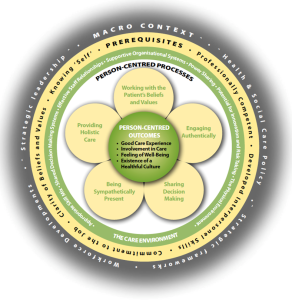
Since the publication of the person-centred nursing framework in 2008, the field of person-centred nursing and person-centred practice has developed and expanded significantly and has adapted to significant changes in health and social care models of service design and delivery. Particular health and social care advancements that need to be taken account of are:
- An increased ageing population with the associated rise in long-term conditions, resulting in the need for health and social care services to be remodelled and redesigned.
- The focus on integrated care and a more overt focus on primary care and public health.
- The global economic down-turn and the need for high quality services to be delivered in a fiscal environment.
- The central focus on public engagement in health and social care services and the development of services that are responsive to individual need.
- The ‘post-Francis’ era where there is a greater emphasis on compassion in care instead of business delivery targets.
- The global attention paid to patient safety and service improvement with some links being made to person-centredness.
- The evidence of person-centred principles underpinning health and social care policy, strategy and service-delivery models.
- The beginnings of a focus on person-centredness in curriculum frameworks for nurses and midwives.
- Significant development in methodologies for developing person-centred practices and process & outcome evaluation.
However, all of this research and theoretical development has not resulted in a large-scale shift towards person-centredness. The values of mutuality, collegiality and care that are espoused in mission statements and organisational frameworks are often not easily realised by staff in practice. Despite a large literature on teams, team-effectiveness and team-culture, dysfunctional team relationships and dissonance between espoused and lived management and leadership values continues to exist in nursing and healthcare. The key goal in the development of a positive learning culture is to recognise and overcome individual, group and organisational barriers in order to move towards an effective culture and overcome the features of workplaces that nurture hierarchical management and horizontal violence, as illustrated by the following poem:
Twenty years as a nurse,
Moving through the ranks knowing who I am
Knowing me
Becoming a manager, being a manager
Managing
Discovering the joys of person-centredness
Unfurling the challenges of being a person-centred leader
Self growth
Discovery
Transformation
The winds of change blow from the west
Person-centred leadership devalued
Targets
Bullying
Devaluing
I am an ‘It’
Stats mean good care
Shared experiences mean coercion
Get out get out get out
Stay safe
Shut down
Hide
But I need to keep listening to the patients
(poem written by a Clinical Leader, personal communication)
There is no doubt that for person-centred nursing to exist, there is a need for a work organisation method that enables nurses to exercise power whilst simultaneously being able to negotiate the nature of that power in relationships with others (including patients and families). The language of empowerment is pervasive in nursing and contemporary nursing policy and strategy espouses the importance of nurses being empowered to exercise autonomous decisions, whilst at the same time empowering patients. Various authors have argued that the language of empowerment is complex and challenging, that nurses aren’t empowered professionally or organizationally to exercise empowerment or to empower others. Organizations need to create and nurture the structural conditions in which clinical staff are enabled to facilitate empowerment.
Developing person-centred nursing requires a sustained commitment to the facilitation of multiple aspects of culture change in clinical settings and organisations. However, despite many examples of well-intentioned projects, it continues to be the case that embedding person-centredness in team, unit and organisational cultures is a challenge, and indeed often seems ‘elusive’ in the everyday (chaotic) world of practice. In addition, for some, the whole agenda of person-centred nursing is merely a buzz term or a process of ‘naming that which already exists’, i.e. “we are doing it anyway aren’t we?”. Others however may have identified issues and ideas that stimulate new ways of thinking about practice and are wondering “how do I move towards this way of nursing?” Both these positions pose challenges to the facilitation of person-centred care developments. What is clear, is that for person-centred nursing to be realised, a sustained commitment to its development and maintenance in practice is required from organisations.
The real challenge for all organisations is the movement from individual ‘person-centred moments’ to ‘person-centred cultures’. It is clearly evident from the international literature that this cannot happen by relying on the individual motivation of practitioners, but instead requires a sustained commitment to facilitated culture change with teams and across organisations.
See two of Professor McCormack’s talks below. The first, a TEDx talk called “In search of (my) personhood” and the second, a keynote speech from the 2013 International Nursing Research Congress called “From Person-centred Moments to Person-centred Care: Creating flourishing healthcare cultures”.
REFERENCES
McCormack B and McCance T (in progress) Person-centred Nursing and Health Care – Theory and Practice, Wiley Publishing, Oxford,
McCormack B and McCance T (2010) Person-centred Nursing: Theory, models and methods. Blackwell Publishing, Oxford.
McCormack B and McCance T (2006) Development of a framework for person-centred nursing. Journal of Advanced Nursing, 56(5): 1-8.
Professor Brendan McCormack,
Head of the Division of Nursing/Head of QMU Graduate School
School of Health Sciences
Queen Margaret University
Queen Margaret University Drive
Musselburgh
East Lothian
EH21 6UU
Email: BMcCormack@QMU.ac.uk
