Sport and Exercise Medicine: The UK trainee perspective (A BJSM blog series)
By Dr Jim Kerss
Why public health? Was a surprisingly common question asked of me when I explained to my friends, family and colleagues that I was working in Public Health as part of my Sport & Exercise Medicine training. Thus, my aim of this blog post is to share reflections and inform anyone interested or involved in SEM training of the benefits and opportunities of working in Public Health.
Local experience
SEM enthusiasts are well aware of both the mounting global public health crisis of physical inactivity and the evidence base behind physical activity as a preventative and treatment intervention for a range of diseases. I was keen to learn the extent to which these messages were filtering through to other medical specialities and if there was evidence of the development of local services to tackle the problem.
Under the brand of ‘Liverpool Active City’, work done by the Public Health department has contributed to a 3% increase in city residents being sufficiently active between 2005 & 2011, with an aim to achieve a 1% yearly rise until 2017. I have been involved in work to develop a physical activity treatment pathway for women with Breast Cancer and to improve the existing GP exercise referral scheme which will hopefully help to achieve these targets.
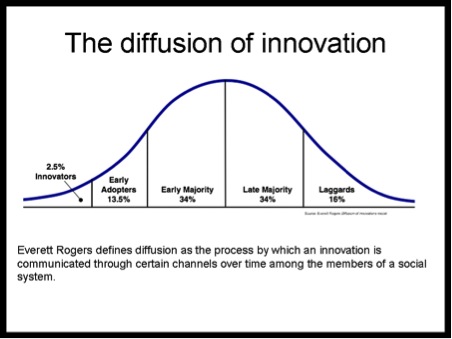
Clearly there is a great deal being done but we are still probably in the ‘Early Adopters’ phase of the law of diffusion of innovations meaning there is still more to do before physical activity becomes a cornerstone of healthcare in the UK. See TED talk by Simon Sinek on the subject.
National experience
I attended a NICE Public Health Interventions Advisory Committee meeting on Physical Activity advice in Primary Care. The analysis of evidence and cost-effectiveness was very robust but there was a lack of clinical input into the discussions which I feel could have been provided by a specialist in SEM. NICE accepts applications to join these committees to provide such expert guidance and are shortly due to commence the update of advice on exercise referral schemes.
In 2012 NICE also discussed adding indicators on recording physical activity levels in patients with hypertension to the QOF but these were rejected. I believe financial incentives could be a useful way of encouraging the recording of physical activity as a ‘vital sign’ in primary care. SEM specialists could use their expertise, and skills learnt in public health, in helping to develop national guidance that would encourage healthcare staff to discuss physical activity with their patients. An example of this already occurring is the RCP document ‘Exercise for life: physical activity in health and disease’.
NHS management
Given the current organisational changes in the NHS, and particularly as SEM is a new and developing speciality the exposure to NHS management, funding issues and experience of developing new services that can be gained through working in public health is invaluable.
Education
Working in public health has highlighted the importance of continuing to spread the messages behind physical activity through education of different groups – medical students, doctors in various stages of training and differing specialities, other allied healthcare staff as well as the general public. Public Health provides a good platform to be able to do this.
Final thoughts
Starting work in public health was actually quite daunting, with a sense of being out of my comfort zone in clinical medicine. Overall, it was a rewarding experience, that furthered my enthusiasm for SEM and my understanding of where the speciality will exist in the NHS in the future.
*****************************************************************
Dr Jim Kerss is a Speciality Trainee in Sport and Exercise Medicine in Liverpool
Dr James Thing co-ordinates “Sport and Exercise Medicine: The UK trainee perspective” monthly blog series.